(Doctor only)
Symptom fluctuations without a good cause
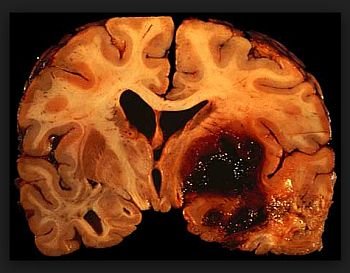
Some patients deteriorate without an obvious explanation. This is a poorly understood phenomenon. It is commonly seen with sub cortical strokes. While this usually occurs in the first three days, it can occur up to two weeks after stroke onset.
The mechanism is unknown. Local hypoperfusion? Inflammation? Neurochemical or neurotransmitter changes? Apoptosis?
Treatment is mainly supportive (maintain euvolemia, check blood pressure to make sure it doesn’t drop, put head of bed flat). Anti-inflammatory (i.e., high-dose statins) and other neuroprotective therapies are under evaluation. One recent study of a free radical trapping drug showed improved outcome in acute ischemic stroke patients, indirectly supporting the laboratory evidence demonstrating an important role of inflammation in producing damage after stroke.
The uncooperative patient
Patients can become confused after a stroke. Contributing factors include advanced age and underlying dementia, placement in a disorienting critical-care environment, and sleep deprivation.
Often, movement to a quiet private room helps, but this has to be balanced against less close scrutiny and treatment of medical complications outside the stroke unit or ICU setting. While sedation should be avoided, low doses of antipsychotic agents can be useful and are used commonly – such as haloperidol PO or IV 0.5–2.0 mg, risperidone 1mg PO and quetiapine 25mg
There are also data to suggest that newer antipsychotic agents increase mortality of patients with dementia, though this was with prolonged treatment (10–12 weeks). Therefore pharmacologic management of agitation and confusion should be practiced with caution. Good nursing care, orientation, and calm environment are important.