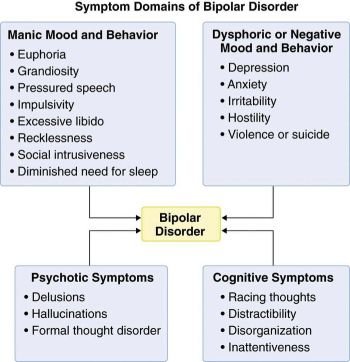
What does a Bipolar Disorder episode look like?
Bipolar Disorder and Addiction

Why is my doctor telling me I need treatment for my addiction when I thought treating the depression would solve my problem?
Patients with a combination of addiction and depression are at higher risk for suicide, homicide, poor compliance, relapse, and greater hospitalization rates. Although there is some evidence to support the concept that many patients use substances to “self-medicate” an underlying depression, there is no evidence that antidepressant medication leads to abstinence. Although the “self-medication hypothesis” may seem right for some individuals, once an addiction develops it takes on a life of its own. It is unlikely that medicating it away can conquer addiction.
Also, if you continue to use drugs or alcohol while receiving antidepressant medication, they render antidepressant medication essentially ineffective. Thus depression cannot be effectively treated without also treating the addiction. However linked they may have been in their origins, they are now separate entities that both require treatment in order for you to return to health.
How are alcoholism and bipolar disorder connected?
Bipolar disorder and alcoholism do co-occur at higher than-expected rates. No one knows why but it appears, surprisingly, that they are not genetically linked. Bipolar men who are alcoholics often had a family history of alcoholism when compared with nonalcoholic bipolar men. Alcoholism among bipolar women, however, was not associated with a family history of alcoholism.
Instead, their addiction often stemmed from anxiety and depression. Bipolar women have a higher risk of developing alcoholism than non-bipolar women. The rate in bipolar women for alcoholism is 29%, and in bipolar men it is 49%.
More importantly, alcohol, cocaine, heroin, PCP, and marijuana can all cause mood swings that make everyone using these drugs suspect of having a mood disorder in general and bipolar disorder more specifically. When these patients are hospitalized psychiatrically as a result of an impulsive, potentially dangerous behavior in the context of their drug and alcohol abuse, the likelihood of their being discharged on a “cocktail” of psychiatric medications with a diagnosis of bipolar disorder is high. With average lengths of stay in a psychiatric hospital of about a week the accuracy of such a diagnosis is suspect at best.
The proof is not even in the pudding, because complicating the picture is the fact that the medications one is discharged on are symptom and not diagnostic specific.
Therefore, although one’s mood may stabilize with an anticonvulsant agent or antipsychotic that does not mean one has bipolar disorder. Unfortunately, the pitfall inherent in the diagnosis is that all too often these patients and their families focus entirely on the bipolar diagnosis, attributing continued relapse into drugs and alcohol to bipolar disorder while doing nothing to get treatment for substance or alcohol abuse. Alcohol and drugs of abuse worsen bipolar symptoms and go further toward explaining the mood swings than vice versa. More likely, any mood swings stand a far better chance of improvement from abstinence than from any psychotropic medication offered.
Are individuals with bipolar disorder at risk for drug abuse?
Alcohol and drug abuse is very common among people with bipolar disorder. The most common co-occurring illnesses with bipolar disorder are substance abuse disorders, with up to 60% of patients with bipolar disorder having substance-related problems. Substance abuse can make bipolar disorder more severe and worsen the course of the disease by exacerbating symptoms or precipitating episodes. Such comorbidity may result from the self-medication of mood disorder symptoms, or mood symptoms may be induced by substance abuse. The risk of comorbid substance abuse may be increased by family history of substance use, an early age of onset of bipolar disorder, and the presence of mixed episodes. Treatment for co-occurring substance abuse, when present, is an important part of the overall treatment plan. The diagnosis of bipolar disorder should not be made in the presence of active substance use, as many illicit drugs (and the rapid withdrawal from them) can cause symptoms of mania (and subsequent depression). Ideally the substance of use is discontinued so that a baseline of functioning can be assessed. Symptoms should dissipate if due to an ingested substance. If substance abuse persists, treatment for presumed bipolar disorder may be initiated if co-occurring substance abuse treatment is obtained. Even if self-medication of symptoms was the reason illicit substance use was initiated, once abuse or dependence has set in, the problem will require separate treatment.
Since returning from active duty overseas, my husband is having rageful episodes, is irritable, is suspicious of others and complains of racing thoughts at night. Is he bipolar?
Active duty can be a precipitating stressor for many mental disorders. As part of any evaluation, various diagnoses are considered because of overlapping symptoms.A common combat casualty for many soldiers returning from war is posttraumatic stress disorder (PTSD). Symptoms of PTSD can look very much like a mood disorder, and in fact untreated PTSD often results in development of depression and substance abuse. In some studies as many as 52% of subjects develop alcohol abuse or dependence and 47% develop depression. In a person who is at higher risk for bipolar disorder, it is certainly plausible that the first episode would occur following as stressful an event as active duty in combat. In fact, in a recent NIMH-funded study, a high percentage of persons diagnosed with bipolar disorder also exhibited symptoms of PTSD. Symptoms of PTSD may look like bipolar disorder, however.
PTSD is associated with three primary symptoms that persist for longer than a month after a traumatic event:
• Re-experiencing, such as flashbacks or nightmares or intense memories
• Hyperarousal, such as jumping at noises one used to ignore
• Numbing, such as an inability to feel pleasure and a tendency to isolate
With re-experiencing, there are recurrent, intrusive thoughts and images in the mind. The patient may exhibit behavior as if the events were recurring, and intense psychological distress can occur. Re-experiencing can result in irritability and agitation. Racing thoughts may actually be the recurrent memories and ruminations. Symptoms of hyper arousal include difficulty sleeping, outbursts of anger, difficulty concentrating, and hyper vigilance. Symptoms of numbing include detachment and avoidance, which can look like depression. The cluster of symptoms can thus look very much like bipolar disorder. In a recent study of U.S. soldiers returning from Iraq, about 16% said they were experiencing symptoms of depression and anxiety.
Although their symptoms are likely to be caused by PTSD, it is important to rule out bipolar disorder because the treatment for PTSD is typically an antidepressant, which would not be indicated during an acute hypomanic or manic episode. The sad truth is, though, that many if not most soldiers will not admit to having a problem or seek help. They have been trained to “suck it up,” and they consider any admission of emotional problems related to their duty as an admission of weakness in the face of their responsibility.
The earlier your spouse gets into treatment, the better the chance for a positive outcome.
Terms:
Re-experiencing – the phenomenon of having a previous lived experience vividly recalled and accompanied by the same strong emotions one originally experienced.
Hyperarousal – a heightened state of alertness to external and internal stimuli, often results in sleep disturbance, problems concentrating, hypervigilance, and exaggerated startle response. Typically seen in posttraumatic conditions.
Numbing – the psychological process of becoming resistant to external stimuli so that previously pleasurable activities become less desirable.
Ruminations – obsessive thinking over an idea or decision.