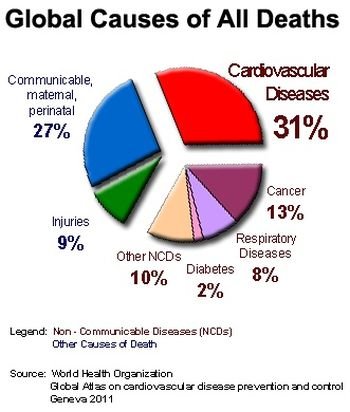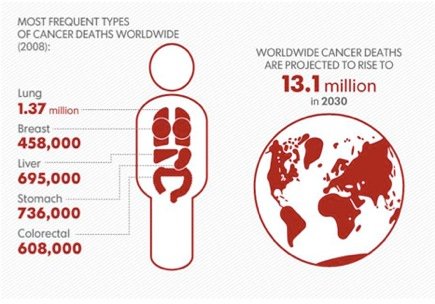
Cancer is the uncontrolled growth and spread of cells. It can affect almost any part of the body. The growths often invade surrounding tissue and can metastasize to distant sites. Many cancers can be prevented by avoiding exposure to common risk factors, such as tobacco smoke. In addition, a significant proportion of cancers can be cured, by surgery, radiotherapy or chemotherapy, especially if they are detected early.
Alternative and complementary approaches to cancer care
Research shows that at least half of cancer patients use complementary or alternative medicines in addition to conventional medicine (and one suspects that a lot of the remainder are simply not telling us). These come in many varieties and include traditional therapies used by patients from ethnic minorities. Although the terms ‘complementary’ and ‘alternative’ are sometimes used interchangeably, it is helpful to distinguish between different varieties of what may be termed to be outside mainstream medical practice. I will, therefore, refer to complementary medicines as those aimed at running alongside conventional therapies as a form of support. An example would be aromatherapy, which does not fundamentally conflict with the patient continuing their conventional therapy. Indeed, aromatherapy may aid compliance with treatment or reduce the need for additional medications such as laxatives or painkillers. As well as quasi-medical therapies like aromatherapy, there are treatments such as acupuncture and homoeopathy that may be available both via mainstream healthcare and via other ‘therapists’. Alternative medicines, on the other hand, are aimed at replacing the mainstream treatment with one that conventional medicine would regard as unproven at best and harmful at worst. In practice, it is impossible to rigidly separate treatments into one or other category, as while one patient may use a remedy alongside the conventional, another may use the same remedy in place of it – the distinction is one of intent as much as content.
There are a huge number of different alternative and complementary medicines, including homoeopathy, acupuncture, dietary therapies, herbal remedies, aromatherapy, as well as techniques such as crystal therapy, visualisation, and traditional therapies used by ethnic minorities. A full analysis of each of these is beyond the scope of this text, so I will try and select a few examples to make general points about how complementary and alternative treatments interact with cancer therapy. Before doing so, it is worth getting a feel for the massive extent of usage of such treatments. While countries may vary, usage in the USA is likely to be pretty typical of use in the developed world. As it is easy to quantify spending in the USA, I will give a breakdown of recent figures produced by the American National Institutes of Health. The headline figure is that 88 million Americans spent $33.9 billion on complementary or alternative medicines in 2007. This amounted to over 10% of all ‘out of pocket’ expenditure on health in the USA. In addition, a further $23 billion was spent on vitamin and mineral supplements. Given the very high medical bills faced by US citizens, it is clearly astonishing that they would spend such a sum in addition. At the 2007 exchange rate, this would have provided all health care for the UK population for about 6 months. These figures clearly relate to total expenditure, not money spent specifically by cancer patients; however, they do give a good feel for the extent to which these treatments are used. Similar expenditures occur in all industrialised countries. Why do citizens in all the most educated societies in the world, generally provided with healthcare which, as we have seen, keeps most of them alive into old age, shell out such huge sums on additional, mostly unproven, therapies? Clearly, in less wealthy societies, traditional remedies may be all that part of the population can afford, and thus different forces may be at play. Before moving on to try and address this, it is worth looking at a breakdown of what the money goes on. Again, I will refer to the US figures, and clearly, the split elsewhere may vary, but I believe it gives a feel of the sorts of things people want. If we understand that, it may help explain the paradox above. The biggest category in the US report is described as ‘non-vitamin, non-mineral natural products’. These are presumably herbal remedies of various sorts – as already noted, this excludes the expenditure of around $23 billion on vitamin supplements and minerals such as selenium. A further $4.1 billion is spent on techniques that focus on mental wellbeing with or without a component of exercise – yoga, for example. Clearly, it is debatable whether these really belong here as the individual’s motivation is clear – it makes them feel good. As this clearly is a benefit in itself, I do not think further discussion is necessary. The same applies to the $0.2 billion spent on relaxation techniques.
