VIDEO
Diabetic Insulin Pump Insertion
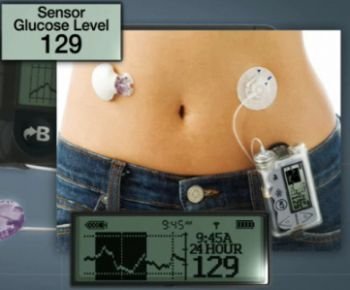
Insulin Pumps
I have heard about insulin pumps for treating diabetes. Doctors in my own clinic never seem very keen on the idea. How do pumps work and are they a good form of treatment?
First, an explanation of why insulin pumps have been developed. People who do not have diabetes release a very small amount of insulin into the bloodstream throughout the day and over the night. This insulin prevents the liver from releasing its glucose stock into the bloodstream. Whenever the glucose level rises after a meal the pancreas immediately produces extra insulin to damp the level down. This is a simple feedback system designed
to keep the level of blood glucose steady. Without the ‘background’ insulin in between meals, the level of blood glucose would slowly rise.
Insulin pumps are an attempt to copy this normal pattern. They consist of a slow motor driving a syringe or cartridge containing insulin, which is pumped down a fine-bore tube and needle. The needle is inserted under the skin and strapped in place. There is also a device for giving mealtime boosts of insulin. The modern pumps are about the size of a pager, and a microprocessor-based button allows a wide range of rate settings.
Many people have successfully controlled their blood glucose with an insulin pump. However, they are not currently available in the NHS, and they are very expensive to buy and run. They require extra blood tests and adjustments in the dose of insulin, but they can be a good way of achieving tight control of diabetes in people with a high degree of commitment. Since the introduction of insulin pens, pumps became less popular, but they are gaining favor in some centers.
My diabetes is well controlled. Should I be thinking of buying a pump?
Probably not, if your diabetes really is well controlled. Pumps are only used in a small number of diabetes clinics throughout the UK, although their use is becoming more widespread.
Currently approximately 0.1% of people with Type 1 diabetes in the United Kingdom use pumps, compared with about 5% in the USA, the Netherlands, Sweden, Germany and Norway. Pump therapy is not suitable for all people with diabetes. From discussions with
healthcare professionals, pump users and manufacturers, the people most suited to using pumps must be well motivated and willing to take control of their diabetes, have a good knowledge and understanding of their diabetes, and be prepared to test blood glucose levels at least four times a day and be able to act on those results.
NICE (National Institute for Clinical Excellence), a government body which assesses the value of new forms of treatment, has reviewed the clinical and cost effectiveness of insulin pump therapy. They will report their findings soon. They may recommend that, under certain circumstances, pumps should be funded by the NHS – this would provide a welcome boost to this method of giving insulin.
Research has shown that, if you are the sort of person who achieves good control by giving insulin with modern insulin regimens, then you would probably be able to do slightly better using a pump but, if your control is normally erratic, then equipping you with a pump is not likely to improve matters.
What are the main difficulties of using a pump for giving insulin?
The main problem with pumps is that, like all machines, they are capable of going wrong. One reason for the high cost of insulin pumps is the need to build a warning system into the design to alert the user to a mechanical fault. If the pump suddenly stops, the user will rapidly go into a state of complete insulin lack and may quickly develop ketoacidosis. Also, because the needle remains under the skin it acts as a foreign body and may set up a focus of infection leading to an abscess.
The needle must be inserted only after careful cleaning of the skin and must be replaced every 2 days. From the user’s point of view, the main disadvantage of the pump is the act that it has to be worn day and night.
This is obviously less convenient than the ordinary injections, which are over and done with. Many people dislike the pump because they find it to be a constant reminder of their diabetes.
How can I obtain an insulin pump?
The first thing to do is to discuss the use of the pump with your diabetes specialist. If they feel that you are a suitable candidate, but they have little experience with pumps themselves, they may need to refer you to another centre. Pumps are not currently available on the NHS, and at the moment (see previous questions) United Kingdom funding for pump treatment is met by a mixture of local charities, purchase by people with diabetes themselves, research trials and private donations to hospitals. At the time of writing there are two manufacturers supplying pumps in the United Kingdom.
The Disetronic H-Tron pump has a programmed 2 year lifetime. The Minimed model 505 has a single basal rate, and the model 507 has multiple basal rates. Minimed pumps and supplies can be obtained from their distributor, Applied Medical Technology. These pumps are estimated to have a lifetime of 7 years.
All pumps are very expensive to buy and they have weekly running costs. Both Disetronic and Applied Medical Technology have nurse educators who will initiate pump treatment either at the diabetes centre or in the home. Both AMT and Disetronic state that they will only supply pumps and instruct people with the close cooperation of the doctor managing the client’s diabetes.Diabetes United Kingdom will have details on pumps as well.