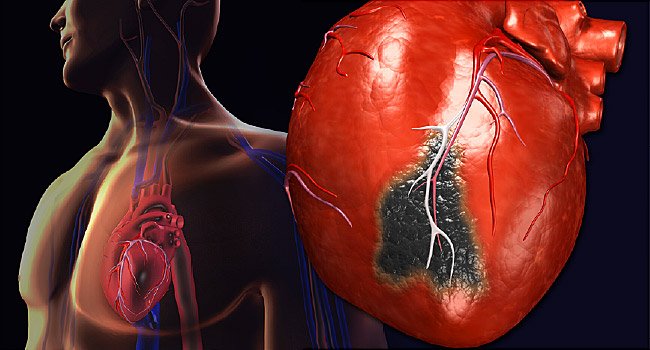
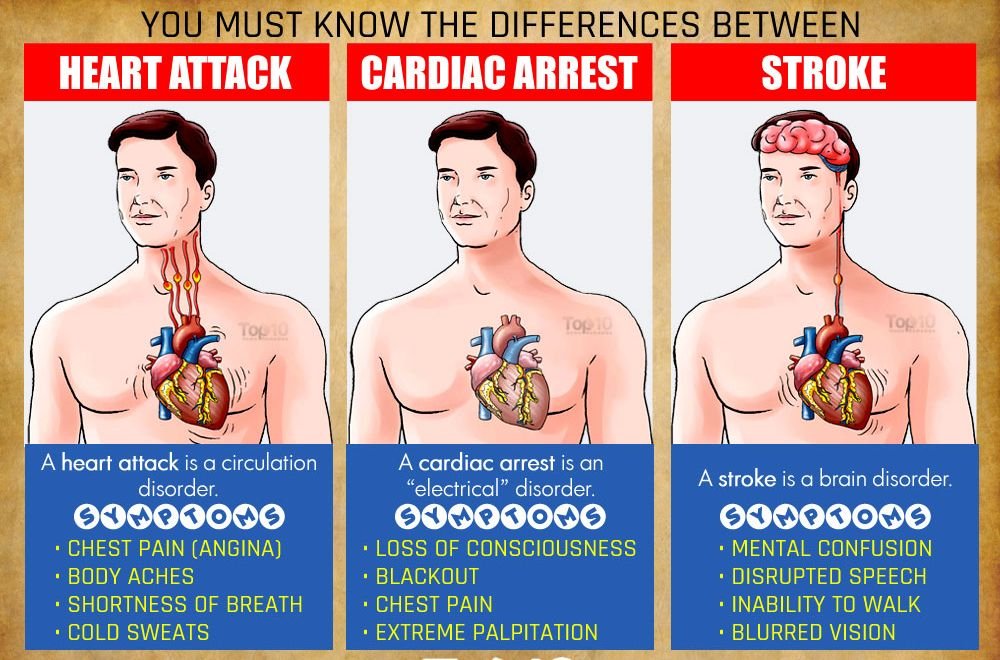
3D Medical Animation – What is a Heart Attack?
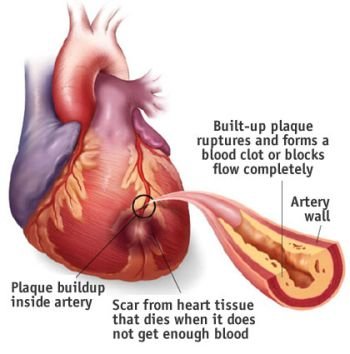
What is a nuclear scan, and what is its diagnostic value?
An echocardiogram uses sound waves to produce an image of your heart. An echocardiogram machine directs sound waves at your heart through a wand-like device (called a transducer) held against your chest. The sound waves bounce off your heart, reflect back through the chest wall, and proceeded electronically to produce video images of your heart on a monitor screen. An echocardiogram can identify an area of your heart muscle that’s been damaged by a heart attack and can show the status of your heart’s pumping action.
What is a coronary angiogram, and what is its diagnostic value?
A coronary angiogram (arteriogram) is the definitive and most accurate diagnostic test for coronary artery disease. A coronary angiogram can precisely identify specific sites and degree of a narrowing (stenosis) or blockage of your coronary arteries. Therefore, a coronary angiogram is essential before any attempt to perform a coronary artery dilatation by coronary angioplasty (PTCA) or a coronary artery bypass surgery.
In a coronary angiogram, a doctor inserts a catheter (a long thin tube) into an artery in your groin area (or, less commonly, in your arm) and threads it through that artery to your heart arteries. Then the doctor injects a liquid dye into your coronary arteries by way of the catheter. As the dye (called contrast agent) flows through those coronary arteries, the doctor can accurately identify any narrowing (stenosis) and blockage of those arteries using a series of x rays and videotapes.
Are other tests available?
Several other tests are available for the diagnosis and treatment of coronary artery disease either directly or indirectly. The chest x ray can evaluate the condition of your lungs and the size and shape of your heart and major blood vessels. A chest x ray is particularly useful also for monitoring the management of various complications from a heart attack.
Electron beam computerized tomography (EBCT), also called an ultrafast CT scan, and scans your coronary arteries for signs of calcium within plaques that can cause coronary artery narrowing or blockage. When it detects a substantial amount of calcium, it almost certainly points to a diagnosis of coronary artery disease, because plaques contain some calcium in the majority of cases.
Magnetic resonance imaging (MRI) with enhanced software can provide accurate information about arterial blood flow, including that in very small coronary arteries not visible when using a coronary angiogram.
Terms:
Coronary angiogram (arteriogram) – x-ray study in which dye is used to demonstrate the degree and the location of coronary artery narrowing or blockage.