Most of the remainder is either grouped as practitioner costs ($11.9 billion) or homoeopathic medicine $2.9 billion (it’s not clear whether this reflects the ‘medicines’ themselves or the total cost including practitioner fees). Either way, this is an astonishing sum to have been spent in a society as litigious as the USA. For a practitioner of conventional medicine, the route to a licence is long and heavily policed. Any licensed drug will have been through stringent approval procedures to demonstrate efficacy, safety, and fitness for purpose. Thus both the practitioner and products used are heavily regulated. Step outside the rules and stringent penalties apply both to practitioners and sellers of medicines and devices. Failure of either to perform to the expected standard will result in legal and often financial penalties. In conventional medicine, a drug company cannot legally sell a treatment for, say, asthma without evidence that it works a reasonable amount of the time. For a most alternative and complementary medicines, no such tests apply in most countries. Regulation is either absent or internal to the ‘specialty’. No tests of efficacy apply to, for example, homoeopathic medicines. Why the practitioners of these specialities are not subject to these basic rules is a mystery. Even if different rules applied, in other walks of life to charge for a good or service on the basis that it has certain properties will be subject to legal penalty if the item does not fulfil the advertised function.
The truth is that the purveyors of these remedies appear to believe that they work and their patients do likewise. Alternative and complementary therapies are therefore in reality more akin to religion than science, and this goes a long way to explaining their apparent immunity to the law, as religion itself enjoys the same degree of legal privilege in most countries. Furthermore, there is a well-known phenomenon observed in clinical trials called the ‘placebo effect’. Patients in blinded trials where some are taking dummy pills called placebos will often experience the beneficial effects (and bizarrely, sometimes the minor side effects) expected from the active drug. This effect is often substantial and is in many ways highly desirable – there is clearly no risk of serious drug-related adverse events. The body is healing itself. Clearly, therefore, if the alternative ‘practitioner’ and the patient collude in a belief that a treatment works, it often will. Does this mean it is an honest practice?
In my opinion, it does not – I believe these remedies should be subject to the same tests of efficacy as any other product, whether medicinal or not. Furthermore, it is not the case that no harm is done by an ineffective product – it depends on how it alters the treatment of the patient. Clearly, if, say, homoeopathy is used for a minor, self-limiting condition such as soft tissue injury, then no long-term harm is likely. If it is used in place of a standard therapy for cancer, AIDS, or tuberculosis (as some of its proponents advocate), then clearly deterioration can occur while the patient is forgoing some more effective therapy.
As already discussed, the gold standard way to assess any medicine, conventional or otherwise, is in a controlled trial. These are widely used to assess conventional medicines but have also been used to test complementary or alternative medicines such as homoeopathic remedies as well as with techniques like acupuncture (where the control is sham acupuncture – a needle is inserted but in the ‘wrong’ place).
The basis of homoeopathy is that ‘like cures like’. Practitioners take compounds that induce a symptom, say, nausea, and then dilute the active compounds sequentially to the point when not a single molecule of the original substance remains. Proponents claim that the ‘potentizing’ involved in making a homoeopathic remedy somehow ‘imprints’ the water molecules with properties that will have medicinal effects. The effects are generally held to be the reverse of the symptom induced by the agent the homoeopathic pharmacy began with – hence the medicine from the example above would be used to treat nausea. For such a therapy to be effective would require a reworking of a substantial body of physics, chemistry, and tissue biology, all of which is currently lacking. Even if we concede that our knowledge of these disciplines is imperfect, it is not unreasonable to expect that there would be evidence from clinical trials of effectiveness. If there were convincing trial evidence of efficacy, clearly the underlying scientific orthodoxy would need to be re-examined to accommodate the new evidence. We, therefore, need to examine the clinical trial evidence for homoeopathy.
