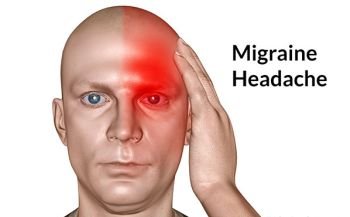
Migraines are quite common among people with bipolar disorder
Migraine and Bipolar Disorders

INJECTION OF THE GREATER OCCIPITAL NERVE
Nerve ‘blocks’ have been used to relieve the pain in a variety of situations and medical conditions, including the following:
- Pain control during surgery, avoiding the need for a general Anaesthetic
- Pain control for patients with fractured bones
- Neuralgia resulting from local injury or trauma to the nerve
- Nerve pain caused by cancer
What is a nerve block?
Anerve block is a way of altering or modifying the response of a nerve so that pain cannot be felt or experienced. It can be done in a variety of ways, including the injection of a local anaesthetic, usually between the site of injury or damage and the spinal cord, thereby altering the pain response.
Another method uses a high radiofrequency signal that causes the nerve to become hot, resulting in damage to the nerve and thus in a permanent break of communication between the nerve, the spinal cord and therefore the brain. Traditionally this was done by heating the nerve to 80ºC for 60 to 90 seconds, resulting in the destruction of the nerve. Currently a ‘pulsed’ method is used with a more gentle process, gradually heating the nerve to 42ºC for 10 to 15 minutes, which means that the nerve is not destroyed but the pain response is altered.
In some patients – usually only those with life-threatening or terminal conditions – the nerve might be destroyed by injecting it with a solution designed to kill it.
What is used when doing a nerve block?
Different specialists and different centres use different drugs and drug combinations. Generally, a local anaesthetic is used and this can be combined with a steroid. Studies looking at occipital nerve block have considered both local anaesthetics alone and local anaesthetic combined with steroid.
What can be done to make the nerve block as effective as possible?
Generally speaking, the right balance of local anaesthetic and steroid must be used and has to be injected in the right area to produce the desired nerve block.
Are nerve blocks safe?
In the right hands, yes, they are but remember that no procedure or intervention is totally without risk. There is always the chance that the nerve is missed and no benefit achieved. There is a chance that an infection may develop at the injection site but if appropriate sterile techniques are used this should not occur. If the needle is slightly out of position then other nerves may be affected, but this effect will wear off. If too much drug is used, the effect may be prolonged – often not a bad thing.
What is a greater occipital nerve block?
The greater occipital nerve is shown in Figure 16.1. The nerve is located by the clinician who is doing the block, using specific markers on the scalp, and the area is palpated (felt) to find where there is maximal tenderness – basically where it hurts the most. The skin is cleaned, the needle is inserted and a mix of steroid and local anaesthetic is injected over an area designed to produce an adequate block.
What is the evidence that greater occipital nerve block is effective for headache symptoms?
The evidence, as always, is mixed. Some studies show that it can help some headaches but others are less conclusive. There is no doubt that nerve blocks are very helpful in the management of neuralgia, but the current evidence base is by no means conclusive in relation to headache.
There must be a range of good-quality double-blind placebocontrolled trials looking carefully at the response to occipital nerve blocks in patients with each of the different types of headaches, including migraine, tension-type headache and medication overuse headache as well as cluster headache.
WHAT ABOUT ‘HOLES IN THE HEART’? PFO AND MIGRAINE
Of all the things to hit the headlines recently ‘hole in the heart’ – patent foramen ovale (PFO) – has, in many ways, been the most exciting but also the most controversial. There is no doubt that there is an association between a PFO and migraine. There is also no doubt that closing a large PFO to try to prevent stroke may be appropriate, but the big question is: are the potential risks of surgery worth it in the context of migraine? At the time of writing, the evidence does not support PFO closure, despite the high level of interest and enthusiasm generated by anecdotal evidence.
What actually is a patent foramen ovale?
