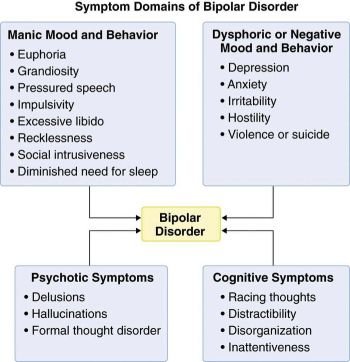
Bipolar Disorder. Sex, Hyper sexuality, High Libido. Mental Health Professionals
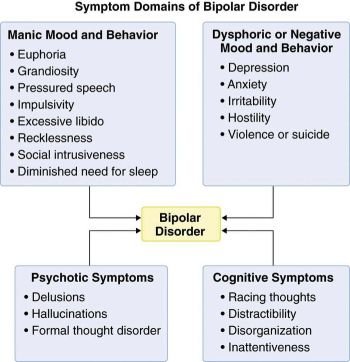
How is psychotherapy helpful if bipolar disorder is due to a chemical imbalance?
Every thought, feeling, and behavior is associated with a chemical change in the brain. If thoughts, feelings, and behaviors occur with a repeated pattern, structural changes can occur in the brain as well. Learning and memory involve complex chemical changes that lead to permanent structural changes in brain anatomy. For example, consider the first time that you learned how to drive a car. It required conscious processing of complex pieces of information and integrating the information into an organized behavioral pattern. The powers of concentration at that time can be exhausting.
However, with practice the skill becomes second nature as the brain adapts the skill so that much of it occurs unconsciously. Behavior ultimately leads to structural and biochemical changes in the brain.
The chemistry and structure of the brain can change via one of three methods:
1. Change in the environment
2. Change in brain chemistry via chemical modification with the use of psychotropic medication
3. Learning how to modify the environment or perception of the environment by developing new skills.
Moving, changing jobs, and getting married or divorced are examples of the first method, while psychopharmacology is the second.
Psychotherapy is the third method.
Brain imaging studies have repeatedly demonstrated, for example, that changes occur in the same brain regions of patients with obsessive-compulsive disorder on Sarafem (fluoxetine) as those receiving cognitive-behavioral therapy.
Each of these methods has their own inherent costs and benefits and therefore none can be considered inherently better or worse than another. The effects of all three methods are generally cumulative; thus in order for one to have the best chance of recovery from mental illness, a combination of two to three methods is generally warranted. In bipolar depression, therapy can be especially useful in an attempt to treat the depression without an antidepressant or with as low a dose of an antidepressant as possible. Therapy can help patients maintain daily structure and rhythm to help prevent the recurrence of mania. During a manic episode, therapy provides support and psycho education that are critical for treatment adherence and recovery.
What are the different types of medication used to treat bipolar disorder?
How does my doctor choose a medicine?
The treatment of bipolar disorder is fraught with controversy. The two most controversial issues include the definition of a “mood stabilizer” and the use of antidepressant medications for the bipolar depressed patient.
A true mood stabilizer should ideally treat acute mania, acute depression, and prevent both relapse and recurrence of either mania or depression. By that definition there is really no true mood stabilizer outside of electroconvulsive therapy (ECT), which is successful in treating all categories of bipolar illness. Typically, therefore, most clinicians equate the term mood stabilizer with a medication that treats acute mania and prevents its recurrence. More appropriately, these should be termed antimanic agents, as they are parallel to antidepressant agents and treat the other end of the mood spectrum. All mood stabilizers fail in the treatment of acute depression.
The jury is out as to whether they prevent depression in the same way they prevent mania. For this reason antidepressants are still commonly used. But because antidepressant medications may switch an individual from depression into mania and actually worsen one’s overall condition, the issue of antidepressant use remains controversial. Complicating this issue is the fact that some clinicians define a mood stabilizer as any agent that treats one arm of the bipolar spectrum without causing switching to the other arm. By this definition, some antidepressants may meet this standard, though the jury is out in this regard as well. It does appear that some classes of antidepressants cause less switching than others.
These classes include the SSRIs and buproprion. Also by this definition the anticonvulsant Lamictal (lamotrigine) has been called a mood stabilizer even though it is clearly more effective in preventing a depressive relapse or recurrence than a manic relapse or recurrence.
Thus, the term mood stabilizer is generally used very loosely to describe any medication that treats “mood swings,” an equally vague term that can mean just about any type of emotional change, even those associated with personality disorders such as borderline personality. One final caveat: most antimanic agents stabilize neuronal cell membranes. As a result, any type of over stimulation of the central nervous system, whether it is seizure activity, mania, a panic attack, or explosive rage, can respond to an antimanic agent. Therefore, the fact that one’s mood is “stabilized” by an antimanic agent does not necessarily mean one is bipolar.
With that introduction let us now proceed with the different classes of medications that are used in the treatment of bipolar disorder. The classes more specifically break down into several of the following categories in order of understanding and importance in treating the condition:
• Lithium carbonate and its different formulations
• Anticonvulsant medications• Atypical antipsychotic medications
• Typical antipsychotic medications
• Benzodiazepines
• Antidepressant medications (specifically the selective serotonin reuptake inhibitors, or SSRIs)
• Calcium channel blockers
• Mood stabilizers
• Others under investigation
Note that the antimanic effects of anticonvulsants do not exhibit a class effect. That is, just because a medication is considered an anticonvulsant one cannot immediately assume it has antimanic properties. This was prominently demonstrated after the medication Neurontin (gabapentin) was touted for its potential antimanic effects prior to any clinical trials, which later demonstrated that it was not superior to placebo and led to a series of lawsuits against the manufacturer for false promotion. Alternatively, both the typical and atypical antipsychotic all demonstrate antimanic effectiveness and therefore clearly exhibit a class effect.