A number of controlled trials of homoeopathy have indeed been carried out. In 2005, the respected medical journal The Lancet published an article analysing the results from 110 trials of homoeopathy that included a placebo. These trials were compared with 110 similar trials of conventional medicine (referred to in the homoeopathy literature as allopathy, meaning ‘other than the disease’). The Lancet article concluded there was no evidence of a coherent effect from homoeopathy that could not be explained by the placebo effect. In contrast, the conventional trials were able to show effects from conventional medicines over and above the placebo in similar conditions. Homoeopathy would thus seem to sit solidly in the ‘alternative’ category as its practitioners promote it as exactly that, an alternative to conventional medicine. With no evidence of solid benefit, this seems an irresponsible view to take, especially as homoeopathy is promoted for use in all manner of diseases including potentially lethal conditions such as asthma, tuberculosis, and AIDS. This view is endorsed by bodies such as the World Health Organization (WHO) which recently issued a warning stating that the use of homoeopathy to treat conditions such as tuberculosis and malaria was dangerous, and it said quite categorically that lives were being lost as a result. Hence on every level, when the ‘science’ of homoeopathy is examined, it clearly poses problems by the yardsticks of conventional science – there is no coherent physical basis for its mode of action, nor convincing trial evidence of efficacy. Despite this lack of evidence, homoeopathy is available on the NHS in the UK, and millions worldwide, including the Prince of Wales, believe in its effectiveness.
So why do so many patients use these treatments? Most people have only the sketchiest understanding of science and tend to view the claims of scientists and alternative practitioners as
equally valid alternatives. This view is peculiarly limited to biology – no one wants to use ‘alternative’ approaches to, for example, engineering or piloting an aero plane; they stick with the laws of aerodynamics and trained pilots. I believe that in many, if not most, cases, people are simply desperate and want to hedge their bets by backing both horses. Patients who have run out of curative conventional options often pursue these therapies and are clearly vulnerable to exploitation. Extreme varieties of these treatments often require the patient to travel to countries where regulation of such therapies is less strict than it is within, says, the USA or the European Union. Patients also frequently adopt unusual dietary approaches. Often, the underlying rationale, if there is one, will mix cause and effect. The logic underpinning these diets often runs something like this: the risk of getting a number of cancers may be increased by a lack of X in the diet (possible), therefore taking X will restore balance and treat the cancer. This leads to patients taking, for example, vitamin or mineral supplements. As a proposal, this is at least testable – we can do a trial with the supplement in question and see whether it impacts on the outcomes experienced by patients. Another common theme in anticancer diets is to pick a particular component of the diet, such as animal fat – the underlying logic being that a number of common cancers have been linked to an excess of animal fats in the diet, therefore giving up animal fats will treat cancer (unlikely). Substituting the word ‘smoking’ for ‘animal fats’ in lung cancer illustrates the futility of this – if all you had to do to treat lung cancer was stop smoking, far fewer would die from it. Sadly, stopping smoking has very little impact on the grimly predictable outcome of most lung cancer. Similarly, evidence that these sorts of ‘subtraction’ diets impact cancer survival is also conspicuous by its absence. Another more recent example I have observed in patients turning up in my clinics is the claim that eating sugar is bad, as this ‘fuels’ cancer. As all complex carbohydrates are digested down to sugars in the gut before being absorbed, this is highly unlikely to be a good therapy, especially as organs such as the liver and pancreas very tightly regulate sugar levels in the blood.
Despite the flawed logic and lack of evidence, patients will often adopt new diets in response to a diagnosis of cancer, frequently giving up foods enjoyed for decades to adopt a diet with alleged ‘detoxification’ or ‘healing’ properties, or adding supplements to ‘boost’ the body’s defence mechanisms. At the extremes, both practitioners and adherents often promote these approaches with a fervour approaching the religious. Indeed, adherence to these doctrines in many ways parallels religious observance, with denial and self-sacrifice being potentially rewarded by improved wellbeing.
Like religious observance, direct evidence of efficacy is not required – belief that it works is sufficient. Furthermore, failure of the technique to work can be interpreted as an indication of insufficient diligence in the application of the regime rather than an indication of lack of efficacy. In 1990, a team of three of us (two oncologists and a psychiatrist) visited the Gerson Centre in Tijuana in Mexico. The Gerson plan is based on a curious mix of a ‘detoxifying’ diet (vegan, crushed fruit and vegetable juices, no added salt) and the frankly odd (regular fresh coffee enemas). Dr Max Gerson developed the diet to treat various ailments, including diabetes (he treated Albert Schweitzer) and tuberculosis. Ironically, he was driven from the USA for advocating the diet for diabetes, at the time treated with a high-fat, low-carbohydrate diet. It subsequently turned out that the ‘Gerson’ high-fiber, low-fat diet actually was a good treatment for diabetes, but this was only realised many years later.
