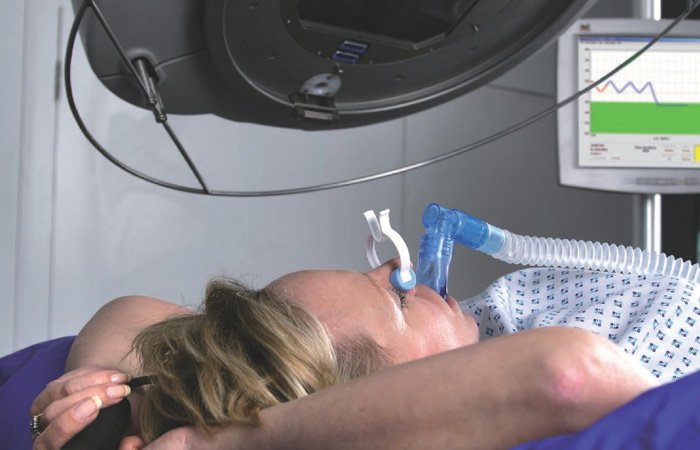
What Is a CAT/CT Scan Machine?
I’ve heard the term “multidisciplinary care,” or “tumor board,” used. What is this and should I be requesting this?
A key advantage to having a multidisciplinary team approach is the special expertise each health care professional offers to each patient’s unique situation. Centers that hold weekly breast cancer case conferences (sometimes referred to as breast cancer tumor boards) to discuss in detail a patient’s clinical condition, diagnostic findings, and recommendations for optimal treatment find that these meetings are beneficial to the patient’s overall wellbeing and clinical outcome.
Since your case will be discussed in light of the most up-to-date research findings, this is a way that you can ensure that you are being given individualized attention and care by a team of experts. All accredited cancer centers are required to conduct such conferences on a regular basis and maintain records of the cases presented. Usually the patient is informed by the physician presenting her case that her clinical situation is going to be discussed by the team.
The doctor then informs the patient of the discussion and outcome of that presentation, including clinical research trials that you may choose to participate in. Ask your doctor if she
is part of a multidisciplinary team and if your case will be presented at their tumor board meeting.
Why would I be participating in a clinical trial now? I thought that they were just for women with breast cancer that hadn’t spread?
Having as many treatment options available to you as possible can be valuable. Breast centers who participate in clinical trials can usually offer more innovative treatment options. Many clinical trials offer you treatment that is at least as good as the standard of care and, possibly, better. If you are asked to participate in such a trial, you are also paving the way for the development of innovative research that will make an important impact on other women diagnosed in the future. You will be closely monitored throughout the treatment process so that data can be collected about your experience with the chemotherapy agents you’ve been given.
My surgery was done when I was originally diagnosed with breast cancer. Will I still need a breast surgeon to be involved now?
You have probably already had breast cancer surgery done when you were originally diagnosed with breast cancer. There are situations, however, that result in needing additional surgery when breast cancer returns. This can be for local control of the disease, diagnostic purposes, or to relieve pain. It is preferable that the surgeon is a surgical oncologist who specializes in breast cancer.
Such surgeons are often found at a large teaching hospital that is part of a cancer center. There may also be a need for some patients to have a plastic surgeon who specializes in breast reconstruction.
How do I select the medical oncologist who will primarily be responsible for my care and treatments?
You will feel more confident being treated by a medical oncologist who specializes in breast cancer. You will want someone who treats a large volume of women with this disease and has access to a spectrum of clinical trials for you to consider. Be sure to also ask how the physician’s office practice handles emergency issues, such as a sudden high fever or uncontrolled nausea and vomiting.
You will also want to know who will cover for your doctor on weekends or when he or she is on vacation. This doctor should also be a medical oncologist. These are important factors to ask about so that you are confident your case is being well managed. Ask what education is available to help you prepare for known side effects of treatment. Inquire how patients are referred for wig fittings, as well as any skin care needs that may occur during treatment. Some breast centers offer these services within their facility.
Do I need a radiation oncologist?
Most patients who are having breast conservation surgery or have had locally advanced disease have already undergone radiation therapy in some manner. It is valuable to go to a facility that has extensive experience as well as doctors and therapists who specialize in treating this specific type of cancer. They will have a radiation physicist on staff who assists with the treatment planning. There are different methods of delivering radiation for breast cancer treatment today. Some are part of clinical trials and some are standard of care. Patients will want to know how their heart and lungs will be protected from the radiation field. Today, a device called Active Breath Control Device is available at some centers, which, by controlling her breathing during the actual radiation treatment, provides a more reliable way for the patient’s heart and lungs to be spared radiation. At some point during your treatment for metastatic disease, you may need radiation therapy to help shrink the tumor(s), provide local control of the disease, or reduce pain symptoms.
I want to make sure that my doctors are communicating with one another and not relying on me to give them updates. How do I make sure my medical oncologist, radiation oncologist, and family doctor are talking?
You need to have confidence that you are being watched over and cared for appropriately. Some facilities have nurse practitioners who stay in touch with the patients via telephone once they are home from surgery and/or chemotherapy. More are beginning to offer patient navigators to help with coordination of care. The team of professionals taking care of you also needs to stay in close contact with one another. Tumor board conferences are another way that your team stays in touch. Ask them how they communicate and keep each other informed about your condition and needs. You want to know that you are being cared for by a team who stays well connected with you and with each other. Feeling confident that you are receiving good continuity of care provides wonderful peace of mind to you and your family.
Who do I call when I have an emergency or urgent problem?
When an urgent medical problem arises, such as vomiting that won’t subside, a clear process needs to be in place for patient management. Ask what the doctor’s procedures are for handling such emergencies. A breast center needs to have available a professional health care provider 24 hours a day, 7 days a week to handle emergencies. In addition to this, the patients should know how to access this service and know they can confidently rely on it. Though it is hoped that you will not need such services, it’s important they are in place and can be readily accessed.
The stress of thinking about what may lie ahead is overwhelming to me. Who can help me with these feelings?
You need to be treated as a total person. You are not only a stage IV breast cancer patient. You may be a schoolteacher, recently divorced, with two young children and a mother who has chronic illnesses and lives with you. Breast centers usually provide social work counseling, psychotherapy services, and nurses along with others to help you along this journey. Some offer to match a breast cancer patient with a survivor volunteer based on her age, stage of disease, and anticipated treatment plan, including those with metastatic disease. This isn’t always possible but when it is, it provides a unique level of support for someone just embarking on chronic treatment. Patients usually value the opportunity to talk with others. Some breast centers also offer special support groups for women dealing with metastatic disease.
Breast centers who participate in clinical trials can usually offer more innovative treatment options.
You want to know that you are being cared for by a team who stays well connected with you and with each other.
Terms:
Standard of care – A diagnostic and treatment process that a clinician should follow for a certain type of patient, illness, or clinical circumstances.
Radiation physicist – Makes sure that the equipment is working properly and that the machines deliver the right dose of radiation
Active Breath Control Device – A special device used during radiation therapy to help protect the heart and lungs from radiation when the left breast/chest wall is receiving radiation. Currently part of a clinical trial.
Patient navigators – An individual who assists patients in navigating their care and treatment by assisting them with scheduling appointments, answering questions related to test results, and providing guidance in decision making across the continuum of care.