The specific medications, whether or not FDA approved, whether or not clinical trials exist to demonstrate their effectiveness, and whether or not they are routinely used clinically regardless of either FDA approval or the existence of clinical trials supporting their use. Bear in mind that this table does not represent all the medications used to treat bipolar disorder but rather the most common. The majority of medications used in the treatment for bipolar are used off-label as they are not FDA approved. First, the FDA is slow to approve medications. Second, pharmaceutical companies are slow to perform clinical trials. Trials are expensive, and once a drug is approved for acute mania, the need to seek approval for the other aspects of the condition diminishes considerably unless increase in market share can be anticipated with FDA approval. Third, once a drug becomes generic, only the government will spend money on a clinical trial.
Finally, just because there are negative clinical trials does not mean that a medication is no longer used. There is enough individual variability in bipolar disorder to not immediately discount any medication, particularly when one is refractory to those medications that have proven beneficial. This is one reason why Neurontin (gabapentin) continues to be used, although in a very limited, circumscribed manner today than prior to the uproar around it. There are individuals who may idiosyncratically respond to one medication just as there are individuals who have idiosyncratic paradoxical responses to another, neither of which condition can be predicted.
There are published treatment guidelines and algorithms that psychiatrists follow in order to simplify this table and start with the most appropriate medication depending upon the clinical presentation. There also appear to be many differences between bipolar I and bipolar II disorder.
All clinical trials leading to FDA approval are based on bipolar I disorder, and it is not clear if these medications have the same effect on bipolar II disorder. It is also not clear if bipolar II disorder is truly a “spectrum” disorder-that is, lying on a continuum with bipolar I disorder rather than a unique entity itself.
This uncertainty is partly based on genetic studies that suggest that bipolar I disorder shares more genes in common with schizophrenia and schizoaffective disorder than with bipolar II disorder. It is also partly based on at least some clinical reports that bipolar II patients may respond differently to the listed medications than bipolar I patients.
That being said, the general guideline makes the following recommendations. If a patient presents with acute mania, use of one medication is indicated; the choice between lithium and Depakote (valproate) is based partly on each medication’s side-effect profiles as well as the presence or absence of various symptoms.
For example, for patients who have suffered from depression but are currently manic, lithium is recommended. Lithium appears to be the closest to meeting the definition of a mood stabilizer in that it appears to prevent both depression and mania. For those patients who have recurrent manic episodes without depression, anxiety/agitation, or a substance abuse disorder, valproate is recommended. Patients with rapid cycling symptoms (four or more episodes annually) may respond better to either Equetro (carbamazepine) (if the episodes include more depression) or Depakote (valproate) (if the episodes include more mania). For manic patients with psychotic features (delusions, hallucinations, and/or grossly disorganized thinking and behavior) the addition of an atypical antipsychotic medication is recommended, but most atypical antipsychotics have FDA approval for monotherapy treatment of an acute manic episode.
Alternatives to lithium and Depakote (valproate) include Equetro (carbamazepine) and Trileptal (oxcarbamazepine).
If symptoms are not adequately controlled within 10 to 14 days, addition of a second first-line agent is indicated (e.g., adding an anti-psychotic if not already prescribed). Clozaril (clozapine) may be effective in refractory cases.
For bipolar depression, either Lamictal (lamotrigine) alone (or with an antimanic agent) or Symbyax should be initiated. If one fails to respond to these two strategies the addition of Seroquel (quetiapine) or lithium may be recommended. Failing that, an additional antimanic agent plus an SSRI, buproprion, or Effexor (venlafaxine) may be added. Electroconvulsive therapy (ECT) is considered for more refractory cases (as well as for refractory mania).
Trials of nontraditional medications such as calcium channel blockers, stimulants, or thyroid hormone should be considered in conjunction with all of the above when symptoms cannot be adequately controlled.
This is known as rational polypharmacy, as medications from different classes with different actions are added that may have a synergistic effect to improve mood stability.
Leslie’s comments:
This is difficult because each prescriber has a different theory on what makes the best combination of medication. I have been on so many different medications trying to get it“right.” It can become very disheartening to try a medication, take the time to build up to a therapeutic dose, and then realize that either it’s not working or the side effects cannot be tolerated. Sometimes I have felt like a guinea pig trying these medications but, in the end, it does pay off because when you find the right medications, the disorder is manageable. Right now I am on an antidepressant, a mood stabilizer, and an atypical antipsychotic. This seems to be a good combination for me.
Terms:
ECT – electroconvulsive or shock therapy
Benzodiazepine – a drug that is part of a class of medication with sedative and anxiolytic effects. Drugs in this class share a common chemical structure and mechanism of action.
Placebo – an inert substance that when ingested causes absolutely no physiological process to occur but may have psychological effects.
Off-label – prescribing of a medication for indications other than those outlined by the Food and Drug Administration (FDA)
Rational polypharmacy – the practice of combination medication therapy with consideration of the clinical effects, adverse effects, drug interactions, and relation between effective and toxic drug levels, as well as with an understanding of the mechanisms of action of each agent.