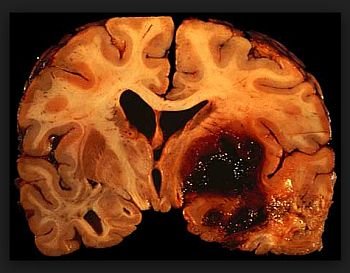
Transient ischemic attack (TIA)
(Doctor only)
Clinical approach to a patient with suspected TIA
Evaluation of TIA is the same as for ischemic stroke, since the pathophysiology of TIA and ischemic stroke are the same. TIA should be thought of as a briefer, smaller ischemic stroke, but with the same implications for recurrence.
History and Physical Exam
Make sure that the neurologic symptoms have resolved!
If you document a normal neurological exam and later the patient develops recurrent neurological deficits, they can still be treated with TPA because the clock starts over from the time of new symptoms, as long as the patient was completely back to normal in between.
Since you are likely to be seeing the patient after, and not during, the TIA, get an objective description as much as possible, perhaps from a witness:
‘‘Were you able to move your arm?’’
‘‘Was his speech slurred?’’
‘‘Was she able to walk normally?
Brain Imaging
Consider skipping CT and going straight to MRI and MRA if possible.
CT is expected to be normal because
. It was transient ischemia;
or
. Ischemia continues to be present but it’s too small to see on CT;
or
. It was not ischemia.
MRI is more likely than CT to be helpful because
. It shows you a small stroke that you didn’t see on CT (ischemia improved to make the patient symptomatically back to baseline but tissue was damaged);
or
. It shows you a vascular lesion that, by association, makes you suspect that it was an ischemic event (small vessel disease, old stroke, arterial stenosis, etc.);
or
. It shows you some other explanation of the transient event (subdural hematoma, tumor, etc.).
Decide whether this is more likely a Tia or smothingelse
Other tests might be done to exclude non-TIA diagnoses if they are suspected.
Electrocardiogram (EKG) is helpful because
. If you see atrial fibrillation, it was likely to have been a cardioembolic TIA. In these cases, initiating treatment with anticoagulation may prevent a stroke.
Measurement of blood sugar is helpful because
Hypoglycemia can explain the event.
Measurement of other electrolytes is helpful because
Electrolyte abnormalities may also explain the event.
The risk of stroke after TIA: the Diabetes, Duration, Weakness (DDW) score
Three risk factors for stroke after TIA (Give 1 point each if present) – Number of risk factors present – Estimated risk of stroke in 7 days
Diabetes mellitus – 0 – 1%
Duration of episode – > =60 minutes – 1 4%
Weakness (focal) with episode – 2 – 9%
– 3 – 10%
Notes:
(1) These are risk factors that make ischemic etiology more likely.
(2) This prognostication score has not been prospectively validated in an independent dataset.
Adapted from: S. C. Johnston & S. Sidney, Validation of a 4-point prediction rule to stratify short-term stroke risk after TIA. Stroke 2005; 36: 430.77 Reproduced with permission from Lippincott Williams & Wilkins.
Management
Again, the management is similar to that for acute ischemic stroke, as are the preventive measures.
Observe the patient for 24 hours. Remember, if they develop new neurological symptoms they could be candidates for TPA if no other exclusions exist.
Start daily antiplatelets.
MRI to evaluate for new and old stroke.
Carotid ultrasound and TCD, MRA of neck and brain, or CT angiogram of neck and brain to look for arterial stenosis. Be sure to evaluate the entire cerebrovascular system.
EKG, and consider EKG telemetry.
Cardiovascular risk-factor evaluation of blood pressure, lipids, and fasting glucose
Consider echocardiogram for evaluation of cardioembolic source.
Educate the patient about:
Stroke risk factors including smoking, exercise, weight loss, alcohol;
Specific medications prescribed for prevention;
Recurrent symptoms to look for; and
Calling emergency services for acute stroke symptoms.
Discharge with established follow-up plans.
Prognosis after TIA
After an ED visit for TIA:
5.3% stroke risk within 2 days;
0.5% stroke in 90 days (21% fatal, 64% disabling).
1 in 9 patients will have a stroke within 3 months.
The key problem is trying to predict who will have a stroke