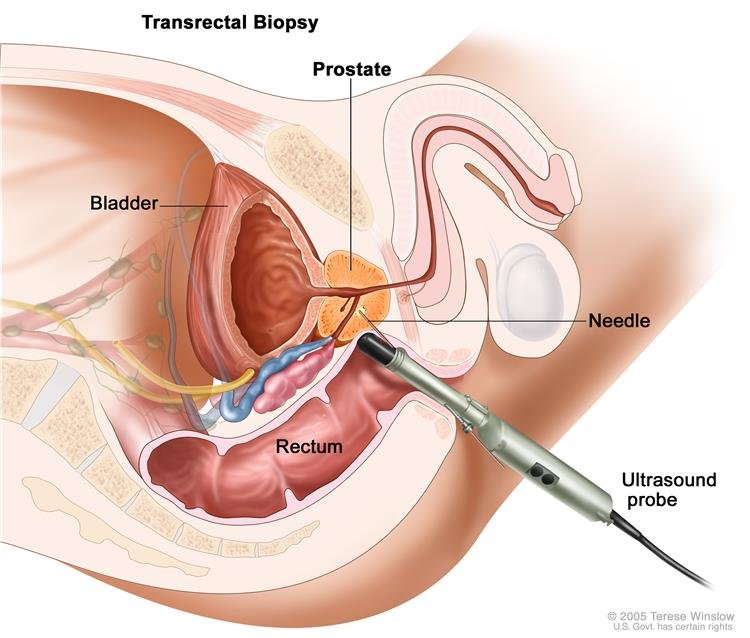
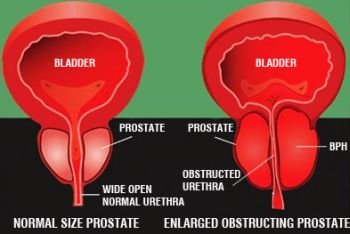
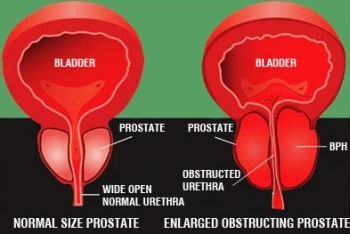
Prostate Enlargement Causes and Symptoms & Home Remedy Treatment for Prostate Disorder
Surgical Treatment of Benign Prostatic Hypertrophy
What is electrovaporization of the prostate?
Electrovaporization of the prostate (TUVP) is, in a sense, a derivation of TURP.Rather than a resecting loop, the urologist uses a “roller ball” to heat and desiccate the prostate instead of actually resecting tissue. Electrovaporization of the prostate has been most often applied in patients with a history of bleeding disorders or in cases in which it is desired to minimize blood loss. Electrovaporization of the prostate tends to be used in patients with small- and medium-sized glands. Like TUIP, in properly selected patients, it is an alternative to TURP.
What are the side effects of surgical treatment of BPH?
The side effects associated with TURP can be divided into intraoperative and postoperative complications. A TURP is performed under either spinal or general anesthesia, and the usual complications that are associated with these forms of anesthesia can occur during a TURP. The introduction of either spinal or general anesthesia can result in hypotension or a drop in blood pressure.
Bleeding can occur with a TURP, and it is correlated with the size of the prostate and the duration of the operation; however, it should be emphasized that significant bleeding is uncommon when an experienced urologist performs the TURP. Extravasation or perforation of the prostate can occur during a TURP. This causes some of the irrigation fluid used during a TURP to extravasate or leak outside the prostate. If the patient is awake under spinal anesthesia, this can result in nausea, vomiting, or abdominal pain. Most often, this complication can be managed by cessation of the operation and urethral catheter drainage. As with bleeding, extravasation in the hands of an experienced resectionist is uncommon. The most dramatic complication that occurs intraoperatively or in the immediate postoperative period is the so-called TUR syndrome. In order to enable the urologist to see during a TURP, and for transmission of the electrical current, a somewhat dilute or hypotonic irrigation solution known as glycine is used during the TURP procedure. Variable amounts of the glycine are absorbed during a resection, depending on the amount of bleeding and length of time associated with the operation. Because of systemic absorption of relatively dilute fluid, some patients can develop a condition known as dilutional hyponatremia (low sodium) or the TUR syndrome. The manifestations of the TUR syndrome include nausea, vomiting, brachycardia or slow heart rate, and visual disturbances. The treatment of the TUR syndrome is principally diuretic medications, which help the patient urinate out the excess fluid that has been absorbed. Some urologists will also give hypertonic saline or high concentration sodium solutions to increase the serum sodium. In most circumstances, the TUR syndrome can be corrected in the immediate postoperative period. In the postoperative period, a very rare patient will continue to bleed after a TURP. The initial management is to replace the blood loss with appropriate blood transfusions and to increase the irrigation fluid that is used to irrigate the bladder through what is known as a three-way urethral catheter. Despite these maneuvers, some patients continue to bleed and require a return to the operating room to fulgurate (burn) the bleeding points present in the prostatic urethra.
What are the results of surgical treatment of BPH?
