VIDEO
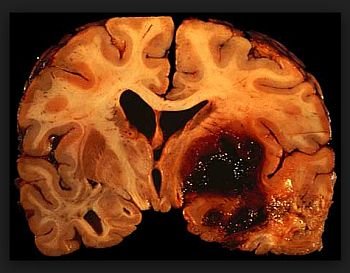
Carotid Stenosis: What it Means

Carotid Stenosis
(Doctors only)
Carotid stenosis is also one of the better-studied causes of stroke for which specific therapy is available.
There is a large body of literature on carotid endarterectomy and a large one is developing for carotid stenting. For review we recommend Barnett et al., 2002.
SYMPTOMAT I C INTERNAL CAROTID STENOSIS (70–99% BY NASCET CRITERIA OF ANGIOGRAPHIC STENOSIS)
Surgery (carotid endarterectomy, CEA) is beneficial compared to medical therapy.
– 2-year risk of ipsilateral stroke was 8.6% in the surgical group and 24.5% in the medical group (RRR 65%, ARR 16%, NNT 6 to prevent 1 stroke in 2 years).
– It is most beneficial to those who have highest risk of subsequent stroke: those who had hemispheric symptoms (compared to ocular symptoms), tandem extracranial and intracranial disease, and those without apparent collaterals.
– Perioperative risk was 5.8% overall and was higher for those with contralateral internal carotid occlusion and those with intraluminal thrombus, but those high-risk patients still received benefit.
SYMPTOMATIC ST ENOSIS (50–69%)
Benefit of surgery is marginal.
-5-year risk of any ipsilateral stroke was 15.7% surgical vs. 22.2% medical (ARR 7%, p¼0.045).
– No benefit in preventing disabling strokes.
– Women and those whose symptoms were limited to transient monocular blindness did not benefit.
– 6.7% 1-month surgical morbidity and mortality in NASCET.
ASYMPTOMATI C S TENOSI S
– The risks vs. benefits of treating asymptomatic carotid stenosis must be weighed very carefully.
– Two large randomized trials have shown that carotid endarterectomy for stenosis >60 -70% reduces ipsilateral ischemic stroke compared to medical therapy.
– ACAS showed that the 5-year risk was 5.1% for surgical vs. 11.0% for medical therapy.
– The results were confirmed by the ACST trial, which showed 5-year stroke risk of 6.4% for surgical vs. 11.8% for medical therapy.
– The overall subsequent risk is smaller than that for symptomatic carotid stenosis. The absolute risk reduction is about 1% per year, with NNT 17–19 to prevent 1 ipsilateral ischemic stroke in 5 years.
– The perioperative risk was 2.3% in ACAS and 3.1% in ACST.
– If one considers surgical treatment for asymptomatic carotid stenosis, the surgeon must have volume and experience.
– Women, for reasons which are unclear, have smaller benefit from carotid endarterectomy than men.
SURGERY: CAROTID ST ENTI NG V S .ENDARTERECTOMY
– Carotid stenting, though performed for several years now, is still considered investigational.
– SAPPHIRE was a randomized trial designed to compare carotid stenting (with a distal protection device) to endarterectomy in high-risk patients with symptomatic and asymptomatic carotid stenosis.
– It showed that the stroke rates at two years are equivalent (stenting is not inferior) and there was a trend favoring stenting in rate of adverse events.
– Several ongoing studies, including CREST, SPACE, EVA-3 S, and CAVATAS-2, are examining the effectiveness of the procedure in stroke prevention. So far, safety appears similar to that of CEA except in patients >80 years old.
– Some unresolved issues are durability of the stent and restenosis rates. The eventual hope is that carotid stenting will be cheaper and safer, especially in those with multiple medical comorbidities.
– Carotid stenting is approved for TIA and stroke patients where the stenosis is hard to reach surgically, where there are medical comorbidities that increase the risk of surgery, or in cases of post-radiation or postoperative stenoses. Outside of theses situations, stenting should be done only in the context of the aforementioned clinical trials.
WHEN CAN YOU
– CEA performed early after a symptomatic event confers the greatest benefit since the highest risk of recurrent stroke is in the first two weeks after a TIA or minor stroke.
– Combined data of NASCET and ECST trials show that the benefit of CEA is greatest with CEA performed within two weeks of symptoms.62,63 These trials, as well as a systematic review, saw no increased risk of early surgery (defined as earlier than 2–6 weeks). However, ‘‘unstable symptoms’’ or ‘‘urgent’’ surgery are also among the strongest risk factors for perioperative complications.
– Traditionally, it has been recommended to wait 4–6 weeks after a large stroke to perform revascularization by CEA.
The rationale is that reperfusing an area of recent stroke might lead to hyperperfusion or even hemorrhage. Breakdown of the blood–brain barrier and loss of autoregulation in the area of injury may lead to edema and bleeding.
Also, at the time of stroke, it may be unclear how well the patient will recover and how aggressive to be with various prevention strategies.
– In summary, it is probably best to revascularize early (within two weeks), especially after a TIA or if the stroke is small clinically and radiographically. There have been several studies in this regard, but none conclusive. A sense of ‘‘urgency’’ should be tempered with awareness of complications.