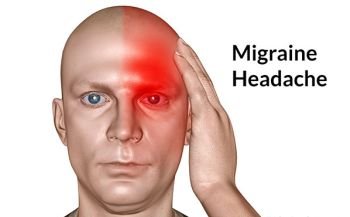
Managing Headache During Pregnancy
Migraine Action UK – The national advisory and support charity for people affected by migraine

PREGNANCY
I’m expecting our first baby. Am I more or less likely to get migraine while I am pregnant?
If you get menstrual migraine, there is a 60-70% chance that you will have few or no migraines while pregnant. This is even more likely if you normally get migraine without aura. Up to 25% of women get no change in migraine frequency while they are pregnant but, unfortunately, 4-8% finds that their attacks get worse. They are more likely to get worse if you normally get migraine with aura.
My sister did not get any migraines while she was pregnant but I do. Why are we different?
It would be fair to say that no one really knows why but it is assumed that it is something to do with the steady level of oestrogen that occurs during pregnancy. Pregnancy is divided into three ‘trimesters’ and migraine might get worse in the first trimester and then improve in the second and third trimesters.
Your situation is more likely to improve if you have migraine without aura. You are more likely to get migraine with aura for the first time during pregnancy and it is more likely to get worse during pregnancy.
I have always had migraines around the time of my period. Will they get better or worse while I am pregnant?
Migraine around the time of your period, especially if it is true menstrual migraine, is normally migraine without aura. The expectation would be that the migraine will get better, especially in the second and third trimesters.
Are there any headaches that occur during pregnancy that I should be worried about?
A serious (or ‘sinister’) headache can occur at any time, not just during pregnancy. The main concern in pregnancy is a headache that is associated with pre-eclampsia or eclampsia. Pre-eclampsia is a condition that can occur at any stage in pregnancy and is associated with a rise in blood pressure, swelling of your feet and/or fingers and protein in your urine.
Eclampsia is the next step and much more serious. The headache will often become much more severe, the blood pressure higher and may be associated with changes in the level of consciousness and, occasionally, fits. If you are worried about your headaches, talk to your doctor or midwife about them.
I am six months pregnant and occasionally get blurred vision with a bad headache. Should I go and see my doctor or midwife?
Any change in your vision should not really be ignored. It could be related to your blood pressure or possibly a rise in the pressure in your eye. The latter, called glaucoma, can be associated with eye pain or headache.
Blurring of your vision is not usually a feature of migraine aura unless it is what is referred to as stereotypical – meaning that the pattern is consistent and blurring is more of a visual distortion rather than just a slight loss of focus.
If you get new symptoms or a change in symptoms, it is always important to seek advice. If you don’t want to bother your doctor in the first instance, you could see your optometrist and, if this assessment seems normal, see your doctor or midwife.
I am a little concerned as I got these horrible flashing lights in the middle of my vision when I was pregnant. I never got a headache to follow. What was this all about?
Migraine with aura can occur for the first time in pregnancy, although it is not clear why. The flashing lights might have been a migraine aura. As is the case when you are not pregnant, it is possible to get an aura but not have a headache follow it.
My mother got her first migraine when she was pregnant with me. My sister and aunt get migraine, but I have never had one. I have just got pregnant and wonder what my chances of getting a migraine while pregnant are?
The optimistic view would be low, the pessimistic view would be high and the realistic view is ‘who knows’. If you have a family history of migraine, you have an above average chance of developing migraine at some time. Migraine can develop at any time and pregnancy is as good a time as any.
I have never had migraine before but I developed migraine with aura during the early part of my pregnancy. Should I be concerned, and will I always get them now?
Not easy questions to answer! If you have a family history of migraine, you could develop migraine at any time, and migraine with aura is more likely to occur for the first time during pregnancy. It is important that you ask your doctor for a full assessment in order to confirm that there are no symptoms, or ‘red flags’, to cause concern, and make sure that on examination there are no abnormalities to be found to suggest a structural cause.
Aura tends to follow a typical pattern and, provided that what you experience fits with what is regarded as normal, there is little cause for concern. If the aura symptoms are not typical, your doctor might refer you to a neurologist, to exclude any possible ‘sinister’ cause, especially when they occur for the first time.
I’m afraid it is impossible to say whether your migraine will continue after the baby is born. Only time will tell. My migraines have settled while I have been pregnant but what’s going to happen when my baby arrives?
