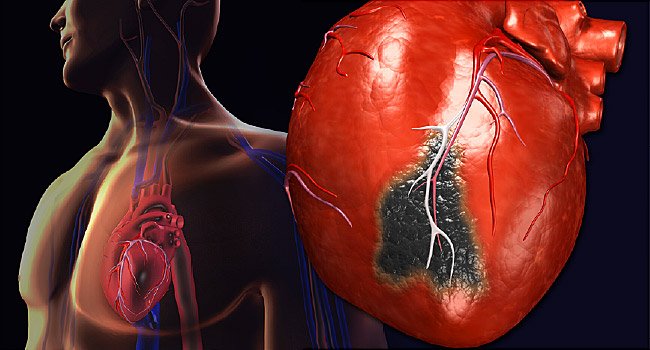
What are the characteristic features of chest pain or other forms of chest discomfort felt by heart attack victims?
For one thing, you would feel any form of chest pain or chest discomfort deeply rather than feeling it on the surface. Physical exercise, stress, or anger often trigger chest pain, but heart attack pain does not clear up by resting or taking even three or more tablets of nitroglycerin.
Heart attack victims often describe such chest pain as crushing, heavy, oppressive, or constricting, or as a sensation of severe pressure in the chest. Chest pain frequently occurs behind the breastbone. As has been pointed out, it may spread to the left arm, left shoulder, jaw, teeth, or neck or to the center portion of the upper back. Occasionally, it may radiate to the right arm or right shoulder as numbness or a tingling sensation instead of as outright pain. Sometimes, such discomfort may be felt in much lower locations than usual, so it may be pronounced in the upper abdomen. In 10 to 15% of heart attack victims, a typical silent heart attack might not produce any pain at all.
Do women’s and men’s heart attack symptoms differ?
Women often experience nausea and vomiting. Pain or severe discomfort is frequently felt in the upper abdomen. Sometimes women notice only marked fatigue after everyday physical activity, rather than chest pain. Women’s symptoms of angina or heart attack are not typical, so they often delay medical attention and necessary diagnostic tests.
Many women misinterpret their heart attack symptoms as other illnesses, and they have a tendency to regard their symptoms very lightly. For this reason, many physicians tend to manage this disorder less aggressively in women patients.
Which heart attack victims are at highest risk of death?
The outcome of a heart attack depends on the conditions that surround the event. Outcome is more serious in some people than in others. For example, elderly people (particularly those with poor general health conditions) react more intensely to heart attack. People with diabetes and diseases of other organs (e.g., kidneys, liver, and lungs) also are less able to endure a heart attack. This holds true also for people recovering from cardiac arrest; those having had a massive heart attack or blockage of multiple heart arteries; and those with multiple coronary risk factors. People having varied complications (e.g., congestive heart failure, serious heart rhythm abnormalities) also suffer the results of heart attack much more severely.
What is a silent heart attack and whom will it strike?
The term silent heart attack describes an attack that produces little or no chest pain. In place of chest pain, silent heart attack makes itself known by rather uncommon symptoms: marked dyspnea (shortness of breath), extreme fatigue, and life-threatening cardiac arrhythmias (abnormal heart rhythms). A silent heart attack may occur in 10 to 15% of heart attack cases (up to 25–30% according to some medical reports). It’s relatively common among elderly people and diabetic patients. It’s also more common in undereducated people and in chronic alcoholics. Such heart attacks are commonly misdiagnosed or their diagnosis is delayed because of their unusual symptoms.
Thus, risk of death in a silent heart attack is higher.
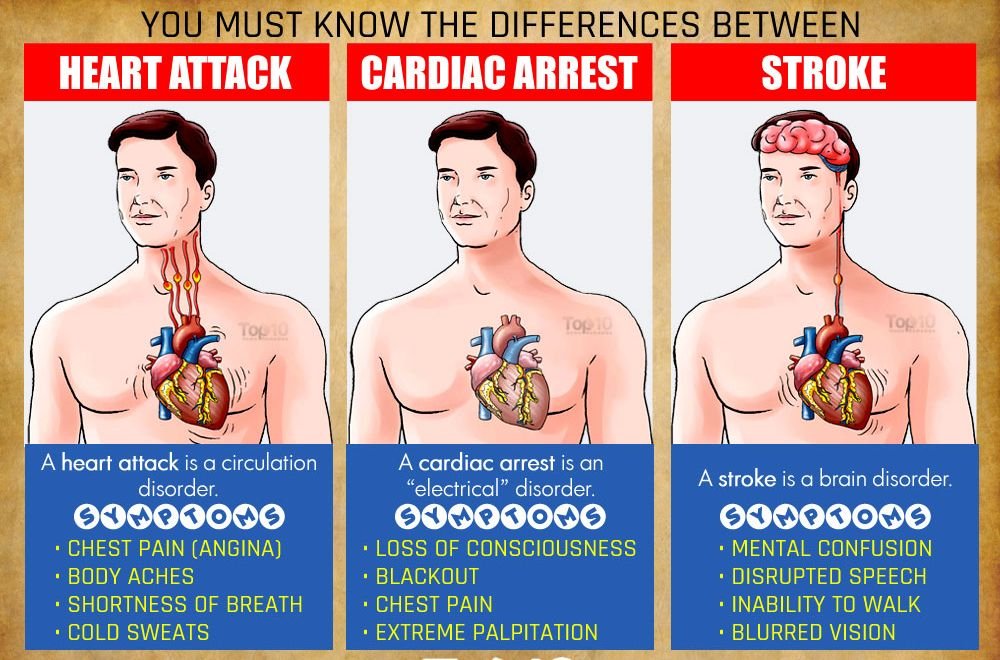
What is cardiac arrest?
