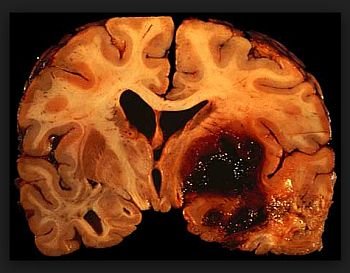
All of the following may present similarly to a stroke. In all cases, the distinction can be made by an emergent MRI scan, which will show abnormal diffusion-weighted signal in most stroke cases, but not in mimics.
. Seizures. If a seizure has a focal onset in the brain, the patient may be left with weakness, numbness, speech, or vision problems for a period of time (usually less than 24 hours) after the seizure. Unlike the typical cerebral infarct, focal deficits after a seizure are often accompanied by lethargy and have a resolving course, but if the patient has had a seizure accompanying a stroke it is impossible to know for sure how much of the deficit the patient displays is due to each. This is why patients with seizures at onset are usually excluded from clinical trials of new stroke therapies.
. Migraine. Patients may have unilateral weakness or numbness, visual changes, or speech disturbances associated with a migraine headache (‘‘complicated’’ or ‘‘complex’’ migraine). Also, patients with complicated migraine are at higher risk for stroke. In trying to make the distinction between complicated migraine and stroke, it is important to remember that because of the high prevalence of both migraine and stroke in the general population, it is dangerous to attribute the patient’s deficit to migraine just because the patient has a migraine history. The best rule of thumb is not to make the diagnosis of complicated migraine or migrainous stroke unless the patient has a history of previous complicated migraine events similar to the deficit displayed in the emergency department.
. Syncope. This is usually due to hypotension or a cardiac arrhythmia. Stroke rarely presents with syncope alone. Patients with vertebrobasilar insufficiency may have syncope, but there are usually other brainstem or cerebellar findings if syncope is part of the stroke presentation.
. Hypoglycemia. Patients with low blood sugar may have symptoms that exactly mimic a stroke. The important thing is to check the blood sugar and, if low, correct it. If the symptoms do not resolve with correction of the hypoglycemia, the symptoms are probably from a stroke.
. Metabolic encephalopathy. Patients may have confusion, slurred speech, or rarely aphasia with this condition. They usually do not have other prominent focal findings.
. Drug overdose. Similar to metabolic encephalopathy. Central nervous system tumor. The location of the tumor would determine the type of signs and symptoms seen. A tumor, unlike a stroke, usually does not present with sudden focal findings, unless accompanied by a seizure.
. Herpes simplex encephalitis (HSE). This infection tends predominantly to affect the temporal lobes, so patients may have signs of aphasia, hemiparesis or visual-field cuts. Onset can be rapid and in its early stages may mimic a stroke, but fever, CSF pleocytosis, seizures and decreased level of consciousness are more prominent with HSE.
. Subdural hematoma. Depending on the location, this may cause contralateral weakness or numbness that may mimic a stroke.
. Peripheral compression neuropathy. This may cause weakness or numbness in a particular peripheral nerve distribution and is usually not sudden in onset.
. Bell’s palsy (peripheral seventh nerve palsy). The important point here is that the forehead and eye closure are weak on the same side. One can have a stroke involving the pons and produce a peripheral seventh nerve palsy, but usually there are other signs and symptoms such as weakness, a gaze palsy, or ipsilateral sixth nerve palsy.
. Benign paroxysmal positional vertigo (BPPV). This may cause vertigo, nausea, vomiting, and a sense of imbalance, usually with turning of the head in one direction. This characteristic syndrome is due to labyrinthine dysfunction and not stroke. However, as with syncope, the presence of any brainstem or cerebellar signs should alert one to the possibility of a stroke.
. Conversion disorder. Patients may develop neurological signs or symptoms of weakness, numbness, or trouble talking that are manifestations of stress or a psychiatric illness. Always assume that your patient has a true neurologic illness first.