If you are lucky, you may not get a ‘rebound’ effect immediately after the baby arrives. Unfortunately, the evidence suggests that as many as 40% of women who have migraine get their migraines back after the baby is born.
What can I take to treat my migraine while I am pregnant?
Hopefully, you won’t get many migraines while you are pregnant, because your options are limited in real terms to paracetamol. If you get significant symptoms and their severity justifies using other drugs to aid the nausea and vomiting, you could take an anti-nausea drug, but this may be discouraged in the way that the use of any drug during pregnancy is discouraged. See the next few answers for more information. Some people have found that ginger in its various forms – biscuits, tea, cordial – may help some of your nausea symptoms.
I have been told that all I can take for my migraine while I am pregnant is paracetamol. Why can’t I take anything else?
As I am sure you know, no drug is encouraged during pregnancy other than iron supplements and folic acid. The reason for this is that at any stage in the pregnancy a drug might have an effect on the growth and development of the baby. Different drugs tend to have different effects and degrees of effects at different stages of the pregnancy.
Over time a database has been built up to try to evaluate exactly what effects drugs have. This information tends to be ‘opportunistic’ (not the result of scientific research), and often reflects the fact that women have taken drugs in the very early stages before they realized they were pregnant.
Deciding to take anything during pregnancy is about balancing the potential risk of the drug affecting the developing baby and the potential consequence of not managing a problem that needs treating. Discuss the benefits and risks with your doctor or midwife before making a decision.
What can I do if my migraine gets worse while I am pregnant?
Any drug is best avoided in pregnancy. Preventing migraine by following a diet and lifestyle regimen that will keep your threshold as high as possible is a vital first step to staying in control. Making a decision to take drugs is about weighing up the risks and benefits to you and to your baby, which do change in the different stages of pregnancy.
Some drugs that are used to treat migraine are also used for other conditions, and occasionally the potential benefit may well outweigh the theoretical risks of using these drugs in pregnancy.
Talk to your doctor or midwife about lifestyle changes you can make now and what the options might be if your migraines get worse.
How does the specialist decide what I can take to treat my migraine while I am pregnant?
It is never an easy decision to make and tends to depend on the severity of the symptoms you are experiencing and whether the benefit of taking something outweighs the risk. Some drugs, such as beta-blockers and antidepressants, that can be used to treat migraine, are also used to treat high blood pressure and depression during your pregnancy. These drugs are introduced because not treating the high blood pressure or depression would have a detrimental effect on both mother and baby. Starting these drugs to treat migraine does depend, though, on whether you feel that the possible risk is worth it.
I am taking a preventative drug for my migraine but want to get pregnant. Do I need to stop it?
It is a good idea to stop and see what happens to the frequency of your migraines as a result. The probability is that things will be OK. The advice will always be ‘avoid any drug during pregnancy’ if at all possible. Some drugs carry a lower risk of harm than others, but taking any drug needs careful thought and consideration.
Beta-blockers:
- Cause intra-uterine growth retardation (slow the growth of the baby in the womb)
- Cause bradycardia (slowing of the heart rate) after birth
- Cause hypoglycaemia (very low blood sugar) after birth Anti-epilepsy drugs (AEDs):
- When used to treat epilepsy the risk of harm outweighs the risk of treatment
- When used to treat epilepsy the risk of harm increases if more than one drug is used at the same time
There is increased risk of neural tube (spina bifida) and other defects associated with any AED but especially with:
- Epilim (sodium valproate)
- Carbamazepine
- Oxcarbazepine
- Phenytoin
If I stop my preventative drug, will my migraines get worse? If they do get worse, what can I do?
There is no way of knowing if they will get worse but they shouldn’t. No preventative drug is taken permanently, so they will have to be stopped some time. The best way to stop it is to reduce the dose slowly, in steps, until you stop taking it altogether. During the
phase of ‘stepping down’ and stopping the drug you need to really focus on the diet and lifestyle areas to keep your migraine threshold as high as you can.
I am planning to breast-feed and wondered what I can take to treat my migraine?
Paracetamol is top of the list. If you need something different, you could try ibuprofen but aspirin and other NSAIDs are to be avoided, as should codeine. If you need something to help the nausea and/or vomiting, opt for domperidone rather than metoclopramide; you could try prochlorperazine if you cannot tolerate domperidone.