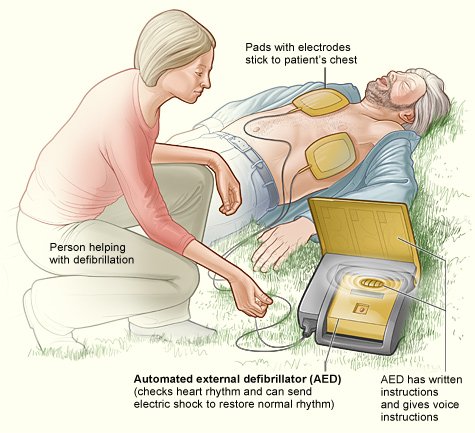
Cardiac arrest means that the heart is not able to pump the blood at all as a result of ineffective, abnormal heart rhythms: too fast, too slow, or lack of heartbeat. When cardiac arrest strikes, your lungs also fail to function, leading to cardiopulmonary arrest. (Cardio means heart, and pulmonary means lungs). Because blood circulation to the entire body, including the brain, is stopped, you become unconscious (enter a coma or a semicomatose state).
By and large, the underlying cause of cardiac arrest in the majority of the cases is ventricular fibrillation (as mentioned, a very rapid, irregular, chaotic, and ineffective heart rhythm arising from the ventricles). On the other hand, an AV block (heart block, slower or nonexistent conduction of the cardiac impulse from the atria to the ventricles) usually causes a very slow heart rhythm. This is a condition in which the electrical conduction of heart impulses to the ventricles is slowed or interrupted.
Terms:
Cardiopulmonary arrest – cessation of heart and lung functions.
Heart block – slower-than-usual or absent conduction of the cardiac impulse from the atria to the ventricles.
What are the direct causes of sudden cardiac death?
In the majority of the cases, sudden cardiac death occurs as a result of ventricular fibrillation, the chaotic heart rhythm arising from the ventricles. You can use the terms sudden cardiac death and cardiac arrest interchangeably, but the underlying problem is ventricular fibrillation.
CONDITIONS THAT MIMIC HEART ATTACKS
Can other ailments cause me to think I’m having a heart attack?
Many disorders, both cardiac and noncardiac, may closely mimic a heart attack. For example, the symptoms of cardiac diseases or disorders, such as myocarditis (inflammation of the heart muscle), pericarditis (inflammation of the sac surrounding the heart), and aortic dissection or rupture (tear of the main artery leading from the heart), can cause you to think you’re going through a heart attack. Certain disorders or diseases of the lungs can also fool you. Some of them include pulmonary embolism (blood clots in the lung arteries), a pneumothorax (a collapsed lung), and pneumonia (infection and inflammation of the lungs). Then, too, you could be experiencing severe asthma, pulmonary hypertension (elevated BP in the arteries carrying blood to the lungs), or pleurisy (inflammation of the membrane that lines the chest cavity and covers the lungs).
Gastrointestinal diseases and disorders that might fool you would be gallstone, cholecystitis (inflammation of the gallbladder), peptic ulcer, heartburn, and disorders of your esophagus. As if that isn’t confusing enough, you could be having a panic attack (an anxiety attack) or Tietze’s syndrome. Possibly you might have fractured a rib or be having pain in bones in that area due to other causes, such as sore muscles in the chest.
Other disorders with similar symptoms that might not be very familiar to you are shingles, cancer, anemia, and vasculitis (a group of disorders that inflame the blood vessels). Even exposure to high altitudes could produce discomfort resembling that of a heart attack.
Because there are so many potential reasons for your symptoms-including the possibilities that you really are having a heart attack-you should not attempt to decide the cause for yourself. Even when it’s not a heart attack, some of the other possible causes are dangerous or life-threatening conditions, so you should get treatment regardless.
Terms:
Myocarditis – inflammation of the heart muscle.
Pericarditis – infection or inflammation of the pericardium.
Aortic dissection – a tear of main artery leading from the left ventricle.
Pulmonary – embolism blood clots in the lung arteries.
Pneumothorax – collapse of part or all of a lung as a result of accumulation of air in the chest cavity.
Asthma – recurrent sudden shortness of breath, with wheezing cough and sensation of constriction.
Pulmonary hypertension – elevated blood pressure in the arteries carrying blood to the lungs. Pleurisy inflammation of the membrane that lines the chest cavity and covers the lungs.
Cholecystitis – inflammation of the gallbladder causing abdominal pain.
Esophagus – feeding tube connecting the mouth and stomach.
Shingles – disorder caused by the herpes zoster virus (chicken pox) that can cause intense pain along the nerve distribution.
Anemia – a decrease in the red blood cells and/or hemoglobin content of the blood.
Vasculitis – group of disorders that cause inflammation of the blood vessels.