Developing Diabetes In Pregnancy Increases Risk For Autism In Babies Up To 63%
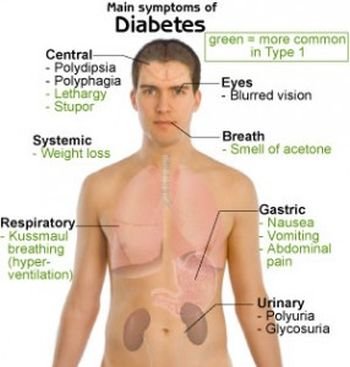
Diabetes in the young
Diabetes in young people is divided naturally into three main age groups: babies, children and adolescents. Diabetes on babies and children consist of questions asked by parents and the answers are naturally directed at them. Diabetes on adolescents is for both young people and their parents. We have listened to hundreds of parents who have felt the despair of finding that their child has diabetes and then overcome their fears to allow their child to develop to the full. Mothers and fathers usually end up by being especially proud of children who have diabetes. We hope to pass on some of this experience to those parents who are still at the frightened stage.
The baby with diabetes
My baby developed diabetes when she was 4 weeks old. She is now 6 weeks old and looks very healthy but I would like emergency advice in order to protect her life. What food and treatment should I give her?
You must be relieved that your baby is better now that she has started treatment, but worried about the difficulties of bringing up a child with diabetes from infancy. Diabetes is very rare in infants less than 12 months old, so you will not find many doctors with experience of this condition. However, the general principles are the same for all infants with diabetes and there is no reason why she should not grow into a healthy young woman.
Diabetes UK has produced a special youth pack for children under 5 years old, which contains many useful documents including a booklet about babies with diabetes. Diabetes UK might also be able to put you in touch with other people who have had the same problem. Practical advice and reassurance from these people would be more use than any theoretical advice.
Like all babies, your daughter will be fed on breast or bottle milk. For the first 4 months frequent feeds are best – 3-hourly by day and 4-hourly by night. Bottle-fed babies usually need 1 scoop (168 g of milk per kg of body weight) each day (21⁄2 ounces per pound). Some babies grow very rapidly and need more milk than this, while others may need solids earlier than 4 months. This may be a help in babies with diabetes as the solids will slow down the absorption of milk. It is important to wake young babies for a night feed to avoid night-time insulin reactions.
If there is any doubt about this, do a blood glucose check while your baby is asleep. If her blood glucose is low an additional 5–10 g carbohydrate (100–200 ml milk) should be given.
My little boy is nearly 12 months old and has been ill for a month, losing weight and always crying. Diabetes has just been diagnosed. Does this mean injections for life?
Yes. We are afraid it does literally mean injections for life. The thought of having to stick needles into a young child quite naturally horrifies parents, but with loving care, explanations and playing games like injecting yourself (without insulin) and a teddy bear (using a different needle) and perhaps some bribery, most children accept injections as part of their normal day. Young children grow up knowing no other way of life and they often accept this treatment better than their parents do. Encourage your child to help at injection time by getting the equipment ready or perhaps by pushing in the plunger and pulling out the needle.
How can I collect urine for testing from my 18-month-old son?
It is not easy to get clean samples of urine from babies in nappies. Many infants will produce a specimen by reflex into a small potty when undressed. You can also squeeze a wet nappy directly onto a urine testing stick. But be warned – washing powders or fabric softeners in the nappies alter the urine test result.
Diastix or Diabur-Test 5000 can be used for testing for glucose, whilst Ketostix or Ketur Test are used to test for ketones. Keto-Diastix and Keto-Diabur tests for glucose and ketones. Infants are much more likely than older people to have ketones in the urine. This is because they rapidly switch to burning up fat stores in the fasting state. It is important to check on ketones and try to keep his urine ketone-free, although you should not worry if ketones appear for a short time.
You will also have to do blood tests on your son. Parents expect children to find these painful but blood tests taken from a finger, heel or ear lobe are surprisingly well accepted by young people. They enable you to check accurately what is happening if your son feels unwell or looks ill. Urine tests provide only a guide about the state of his diabetes since his last urine specimen. The blood test confirms what is happening at that very instant. It is the only reliable way of deciding whether your son is hypo or just tired and hungry. Blood glucose measurements are also necessary to check the overall control of his diabetes and to help you decide on the dose of insulin if his blood glucose rises during an illness. Blood samples should be obtained with an automatic finger pricker – the Autolet (Owen Mumford [Medical Shop]) has a special platform for children, but the Soft Touch and Softclix (Roche), the Glucolet (Bayer Diagnostics), the BD Lancer (BD) and the Monojector (Tyco Healthcare) are all suitable. There are new blood glucose meters on the market that need only a very small amount of blood for the test. For instance, the OneTouch Ultra works on a tiny blood sample and comes with a new lancing device, which is adjustable. The small blood volume means that only the shallowest skin puncture is needed. Adults can check their glucose by sampling from their arm and it is virtually painless. Such a meter would be ideal for a baby or young child.