Electron beam computerized tomography (EBCT) – a new diagnostic test to detect calcium within plaques of coronary artery
Magnetic resonance imaging (MRI) – a form of special diagnostic x-ray tests that can be used to diagnose coronary artery narrowing or blockage.
What is ventricular wall rupture?
Ventricular wall rupture (rupture of the heart muscle of the ventricles) is the most serious and life-threatening complication of a heart attack. This is because the disorder causes rupture of the pumping chambers of the heart. As soon as the ventricles rupture, there will be no heart function at all, and sudden cardiac death is the immediate outcome. For nearly every patient who experiences ventricular wall rupture, there is no possible treatment.
What is congestive heart failure and what are its usual symptoms?
The heart muscle damage from a heart attack may be so extensive that the remaining heart muscle is unable to provide adequate pumping action. Consequently, blood flow to tissues and organs throughout the body (including the heart itself) markedly decreases, leading to congestion in the lungs and to a variety of symptoms and signs. This event is termed congestive heart failure (CHF) or simply heart failure.
CHF displays various signs and symptoms. Shortness of breath (dyspnea), especially during physical exertion or upon lying down; fatigue and weakness; and edema (swelling) of the legs, ankles, and feet are symptoms characteristic of CHF. It also can lead to wheezing or coughing up white or pink blood-tinged phlegm (sputum); swelling of the abdomen and rapid weight gain from fluid retention; and engorged neck veins. Those experiencing CHF would have dizzy or fainting spells (syncope) and palpitations from abnormal heart rhythms (cardiac arrhythmias). Nausea and loss of appetite would also be evident. CHF can even cause diminished alertness and difficulty in concentrating.
What is cardiogenic shock?
Cardiogenic shock occurs after insufficient blood circulation to your body, including the heart muscle itself. It’s the result of low and ineffective blood pressure (BP) brought on by a markedly diminished pumping action of the heart during or immediately after a heart attack. In cardiogenic shock, coronary arteries do not receive sufficient blood, so the heart becomes weaker, and the blood circulation further decreases. Unfortunately, this vicious cycle is fatal in most cases. In 7 to 15% of cases, cardiogenic shock often occurs during the first few days after an acute heart attack.
Cardiogenic shock tends to occur when 40% or more of the left ventricle is damaged by a heart attack, and advanced disease is often found in three major coronary arteries. Usually, cardiogenic shock is associated with advanced CHF in heart attack victims. (The scope of this book prevents discussion of the management of cardiogenic shock.)
What are cardiac arrhythmias and how should they be handled?
Various abnormal heart rhythms, known as cardiac arrhythmias, frequently occur after a heart attack damages the heart muscle. Abnormal heart rhythms may be benign (i.e., not harmful) and self-limited, but serious arrhythmias often lead to sudden death. Abnormal heart rhythms may be slow (called bradycardia or bradyarrhythmia), fast (called tachycardia or tachyarrthymia), or irregular. In most cases, if you were affected by this disorder you would need an artificial cardiac pacemaker, an electrical device that activates the heart with batteries, for a persisting slow heart rhythm. For rapid heart rhythms, on the other hand, your doctor could prescribe any of several medications (e.g., beta blockers, calcium channel blockers, lidocaine, procainamide, amiodarone, and the like). To handle life-threatening rapid arrhythmia (ventricular fibrillation), your doctor would immediately apply electric shock, the only life-saving measure.
Cardiac arrhythmia (also called cardiac dysrhythmia) may appear as too fast, too slow, or irregular heartbeats. Certain stimulants, such as stress, tobacco smoking, caffeine, and alcohol, can cause you to experience a variety of cardiac arrhythmias, even if you’re apparently healthy. Under those circumstances, you wouldn’t need any particular treatment other than eliminating or controlling the abovementioned stimulants. However, more than 4 million Americans suffer from recurrent or symptomatic arrhythmias that usually require treatment. Clinically, significant arrhythmias usually occur in older adults with coronary artery disease when the electrical system of the heart is disturbed. Serious arrhythmias commonly are by-products of coronary artery disease damage to the heart, particularly that resulting from a heart attack. Life-threatening arrhythmia, particularly ventricular fibrillation, must be terminated within a few minutes to prevent sudden death, especially in patients experiencing an acute heart attack.
Terms:
Heart failure – inability of the heart to pump adequately; also called congestive heart failure.
Dyspnea – shortness of breath.
Edema – fluid accumulation resulting in swelling, commonly due to heart failure.
Cardiogenic shock – life-threatening complication of a heart attack, common signs of which include hypotension, clammy skin, unclear mental state, markedly reduced urine output, and very poor pumping action of the heart.
Cardiac arrhythmia – abnormal (slow, rapid, or irregular) heart rhythm.
Bradyarrhythmia – abnormally slow heart rhythm (also called bradycardia).
Tachyarrhythmia (or tachycardia) – rapid heart rhythm.
Artificial cardiac pacemaker – electrical device that activates the heart using batteries, used temporarily or implanted permanently.
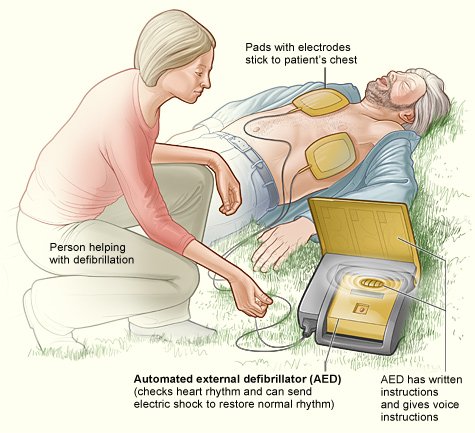
Defibrillation – an electric shock applied to the chest to restore the regular heart rhythm.