This does demonstrate the need to evaluate therapies in a scientific way – when this was done, it proved the value of low-fat, high-carbohydrate diets for diabetes. However, after being expelled from the USA, Gerson continued to advocate the therapy for a range of other conditions, including cancer, heart disease, and arthritis. The US National Cancer Institute carried out investigations in 1947 and 1959 to assess whether the Gerson regime had any effect on cancer outcomes, concluding both times that there was no convincing evidence of a treatment effect. Our own review of cases selected by the Centre in 1990 came to the same conclusion, which we published in the medical journal The Lancet. Patients at the centre undoubtedly believed they were benefiting, and in a sense, for the reasons outlined above, they were getting spin-off psychological benefits from feeling more in control of their fate. There is a flip-side to this, however, in that patients who invest a lot of energy and belief in such treatments inevitably feel that they have somehow failed when their disease worsens. This is often painful in itself, but can sometimes drive them to more extreme adherence to a regime in the mistaken belief that, if only they could adhere more perfectly, then improvement would follow. There is a further problem with some dietary approaches like Gerson therapy. Whilst in some ways the diet (at least, without the coffee enemas) could be regarded as healthy, it may be unsuited to some types of cancer patients. For example, patients with pancreatic cancer tend to lose weight rapidly. Following a diet that will tend to bring about weight loss in healthy individuals is thus actively harmful when weight loss is part of the problem being faced. Also, as already noted, many patients tend to ‘mix and match’ the conventional with the alternative. Treatments such as chemotherapy can lead to digestive problems and promote weight loss. It is thus easy to see that a very high-fiber diet, relatively low in calories, may not be ideal in such circumstances. The alternative practitioner would, of course, argue that the problem here is the conventional not the alternative part of the treatment. This would be an acceptable line to run if these treatments were subject to proper scrutiny with proven efficacy. For Gerson therapy, despite 90 years of use, many published case reports, and reviews by academics, there is still not a single published clinical trial. Rather as with drugs, I feel it is for the proponents of such treatments to arrange trials, just as the drug companies have to demonstrate effectiveness to obtain a licence for their products. There may well be patients who do benefit from ‘alternative’ dietary approaches, but at present, the evidence is lacking. Closely linked to alterations in the diet are nutritional supplements based on either vitamins and minerals or herbal mixtures (sometimes called ‘nutriceuticals’). These therapies are potentially more amenable to conventional clinical evaluation than the complete lifestyle change advocated by groups such as the Gerson therapists. The simplest version of dietary supplementation is with either vitamins or minerals. Vitamins (a derivative of the compound words ‘vital amines’) are chemicals present in tiny amounts in foodstuffs and are essential for the body to maintain normal functions. A good example is vitamin C, derived from various fruits, particularly citrus ones. Shortage of vitamin C leads to that scourge of ancient mariners, scurvy, a condition in which wound healing is impaired, tissues become fragile and bruise and bleed easily, gums bleed, and teeth fall out – the body’s so-called ‘connective tissue’ fails to connect things properly. Clearly, therefore, vitamin C is essential for life, but if we have sufficient, is there any benefit in taking more? The Nobel prizewinner Linus Pauling became convinced that there was a benefit in so-called ‘mega-doses’ of the vitamin, and he vigorously advocated the practice for various ailments from the common cold to cancer (it should be noted that he got the Nobel for physics, not medicine). Now here we have a readily testable hypothesis – vitamin C can be put in tablets and assessed like any other medicine. This was duly done in various settings and the answer was a resoundingly negative one – dietary supplementation of vitamin C above normal levels did not help fight cancer (or anything else). Nonetheless, hard evidence of lack of efficacy in no way prevents the alternative practitioners from continuing to promote the use of the agent, as the most cursory of online searches will confirm.