CONTRACEPTION
My sister, who also gets migraine, was told she could not go on the Pill. Why is that?
It rather depends on what sort of migraine she gets. If she gets migraine with aura, current guidelines recommend that she should not go on the combined oral contraceptive pill – that is to say, she can’t take a Pill containing oestrogen. However, there is no reason why she can’t use the progesterone-only pill, progesterone injection or progesterone-containing coil.
I have been on the Pill for about two years. I got an aura with my last two attacks, and my doctor has told me to stop taking the Pill. Why do I have to stop?
It is all to do with risk and your risk of developing a stroke, specifically an ischaemic stroke. An ischaemic stroke occurs as a result of a reduction or loss of blood supply to part of the brain. It is estimated that between 1 and 3 women per 100,000 women under the age of 35 years may experience an ischaemic stroke. On an individual level your chance is very low but there are other risk factors that need to be considered and migraine is one of them. Other factors include smoking, being overweight and taking the combined Pill.
Having migraine increases your chance of having a stroke by three and a half to four times. Migraine with aura carries twice the risk of migraine without aura. If you smoke and have migraine, your risk is increased by ten times. Taking the Pill and smoking increases your risk by 34 times.
As you can see, the risks tend to be cumulative. Although the absolute numbers are quite small, the nature of the cumulative risk cannot really be ignored and the fact that you have developed aura is the decider.
Why has my doctor told me that if I want to stay on the Pill I should stop smoking?
If you have migraine without aura and more than one risk factor for stroke, you should stop the Pill – assuming you mean the combined oral contraceptive (COC) pill. Smoking is a potent risk factor, and having migraine and being a smoker and being on the COC pill is not a wise mix. All these, as well as other risk factors such as being overweight or having a high cholesterol, are reasons to think about stopping the Pill.
I know I am overweight but I need reliable contraception. I have been told that, because I smoke, I really should not go on the Pill. Why not?
If you have migraine without aura and want to go on the combined oral contraceptive (COC) pill, you should either lose weight or stop smoking – or, ideally, both. It is about cumulative risk factors and too many risks become a ‘no’.
If you feel unable to do either of those things, you need to consider a contraceptive option that does not involve oestrogen. From a hormone point of view, that would be the progesterone-only pill, progesterone injection or coil.
Topiramate works really well as a preventative drug but I’m having problems with using the Depo injection for contraception. Why can’t I go back on the Pill?
Topiramate is an anti-epilepsy drug that is known to stimulate or induce liver enzymes to work harder. This means that any drug that is processed by the liver before getting into the circulation is broken down or inactivated more quickly, and so less of the drug is active or ‘bioavailable’ to do the job it is meant to do.
Any drug taken by mouth has to be processed by the liver and its bioavailability is affected as a result. Going back on the Pill is possible but it would be less reliable from a contraceptive point of view, because more of the hormone would be broken down by the liver and less would be available to have its contraceptive effect.
I have been started on topiramate for my migraine. What are my contraceptive options?
Your best options, in terms of effectiveness and reliability, would be progestogen-only injections or the LNG-IUS (levonorgestrel intra-uterine system). The former is given every 10 to 12 weeks and the latter is a coil that is impregnated with progestogen that is slowly released within the womb; once fitted, the coil can stay in place for five years.
I am keen to go back on the Pill despite being on topiramate, as it controls my periods better than the injection. What can I do to make it more reliable as a contraceptive?
You could go back on the Pill but you would have to double up on your contraception in order to increase the contraceptive effect. You could do this by taking a stronger pill – a 50 μg pill, which is no longer available as a standard ‘off-the-shelf’ prescribable option, so you would have to double up with one that is still available or you might opt to use condoms with or without spermicides. You will need to chat to your doctor or visit your local family planning clinic for more advice.
I want to stay on the Pill, as it suits me really well. What could I take to reduce the total number of migraine days I get?
You could try valproate, gabapentin or levetiracetam. These are all anti-epilepsy drugs that will not have an effect on the contraceptive reliability of your Pill and have all been shown to have some effect in preventing migraine – they are not liver enzyme ‘inducers’.
I am on the Pill, having been using condoms while taking topiramate, which I’ll be stopping soon. How long do we need to carry on using condoms?
You should continue to use condoms for four weeks after you have stopped taking topiramate. This allows your liver enzymes to get back to normal so that the Pill can work as effectively as possible, once its bioavailability is back to normal.