The TURP is a commonly done surgical procedure that urologists have performed for decades. It is a reliable method to relieve obstructive urinary symptoms. As mentioned previously here, complications associated with TURP can occur. Recent studies report that blood transfusions are required in about 4% of the patients who undergo the procedure. Because the apex of the prostate is near the external urinary sphincter, incontinence is a potential complication. Fortunately, the risk of urinary incontinence after a TURP has been estimated to be about 1%. Erectile dysfunction or impotence can occur after a TURP. It is theorized that some of the electrical current from the resectoscope loupe scatters beyond the prostate capsule and injures the nerves.
JN: Is there a way to preserve ejaculation after a TURP?
KL: There is a technique called “a bladder neck preserving TURP,” which in some cases can preserve ejaculation after a TURP.
What is minimally invasive surgical treatment of BPH?
Even though open prostatectomy and TURP, TUIP, and TUVP have been commonly performed, reliable operations, urologists have sought procedures that are less invasive and easier on the patients. These procedures have become known as minimally invasive surgical treatment (MIST) of BPH. These MIST techniques include laser procedures, hyperthermia and thermotherapy, radiofrequency ablation, balloon dilation of the prostate, urethral stents, and high-intensity focused ultrasound.
JN: If a man has a TURP, TUIP, or TUVP and finds that his prostate continues to enlarge even with two-medication therapy, is minimally invasive or other surgery now something that should be considered?
KL: Yes, these should be considered if medical therapy has failed.
What is laser therapy of the prostate?
Over the past 20 years, several generations of lasers have been used to treat obstructive prostate symptoms. LASER is an acronym for light-amplification stimulated emission resonance. In practical terms, this means that the light energy is very focused and allows powerful and precise application of the light energy to tissue. The potential advantages of laser therapy include minimal bleeding, avoidance of TUR syndrome, less retrograde ejaculation, the ability to treat anticoagulated patients, and the potential to treat patients on an out-patient basis. We now review the various lasers that have been used to treat BPH.
What types of laser therapy are available?
Multiple types of lasers have been used throughout many areas of medical practice. In urology, several types of laser technology have been applied to the treatment of BPH. When considering whether laser therapy is appropriate for his prostate symptoms, it is important for the patient to have a thorough discussion with his urologist about the treatment options and which laser will be used and why. Not every urologist or every hospital has access to every laser that is on the market. Lasers that are used for the treatment of an enlarged prostate have different characteristics. They have different methods of delivery, emit different wavelengths of light, and have variable tissue effects. Several types of laser delivery systems have been used to treat prostate enlargement, including side-firing lasers, contact lasers, and interstitial lasers. In addition, lasers of variable wavelength have also been used in the treatment of BPH.
Laser applications to the treatment of BPH are still evolving, and no single laser type has gained preeminence. A new development in laser technology is the Green Light PVP laser. This laser has a wavelength of 532 nm and has a thermal coagulation depth of 1 to 2 mm. Early studies suggest that this laser in particular may be a very good option to a TURP. The Holmium:YAG laser is also emerging as an attractive laser alternative for the treatment of BPH. The Holmium:YAG laser operates in a pulsed mode in the near infrared area of the electromagnetic spectrum at a wavelength of 2140 nm. Its tissue absorption distance is 0.4 mm.
What are the results of laser therapy?
Many series reporting laser treatment of BPH suffer because they have no control group and have a short follow-up; however, laser therapy for BPH continues to generate interest because of two potential advantages: virtually no blood loss and the ability to perform laser surgery on an outpatient basis. Laser technology continues to evolve rapidly, and not every hospital or urologist has access to every laser technology. The patient should discuss with the urologist what laser is to be used in his treatment and why, as well as what are the individual urologist’s results.
What is microwave therapy of the prostate?
Microwave energy has been used to treat BPH using both transrectal and transurethral approaches, but most modern machines use the transurethral route. Current machines deliver microwave energy to the prostate via a transurethral catheter, and a transrectal balloon monitors rectal temperature simultaneously. The treatment is delivered under local anesthesia on an outpatient basis and typically takes about one-half hour. The patient will go home with an indwelling urethral catheter for a period of days at the discretion of the urologist.
JN: Is a patient who has undergone microwave therapy for the prostate, now with a urethral catheter left in for 7 to 10 days, able to go about his business without much trouble?
Should the catheter be removed by only a health care professional?
KL: Yes, the patient can generally go about his business without much trouble with a catheter in place. It is best to have the catheter removed by a health care professional.
What are the results of microwave therapy?
Results after microwave therapy can be grouped into two classes: subjective and objective. Subjective results use patient symptoms score sheets where the patients record their perception of their voiding characteristics. Objective results such as measurements of peak urinary flow rates and post void residual volumes are measured by the physician. Using these criteria, several studies have shown improvement in both subjective and objective measurement following microwave therapy. This technology, however, is still relatively new, and long-term data are lacking. No one yet knows whether these promising early results are durable.
Terms:
Electrovaporization – a procedure in which electric current is used to destroy prostate tissue.
Extravasation – a discharge or escape of fluid, normally found in a vessel or tube, into the surrounding tissue.
Resectionist – the physician (urologist) who uses the resectoscope.
Brachycardia – a slow heart rate, usually under 60 beats per minute. A normal heart rate is from 60 to 100 beats per minute.