Even doing trials with simpler substances – minerals – turns out to be very difficult. For example, selenium is present in vegetables and is an essential component of tissues, being involved in the maintenance of the integrity of epithelial membranes – the lining cells of the body’s various tubes and glands. It is these cells that give rise to the common cancers, and thus a lack of selenium would seem a potential candidate for a dietary top-up. Further studies demonstrated that populations with lower selenium levels had a higher risk of cancer. This prompted trials of selenium supplementation in patients with cancer, and one famous study in skin cancer showed that the patients receiving the extra selenium had a lower risk of getting second cancer – of the prostate. The problem was, this was not what the trial was studying, but nonetheless, it was sufficient to trigger the mass consumption of selenium by men concerned about their prostates. To confirm the effect, a huge trial called SELECT was set up in the USA looking at two supplements – selenium and vitamin E. After recruiting 30,000 men, who were allocated one or other supplement, both, or neither in a blinded fashion, the trial was stopped by the Data and Safety Monitoring Committee. By this point, the men had been followed for an average of 5 years. The Committee found that not only was there no suggestion of any benefit from either agent but, more troublingly, there was the possibility that there was a slight increase in the risk of prostate cancer with selenium and, unexpectedly, the possibility of an increased risk of diabetes with vitamin E.
Even this is not necessarily the last word on the topic, however. In North America, dietary selenium levels are relatively high, hence extra may not be as useful as it would be in Europe where dietary selenium levels are lower (the difference relates to selenium levels in the soil in which vegetables are grown). In addition, selenium can be supplied as a pure chemical form or as what is known as a ‘complex’ linked to organic compounds more akin to the form obtained from food. Thus all we really know for sure is that the precise form of tablet used in the SELECT trial does not prevent prostate cancer in North American men. Other trials are still ongoing with both agents – for example, our own group is studying both selenium and vitamin E in men and women with early bladder cancer (also linked to lack of both in the diet) to see if supplements can prevent recurrence of cancer. My own opinion is that in most cases in the developed world, the levels of most vitamins and minerals will be adequately provided by most diets, particularly given the growing tendency to over-consume calories. Any effect from supplements in this setting is likely to be small, as most diets will already contain an excess over what is really needed. This is why definitive trial proof has been so difficult to obtain. As with many things in life, what starts out looking quite simple gets more complex the closer you look at it. This uncertainty, of course, fuels the market in supplements – what could be safer than taking extra ‘natural’ vitamins and minerals? If the men in white coats (though, of course, mostly we don’t wear them any more) are not sure, why not take them just in case? What about herbal remedies? These are, of course, attractive in the sense of being somehow more ‘natural’ than harsh, chemically produced pharmaceutical products. The logic is, however, intrinsically flawed – there is nothing inherently ‘nice’ about the natural world – watch any wildlife television show for confirmation of this. The word really has no meaning in this setting – context is everything. For example, botulism is a highly unpleasant, sometimes lethal, gut infection, but botulinum toxin is used to make people look more ‘beautiful’ and is certainly relatively safe as a medicinal product. The medicinal product is therefore much safer than its ‘natural’ source. If a herbal remedy works, it is of course because it is a drug (or more precisely, a mixture of many drugs, with varying activities and side effects).
There is also nothing magic about it being ancient (as if the length of use somehow confers an aura to it). Good examples of long-used natural remedies include witch hazel (which contains abundant salicylic acid, better known as aspirin), the opium poppy (the source of morphine and diamorphine), and foxgloves. Foxgloves are a good example of an ancient source of drugs. A brew known as ‘Shropshire tea’ made from foxglove leaves was used for centuries to treat the ailment known as ‘dropsy’- accumulation of fluid in the lower limbs, accompanied by shortness of breath, now known to be heart failure. Then 20th-century science isolated the active ingredients – a family of chemicals named after the plant – digitalis alkaloids, of which the most commonly used is called digoxin. These drugs still form a major component of the treatment of heart failure. As far as I am aware, though, no one still uses Shropshire tea in place of digoxin.
