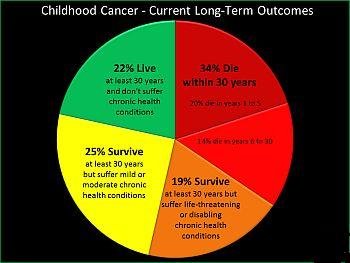
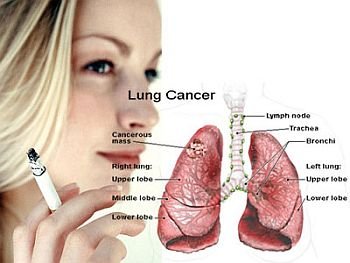
Control of Tumor Promotion and Metastatic Progression by Inflammatory Signaling
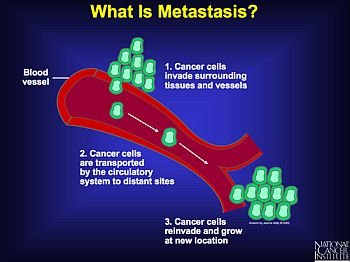
Metastatic Disease: Cure versus Control
The mainstay of treatment of metastatic cancers is drug therapy. Whether they are injected or swallowed, drugs travel throughout the body to reach cancer cells wherever they are hiding. These treatments may be administered for brief or extended periods, depending on the type of cancer and goal of treatment.
Treatment “goals” are defined by what can be realistically achieved given all available and experimental approaches. Although cure is always desired, the reality is that the best we can hope for with many cancers is long-term control.
A patient’s oncologist will make the goals of treatment clear. The two examples that follow illustrate the approaches to treating cancer for cure or for control.
THE NATURE LOVER
Robin, a forty-five-year-old woman with an affinity for natural healing and a love of animals, feels a mass in her abdomen one day. After testing, she is ultimately diagnosed with stage IV non-Hodgkin’s lymphoma involving the liver. She undergoes six courses (cycles) of chemotherapy plus an immune therapy (CHOP-Rituxan, see chapter 3), followed by small doses of chemotherapy administered by spinal tap into her spinal fluid to prevent lymphoma from growing in her central nervous system.
The treatment is hard. She loses her hair and at various times experiences weakness, nausea, pain, and discomfort. But three months later she is back to work, feeling well, with a new short hairdo. Four years later, Robin remains cancer-free and has much longer hair.
THE PAINTER
Patrick, a seventy-year-old accomplished painter, is diagnosed with stage IV prostate cancer involving his bones five years after he underwent surgical removal of the prostate. He is treated by his urologist with injections of a hormone-blocking drug (Lupron) every four months to keep the cancer in check. After two years, the PSA (blood marker of cancer growth) rises again, and he is prescribed a pill (Casodex) to block the ability of testosterone to fuel the cancer. By this time, Patrick has stopped painting, mainly from depression at the thought of dying soon. He is referred to me for management of his cancer at this point.
The new medicine lowers the PSA for six months, but then the PSA begins to rise again, and a bone scan shows worsening of the cancer. The Casodex is stopped, but the PSA continues to rise (it can sometimes fall in this situation). Patrick learns that his estimated average survival at this point is approximately two years. He begins another hormone-blocking pill called ketoconazole; the PSA plummets to the normal range, and he feels well. He begins to paint again and even travels abroad for inspiration.
After a year and a half, the PSA begins to rise swiftly, and Patrick feels weak; he stops painting. We change treatment to intravenous injections of the chemotherapy drug Taxotere, given once every three weeks. The PSA steadily declines and after six treatments is close to the normal range. The chemotherapy tires him for about a week, leaving two good weeks out of every three to accomplish things. After eight cycles, the treatment is put on hold to give him a break from therapy and liberate him from frequent office visits and needle-sticks. Patrick does not feel that he is dying anymore; he travels, paints, and enjoys the company of his loved ones. After six months, the cancer again becomes active, and he resumes treatment in a clinical trial testing a new drug. The situation remains stable for a few months but then requires that he go back on chemotherapy.
The cancer responds, and his condition improves once again. It is now three years since he expected to live between “one and two.” Patrick knows the cancer cannot be cured. He knows he will need to be on and off treatment for the rest of his life. But, he says, “I am so grateful. I didn’t expect to be here now. I don’t know how much time I have but, life on the whole is very good.”