Prostiva RF Therapy from a Physician’s Perspective
Transurethral needle ablation (TUNA)
Transurethral Needle Ablation of the Prostate (TUNA)

What is radiofrequency therapy of the prostate?
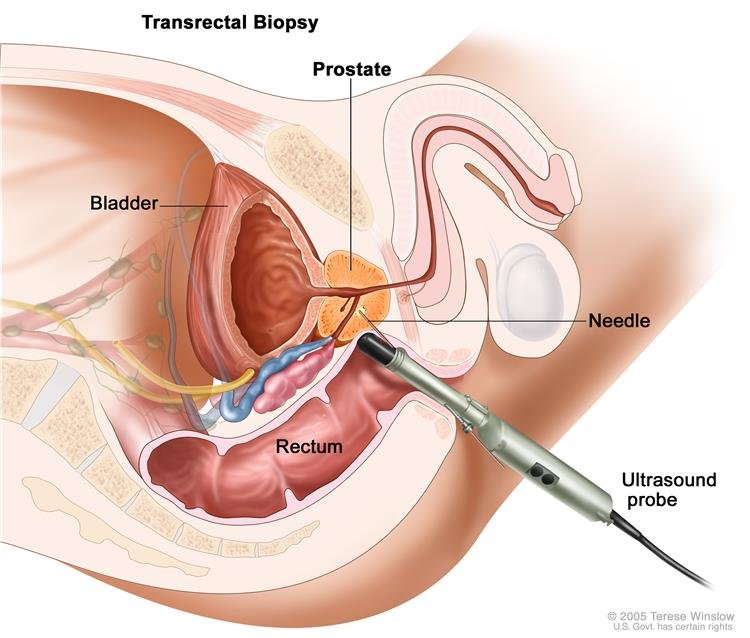
Radiofrequency treatment of BPH is commonly referred to as TUNA-transurethral needle ablation of the prostate. This technique involves placing interstitial radiofrequency needles through the urethra into the lateral prostatic lobes to cause coagulation necrosis The tissue is heated to 100ºC at a radiofrequency power of 490 KHz for 4 minutes per lesion. The number of times the needles are placed into the prostatic lobes is at the discretion of the urologist based on the size of the prostate gland.
Two needles that are at 60-degree angles to each other are deployed into the prostatic tissues by piercing the prostatic urethra. Each treatment with the needles treats prostate tissue about 1 cm in diameter.
What are the results of radiofrequency therapy?
TUNA of the prostate uses radiofrequency energy to treat the patient. As with most of the other MIST results, few long-term data are available, and thus, results must be viewed with caution.
What are prostatic stents?
Prostatic stents are devices that are placed transurethrally and expand to keep the prostatic urethra open. In many ways, they are similar to the coronary artery stents that have gained wide notoriety The patients who are candidates for prostatic stents are fairly limited in number. Although some absorbable stents have been developed, they are not yet available for routine use. The clinically available stents are metallic and nonabsorbable. After they are placed, they are very difficult to remove. Prostatic stents are most commonly used in older men who are in urinary retention requiring an indwelling urethral catheter and who are not candidates for any type of invasive therapy. After the stents have been in place for a few months, the mucosa or lining of the urethra grows through them, and they no longer can be seen cystoscopically.
What are the results of prostate stents?
As mentioned, in properly selected patients, prostatic stents can be very useful. The results of one specific type of prostatic stent called the UROLUME.
What is balloon dilation of the prostate?
In the late 1980s, balloon dilation of the prostate was introduced with great enthusiasm. The concept was similar to that of angioplasty of the coronary arteries, namely a balloon could dilate or stretch the prostatic urethra and thereby relieve obstruction. Several different types of balloons were developed and the early results were very encouraging.
Balloon dilation of the prostate was attractive because it could be done on an outpatient basis, although x-ray guidance of the balloon position and regional anesthesia were required.
What are the results of balloon dilation of the prostate?
Despite the encouraging early results, the improvement initially seen after balloon dilation of the prostate deteriorated over time. By about 2 years, several series showed that subjective and objective measurements had returned to baseline. Currently, balloon dilation of the prostate is no longer used and is considered obsolete.
What other minimally invasive surgical treatments of the prostate are available?
New ablative therapies of prostate tissue continue to be investigated. Among the most promising is alcohol injection of the prostate. This technology is still under development and is not clinically available except as a research protocol.
What is the role of a permanent indwelling urethral catheter in the treatment of BPH?
Some patients with prostatic obstruction and a weak bladder will not be able to void, regardless of what type of surgical intervention is employed. Some of these patients elect to be managed with an indwelling urethral catheter. The main drawback to an indwelling catheter is infection. In addition, sometimes the catheter can become plugged with blood or debris and needs to be changed emergently. Most patients with an indwelling urethral catheter have it changed by a visiting nurse at home or in the emergency room or their doctor’s office at 1- to 2-month intervals.
An alternative to an indwelling urethral catheter is a suprapubic tube. A suprapubic tube can be placed percutaneously (through the skin) into the bladder through the lower abdominal wall. Many patients find a suprapubic tube more comfortable and easier to manage than a urethral catheter. Either the suprapubic tube or urethral catheter is connected to a drainage bag, which can be worn on the leg or hung on the side of bed. A suprapubic tube is typically changed by a nurse or physician as is the urethral catheter every 1 to 2 months.
What is the role of a clean intermittent catheterization in the treatment of BPH?
The problem with indwelling catheters is infection, as well as the fact that some patients find them cumbersome. If a patient is dexterous and motivated, he or she can be easily taught how to catheterize themselves every 4 to 6 hours.
This is a clean, but not sterile, procedure. Namely, the catheter should be clean but can be reused if necessary. Teenagers have been taught to do clean intermittent self-catheterization. It is not hard to do. In circumstances in which a patient is unwilling or unable to perform self-catheterization, a family member can be taught how to perform the task.
What is the role of urecholine in the treatment of BPH?
It is not uncommon for older men to go into urinary retention after any type of surgery that requires an anesthetic. Often these men are given a drug called urecholine that has been shown in laboratory studies in animals to stimulate bladder contractions.
The doses that can be used in humans, however, are pharmacologically inadequate to cause significant bladder contractions. Therefore, urecholine has little clinical value and should not be used in patients with urinary retention.
Terms:
Prostatic stents – cylindrical devices that can be placed in the urethra to relieve prostatic obstruction.
Suprapubic tube – a type of catheter placed percutaneously (through the skin) into the bladder through the lower abdominal wall in order to drain urine