My 2-year-old daughter has diabetes and makes an awful fuss about food. Meals are turning into a regular struggle. Have you any suggestions?
Food is of great emotional significance to all children. If meals are eaten without complaint, then both mother and child will be satisfied. All children go through phases of food refusal because of a need to show their growing independence, their ability to provoke worry or anger in parents and their attempts to manipulate the situation. Food leads to the well-known battleground, which occurs in all families at some stage. The only way for you to win is to remain in control of the weapon. Usually when young children begin this phase (at 10-18 months), they dislike being told to leave the table and go away. They often return and eat rather than remain alone and hungry.
The battle is even more difficult for parents like you where the child has diabetes – your daughter has some explosive weapons!
However, you must stay in control: try distracting her attention away from food by toys, music, talk or your own relaxed approach to eating. You may have to send your daughter away from the table if she is refusing to eat properly. Hypoglycaemia often provokes hunger and, anyway, a couple of mild hypos due to food refusal are a small price to pay for better behaviour next time. Be prepared to modify the type of carbohydrate within reason if she consistently refuses the diet recommended by the hospital. Bread, potatoes, biscuits, fruit juices and even ice cream can be offered as alternatives.
Susie Orbach has written an excellent book called On eating. The box reprints the advice that was given in The Guardian (reproduced with permission from AP Watt Ltd on behalf of Susie Orbach).
FOOD AND YOUR CHILDREN
Dos and don’ts for babies and toddlers
• Do introduce your baby and toddler to the mashed-up version of the foods and tastes you relish, including the herbs and spices.
• Do clip a baby seat on to the table if possible so that the baby can be part of family eating and have her interest in what you are eating stimulated.
• Do respect your baby or toddler when they say ‘no’. When they turn away from eating, offer them some other food and if it doesn’t hit the spot, allow them to stop eating. They will soon let you know if they are hungry again.
• Do let your baby and toddler muck about with food and make a mess. Food is a source of creativity as well as fuel.
• Don’t encourage them to eat five more spoonfuls for grandma, or the starving children elsewhere, or play games that trick them into eating. Show them your relish in food. Dos and don’ts for primary-age children
• Do put lots of different kinds of food out and let the children choose what they fancy.
• Don’t differentiate between kids’ and adult food. Children’s tastes will be as complex and sophisticated as the foods they are exposed to.
• Do value foods equally so that broccoli becomes no less of a special food than ice cream.
• Do let children see you stopping when you are full and leaving food on your plate.
• Do let children leave food when they’ve had enough or when they are compelled to rush off to do something more interesting than eat. If you are worried they have not had enough to eat, make sure there is food around for them to come back and refuel on.
• Don’t ever reward them for eating their greens by offering those sweets or ice cream or cake. Do let them eat in whatever order they like including having dessert first if they are desperate for the carbohydrates.
• Don’t cheer them up or jolly them out of a sad or angry mood with food unless you know they are hungry. Do let them tell you how they feel without shushing them or humouring them out of their upset. If they tell you and get their feelings out in the open, the pain will dissipate faster.
Dos and don’ts for adolescents
• Do expect them to eat fast food. It’s a sign of independence, of showing how different they are from you, of making it with their peers. If you’ve fed them interesting food all along, don’t despair, they won’t be able to eat KFC or Wagamama every day.
• Do sit together around the table several nights a week. If they’ve stocked up on food after school and aren’t hungry, let them sit with you while you eat so that they get accustomed to being around food and only eating it when they are hungry.
• Don’t have fights while eating together. It fuses food and conflict together.
• Do have tons of food in the house and expect erratic eating. Teenagers have fast metabolisms and many need to eat lots more than adults.
• Do tolerate their cooking even if their experiments violate your basic principles in the kitchen.
• Do discourage them from dieting. Set the example by never doing it yourself.
• Don’t have a corner for ‘junk’ food. Disperse it among the foods you consider good.