So what about herbal cancer drugs? Well, firstly, many cancer chemotherapy drugs are indeed herbal extracts – vincristine, used to treat blood and lymphatic cancers is derived from the periwinkle plant. The taxanes, used for many cancers including breast, prostate, and lung, are derived from the yew tree bark and leaves, and so on. Hence the study of the properties of herbs has been a major and fruitful source of some of our most potent drugs. Again, the natural source of these drugs would not make a good herbal medicine – for example, eating yew leaves is both difficult (they are very tough) and potentially fatal – the window between useful treatment effect and lethality is small. There are examples of herbal medicines that have been tested in studies. One that I am particularly interested in is the mixture initially called PC-SPES (which stands for Prostate Cancer-spas, of ‘hope’ in Latin). This was allegedly produced from an ‘ancient’ Chinese herbal remedy, and marketed for ‘prostate health’. Around 20 years ago, it was apparent that patients in mainline prostate cancer trials who happened also to be taking PC-SPES were deriving benefit from the herbal remedy. Despite its name, it was never tested by its makers as a cancer therapy but was licensed as a food supplement. Subsequent laboratory investigation confirmed that PC-SPES behaved like an oestrogen – technically, a photo- (meaning plant) oestrogen. It will be recalled that oestrogens are widely used in prostate cancer therapy, and thus it is entirely plausible that PC-SPES would have anti prostate-cancer effects.
Detailed study of patients taking the mix demonstrated effects on male hormone levels and the prostate cancer marker PSA consistent with a hormonal basis for action. The clinical and chemical analyses were published in the New England Journal of Medicine, probably the world’s premier medical journal.
This publication prompted the setting up of a trial comparing PC-SPES with a real oestrogen called stilboestrol in patients with advanced prostate cancer. The trial commenced but was stopped early due to minute levels of contamination of PC-SPES with stilboestrol. Botanic Laboratories, the manufacturers, were then shut down by the regulatory authorities in the USA, ending any possibility of completing the study. There are puzzling aspects to this story. PC-SPES had been made for years with no adverse inspections, and analysis in the original New England Journal article had found no contamination with stilboestrol. Furthermore, the trial, in so far as it was completed, suggested that PC-SPES was superior to stilboestrol, a result incompatible with the clinical effects being due to stilboestrol contamination, as has been suggested by some commentators.
The problem with agents such as PC-SPES is that they are only licensed as foodstuffs and hence not subject to the sorts of evaluations that a drug will have to go through. Also, the preparation is a mixture of herbal extracts, raising the question of how many components of the mix are actually required for the undoubted clinical effects seen (which included some of the known adverse effects of oestrogens such as deep vein thrombosis). The example of Shropshire tea and digoxin illustrates the potential route of development. Unravelling this would, of course, take many years and many healthcare dollars, possibly with no patent protection to allow the company to fund these costs. We will probably therefore never know what the real active ingredients are in PC-SPES. Furthermore, although the agent looked to have clinical value, it is no longer available, though a number of similar agents (called by various names, including, in a direct reference to PC-SPES, PC-HOPE) have appeared on the market and are widely used by patients. Whether these PC-SPES clones are really the same as the original, again, we will never know. With patients taking these largely unsupervised, there is no consistent body of literature on dosing, adverse effects, and so on. In addition, as these are mixtures of herbs, even if the components by weight are the same, there is no guarantee that the actual active components will be the same in consecutive batches – anyone who has a garden will know the variation seen from year to year in the plants they grow in the same bit of ground. It is hard to see any coherent way forward given the nature of herbal remedies and the current licensing environment. Companies are unlikely to queue up to carry out trials in the future of their herbal remedies given what happened to Botanic Labs with PC-SPES. Equally, the costs of turning a herbal mix into a regular drug with potentially no patent protection seem prohibitive. The pharmaceutical industry will, of course, continue to screen herbs for useful drug properties, but the subsequent development will be aimed at a single chemical entity, not a herbal brew. I suspect that these agents will be forever in a shadowy hinterland between conventional medicine and alternative practitioners. This is unfortunate, as mixed in with the large numbers of ineffective therapies such as mistletoe extracts, there will undoubtedly be agents with potentially valuable activity such as PC-SPES. In conclusion, complementary and alternative medicines form a large and economically important activity in the health economy. However, direct evidence of benefit for most such therapies is hard to find. Furthermore, in some cases, there is good evidence of lack of benefit. Despite this, a large proportion of cancer patients use these treatments as adjuncts to (or in some cases, in place of) their conventional therapies. Alongside these quasi-medical interventions, there is a further arena of altered diets, supplements, and herbal remedies, again largely with little or no evidence base. Understanding usage of these treatments is important as they may confound the results of trials in cancer therapy and also may interfere with outcomes from conventional therapy, either for better (rarely, probably) or for worse.