Tackling medication overuse headache
Medication overuse headache (MOH) is challenging to treat because, first and foremost, it is about stopping taking the painkillers. Doing this successfully means finding the strategy relevant to you, as an individual; what works for one person may not necessarily work for another.
In most instances you will need to rely on the help and support of your doctor or practice nurse throughout this process, as headache clinics and specialist nurses are not a readily accessible resource. As you read through this chapter you may have to substitute the word ‘nurse’ with whoever you are using as your support person; realistically that could be anyone, although you will need the assistance of a doctor if you need prescribed medication or a sick note.
MOH is where an occasional headache becomes a daily or near daily headache. It is a headache associated with the uncritical use of painkillers, increasingly frequent use of painkillers, and the use of stronger and stronger painkillers to treat headache symptoms.
Research has shown that 71% of people with MOH started with migraine alone, 14% started with tension-type headache alone and 15% had a mixed picture headache of migraine and tension-type headache.
STOPPING THE PAINKILLERS – THE FIRST STEP BACK TO EPISODIC HEADACHE
My doctor has told me about medication overuse headache and how to stop it but I just cannot imagine getting through the day without any painkillers. How am I going to cope?
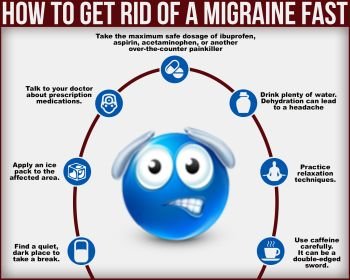
Coping is about getting back in control of your headache symptoms. It means swapping your daily headache for a headache that occurs every now and again. Coping is about changing what you do in response to your headache. It is about putting strategies or ‘cushions’ in place to help you manage your headache without taking a painkiller. The cushions you need will be unique to you and how you cope will be unique to you. There is always a way – you just have to find out what it is. There is no right or wrong way – what this text does is offer you ideas and make suggestions.
The specialist has said I need to stop taking my painkillers but how can I do it?
You need to find your own way. You can either stop all of your painkillers immediately or gradually reduce them to the point where you stop using them. The best way is the way that will work for you. If you are taking strong painkillers, especially if they contain codeine and caffeine, it is probably better to stop them by gradually reducing the number you take to try to minimize the ‘rebound’ withdrawal symptoms you might experience. (See also the next answer.) I am in the process of trying to stop taking my painkillers.
The specialist nurse kept talking about withdrawal symptoms – what does she mean?
When you stop taking your painkillers you can expect to experience symptoms that occur as a direct consequence. This ‘rebound’ effect is inevitable: the type and severity of these symptoms are unpredictable and vary from person to person and from headache to headache. If your primary headache is migraine, many of your rebound symptoms will be similar to those of your migraine – including headache, nausea, vomiting, light sensitivity, mood swings, irritability, and sleep disturbance. If your primary headache is tension type headache (TTH), your symptoms will resemble those of TTH, including worsening headache, irritability and sleep disturbance.
I am worried because I use co-codamol for my headache. I only take two a day, but I have to take them every day. Will that make it harder to stop?
The only answer I can offer is that it might. Codeine is an addictive drug. Co-codamol comes in a dose of 8 mg or 30 mg of codeine mixed with 500 mg of paracetamol. The higher the strength of cocodamol you take, the harder it might be to stop. The more you take each day the harder it might be to stop. Many over-the-counter painkillers contain some codeine as well, so you need to check just how much codeine you are actually taking.
I take co-codamol and have been told that the best way to stop, because of the codeine, is to gradually reduce the tablets. Why is this so?
Stopping codeine causes side effects, and in someone with medication overdose headache stopping painkillers abruptly may lead to ‘rebound’ symptoms. Stopping painkillers when you have medication overuse headache is always difficult, and success often depends on minimising the effect of withdrawal. Codeine is an addictive drug, and reducing the dose of co-codamol gradually also reduces the sort of side effects you might experience in stopping the codeine.
I have been taking co-codamol, up to eight a day, but not necessarily every day. The specialist nurse has suggested that I gradually reduce the dose of codeine, but how gradually is gradually?
How quickly or slowly you reduce your tablets depends on exactly how many you take and what strength the codeine is. If you are taking 30-mg-strength tablets, especially if you are taking two tablets each time, I suggest that you take an 8 mg instead of one of the 30 mg tablets. This way you gradually reduce the amount of codeine you take each time, and then you can gradually reduce the total number of doses each day.
It can be difficult to know over how many days you make this dose reduction – it will often be decided according to the sort of symptoms you experience. Only you can make that decision, and your specialist nurse can help you as you do so.
My friend takes Syndol for her headaches, and she has suggested that as they help her a little I should try them for my headaches. Is that a good idea?
If you have frequent headaches, or have MOH, swapping one painkiller for another is not really a good idea. Any painkiller, including Syndol, Solpadeine (both with paracetamol) or Nurofen (ibuprofen), has the ability to lead to MOH if taken on more than three or four days in the week, and therefore should be used only infrequently to treat headache.
If the headache is going to get worse when I stop the painkillers, what can I do for the headache? I have to be able to get through the day somehow.
The only way to break the MOH cycle is to take no painkillers at all for at least six to eight weeks. If you take any painkillers at all during this ‘washout’ phase, it may make it less likely that the headaches will improve.
Not taking painkillers when the headache gets bad is not easy. You may need to think about taking time off work (your doctor should be able to help with a sick note) or you may need to think about other medication used to treat chronic pain, which could help reduce the headache you experience. By taking something else, a preventative drug every day, you may be able to ease or stop or headache and avoid the need for painkillers. This will make it easier for you to successfully stop the painkillers and allow your headache to become episodic and infrequent again.
I know that my headaches may well get worse when I stop my painkillers. What else can I expect?
It is always difficult to know what will happen, because everyone is different. The possible symptoms include nausea and sometimes vomiting, sensitivity to light, feeling bad-tempered and irritable, getting mood swings, and having difficulty sleeping. It is unlikely that you will experience all of these but you could experience any one of them at some time during your ‘washout’.
The clinic has said that I can’t take any painkillers for at least six weeks. That seems an awfully long time. Do I really have to wait that long?
Medication overuse headache is always difficult to treat. Success can be achieved only if you take no painkillers at all. The longer you can avoid taking painkillers, the more likely that your headache will improve. Your specialist has suggested six weeks as the starting point but will probably encourage you to carry on for another week or two so that your total washout is for eight weeks, and perhaps even longer. It depends on how quickly your headache improves. If your headache is slow to respond, prolonging the washout is the best way to go. Some people find that they notice a dramatic improvement in a week or two whereas others may need as long as ten or twelve weeks; everyone is different and there is no real way of predicting how quickly or slowly things will change.
It is not easy but tries hard to stick to it, because it is the only way. Remember to ask all your friends and family to help; that way you are more likely to succeed.