VIDEO
Carotid Artery Occlusive Disease
(Doctor only)
Acute Carotid Occlusion
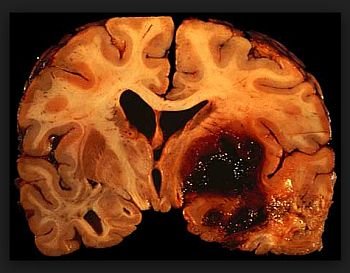
Carotid occlusion can cause a stroke by two mechanisms: Hemodynamic reduction of flow or embolism into the downstream cerebral circulation.
These two mechanisms can often be distinguished by the appearance of the stroke on MRI, and by perfusion studies. Hemodynamic strokes will have a ‘‘watershed’’ distribution of infarction and reduced flow in the distal beds of the MCA, ACA, and PCA, while emboli will have a classical embolic distribution of infarction and reduced flow in the branches of these vessels.
. Carotid occlusion patients are at high risk for recurrent stroke by either mechanism.
. In general, patients with carotid occlusion are managed conservatively with risk factor reduction, careful maintenance of cerebral perfusion by cautious blood pressure control, and antiplatelet drugs. Aggressive intervention with anticoagulants or revascularization is mainly reserved for patients with small areas of infarction who are having continued symptoms and are at perceived risk of deterioration or recurrence.
. One traditional approach is to anticoagulate acutely and for several months after acute symptomatic carotid occlusion to prevent distal emboli. The thinking has been that the end of the occlusion intracranially has an unstable clot that can propagate or embolize.
However, there are no conclusive data supporting anticoagulation and substantial variability exists among stroke experts on this issue, so the decision is usually individualized from patient to patient.
. Carotid occlusion can also be revascularized surgically (by CEA) or endovascularly (by intra-arterial lysis with or without stenting). The clot is usually at the internal carotid origin; andthe rest of the artery downstream might be open. Though acute revascularization has been advocated by some, there are no prospective data to support the theory that acute revascularization (1) improves the patient’s symptoms from current stroke or (2) prevents recurrent stroke long-term.
There are substantial risks to acute revascularization and such patients must be selected very carefully.
. In the
. If bypass is considered, there are several measurement methods for risk stratification by hemodynamic reserve:
– Xenon-CT or single photon emission CT (SPECT) with acetazolamide (Diamox) challenge.
– PET with oxygen extraction fraction.
– TCD with breath-holding index (BHI).
. Normal BHI0.69> – <10% ipsilateral stroke in 2 years.
. Impaired BHI<0.69 – 40% ipsilateral stroke in 2 years.