Aforamen ovale is the opening between the two upper chambers of the heart – the atria (singular = atrium) – that allows the blood to circulate oxygen safely and effectively in the fetus (baby) during pregnancy. After the baby is born the foramen ovale closes in 75–85% of cases. If it remains open, it is called ‘patent’, hence the term patent foramen ovale, or PFO.
The atria normally allow blood to pass from the venous circulation to the ventricles. On the right side this means blood passes from the body to the right ventricle and from there to the lungs, collecting oxygen along the way before passing back to the left atrium, to the left ventricle and from there back to the body.
What conditions might be associated with a PFO?
APFO has been recognised coincidentally at post-mortem in up to 30% of individuals. Most people with a PFO have no symptoms related to its presence. As patients with specific medical conditions are looked at more closely, the picture seems to change a little, but this is an association; deciding on cause and effect is something else again.
- Stroke: In people who have had a stroke under the age of 50 years, between 40 and 60% had a PFO; the larger the PFO the more likely they were to have had a stroke.
- Divers: As many as 60% of divers who have had recurrent bouts of decompression sickness (‘the bends’) have been found to have a PFO.
- Migraine: Studies so far have found that 22–57% (higher than the ‘control’ population) of patients with migraine with aura have a PFO, and 14–21% (similar to the ‘control’ population) of those with migraine without aura have a PFO.
How can a PFO be diagnosed?
There are a variety of techniques used to diagnose a PFO, including:
- Transthoracic echocardiography (TTE, through the chest)
- Transoesophageal echocardiography (TEE, through the oesophagus, the tube from the back of your throat to your stomach)
- Transcranial Doppler (TCD) imaging (through the base of the skull) An echocardiogram is a way of looking at how the heart is pumping.
It uses ultrasound waves to produce a visual display of the heart on a monitor.
A contrast transthoracic echocardiogram was used to screen patients for the MIST (Migraine Intervention with STARFlex Technology) study.
The MIST study was the first to have a placebo, or sham, part to the study. Patients selected for the study had migraine with aura and had failed to respond to two previous preventative drugs. Patients in the placebo group were taken to the catheter lab, anaesthetised and had an incision made so they had no way of knowing whether they had had a device fitted. This was done because it was recognised that the highest quality study was needed to answer the questions relating to PFOs and migraine, and whether PFOs should be closed if found in migraine sufferers.
How can a PFO be closed?
PFOs are closed using any of a variety of devices; the one used in the MIST trial was called STARFlex. This can best be described as a double-layered umbrella that, when opened, can sit either side of the hole and cover it up, hence it is ‘closed’.
How does the implant get to where the PFO is in the heart?
Atube (catheter) is inserted into the femoral vein (a vein in the leg) and moved through the venous system to the heart. This is done in a sterile operating theatre under the guidance of echocardiography, which allows the surgeon to see exactly where the catheter is and to make sure it is put into the right place.
The safety of this sort of procedure depends in large part on the skill of the surgeon. No procedure is without risk but complications on the whole are fortunately rare; they include:
- Short-lived heart arrhythmias (irregular heart beats)
- Damage to the vein, or bleeding at the site where the catheter is inserted
- Damage to the heart muscle
- Reaction to medication used during the procedure
In the MIST study the complications in the active group included:
- Cardiac tamponade (pressure on the heart from fluid collecting in the sac around it)
- Pericardial effusion (fluid collecting in the sac that surrounds the heart)
- Retroperitoneal bleed (bleeding within the abdomen)
- Atrial fibrillation (an irregular heart beat)
- Chest pain
And in the placebo, or sham, group:
- Bleeding at the incision site (where the catheter is inserted)
- Anaemia
- Nose bleed
- Brainstem stroke
Will closing a PFO really cure migraine?
The answer to your question is that closing the PFO will not completely ‘cure’ your migraine. It may reduce the number of headache days you have but so will a variety of other drugs or interventions. Closing a PFO is not without risk and needs to be considered
very carefully. The MIST study showed that there was a 37% reduction in the number of headaches in the intervention group compared with 17% in the placebo group. This suggests that closing the PFO on the basis of the current evidence is no better than current preventative options