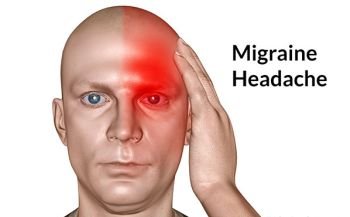
Migraine Pathophysiology (Video)
What is migraine? What causes migraines?
DURING AND AFTER THE MENOPAUSE, AND HRT
Everybody says my migraines will get better when I stop having periods. Are they right?
There is a good chance that your migraines will improve once you reach the menopause and have stopped having any periods. Unfortunately, there is also a chance that they will get worse or even stay the same. There is no way of knowing or predicting what will happen.
I am convinced that my migraines have started to get worse now that I am getting some sweats and flushes. Is this because I am becoming menopausal?
Probably, is the simple answer? Sweats and flushes are common in and around the time of the menopause. Menopausal symptoms are caused by fluctuating hormone levels, and it is quite likely that it is these peaks and troughs in oestrogen levels that lower your threshold so that migraine attacks are triggered more easily.
My gynaecologist has suggested that I have a hysterectomy. I have really bad periods and my migraines are getting worse. Will the hysterectomy help?
A hysterectomy will definitely help the periods but will probably make the migraines worse. Evidence suggests that a natural menopause reduces the chance of having migraine to about 7% whereas having a ‘surgical’ menopause leaves you with a 27% chance of getting migraine if you have no premenstrual syndrome (PMS) symptoms. Not the best of odds, I am afraid. See also the next question and answer.
I used to get bad premenstrual syndrome when I was a teenager and it is getting bad again. The migraines are kicking off as well. My periods are irregular and really heavy. Is hysterectomy the best option?
Premenstrual syndrome (PMS) is not much fun at the best of times and is not easy to treat. It is often associated with migraine-type headaches and migraine can also occur more closely associated with the period. Regulating the period cycle is a good idea, as it may make it easier to control the PMS. Hysterectomy is not the best of options: the evidence suggests that a ‘surgical’ menopause with a history of PMS gives you a 44% chance of getting migraine afterwards compared with 7% without an operation.
I stopped having periods last year. I have never had an aura in my life but last month I became aware of short episodes of flashing lights, just like forked lightning. They last 15 to 20 minutes each time but I don’t always get a headache. Should I be worried?
It is not uncommon to experience aura in the absence of headache and is a recognised entity. If you have never ever had aura, it is a good idea to see your doctor so that a full assessment can be made to ruleout any other possible cause for the aura developing. It is a good idea to check your blood pressure, cholesterol and other similar risk factors for stroke. It may even be necessary to have a brain scan to be absolutely certain that the aura is just migrainous. That decision is best made by a specialist.
My migraines seem to have got worse as my periods have got more irregular. The specialist has suggested I see my doctor to discuss HRT but I have read so much about it in magazines that I am not sure what to do. Why is HRT a good idea?
HRT can help some of the people some of the time. There are, of course, a lot of pros and cons, and the decision-making is nowhere near as easy or straightforward as it used to be. HRT is believed to help by keeping your oestrogen levels as even and steady as possible, because it is thought that it is the peaks and troughs in oestrogen levels that may push down your migraine threshold to a point where triggers are more easily able to generate a migraine attack.
I always thought that HRT protected you against stroke, at least that is what my aunt was told when she started HRT ten years ago. My doctor has said that it increases the risk of stroke. What has changed?
Over recent years a lot more research has been completed that has looked at the long-term effects of using HRT. A careful review and analysis of these studies suggests that, on the basis of the best current evidence, the use of HRT increases your chance of ischaemic stroke by 1.29. There is no evidence that it has an effect on haemorrhagic stroke (1.07) or transient ischaemic attack (1.07).
What do these figures mean? If the number is ‘1’, this means that there is no difference. If the number is less than 1, this means that you are less likely to have a problem; if the number is more than 1, you are more likely to have a problem. The bigger the number the greater the risk of an event happening.
My mother and her sister both had breast cancer. My migraines have got much more frequent during the last few months. I am getting sweats and flushes and my periods are all over the place. I have been thinking about going on HRT, but will it make a difference and what are the risks?
If you are getting a lot of menopausal symptoms, tend to get menstrual migraine and want to find a way of regulating your periods, HRT may well help you. If you are under the age of 50, on the basis of current evidence, there is no perceived risk because all you are doing is replacing those hormones that you are not producing consistently. If you are over the age of 50, the current evidence suggests that you can use HRT for up to five years with no significant increase in risk of developing breast cancer.
What you need to think about is your personal risk of developing breast cancer on the basis of your family history. You have quite a strong family history of breast cancer, which will tend to raise your personal risk, or chance, of developing breast cancer. This risk is higher than in someone with no family history of breast cancer. There is an increase in risk of developing breast cancer once you have been on HRT for five years or more. Your personal level of risk, and hence your starting point, is higher; going on HRT does not magnify this risk any further, your line just runs along a little higher.
I have been thinking about starting HRT to try to help my migraines. My doctor has said that I am more likely to get a blood clot in the first year of taking HRT. How likely am I to get a blood clot? Is it worth the risk?
Your second question is quite difficult to answer because you are the one who should decide whether it is worth the risk. You need to try to assess your personal risk of getting a DVT (deep venous thrombosis – blood clot in the leg). Age is also a factor: the older you are, the more likely you are to get a DVT. The statistics are given as [number] per 1,000 women in five years.
There are other times when your risk is increased: when you have been immobile for a prolonged period of time, or anything else that slows your circulation.
I’ve heard of the coil for contraception. What is a Mirena coil?
A Mirena coil is a specific type of coil that has been impregnated with a particular hormone that is released slowly into the womb. It is also referred to as an LNG-IUS, ‘LNG’ standing for levonorgestrel and ‘IUS’ standing for intra-uterine system. Originally developed as a form of contraception, it is now used to treat heavy periods and can also provide the progesterone needed for protection of the womb lining when using oestrogen patches or gel for HRT.
If it is the oestrogen that helps the migraine and I need HRT to help the migraine, why can’t I just take oestrogen?
That way I won’t get periods. The reason you can’t take oestrogen alone, if you have not had a hysterectomy, is that you have to protect the lining of the womb. The lining of the womb – the endometrium – can be over-stimulated when oestrogen is taken on its own and may lead to endometrial cancer.
Five in 1,000 women who are aged between 50 and 64 years of age might expect to develop endometrial cancer if they do not use HRT. Nine in 1,000 women, of the same age, using oestrogen alone for five years might expect to develop endometrial cancer. Obviously, the longer you use oestrogen, the greater the risk. Fifteen in 1,000 women who use oestrogen alone for ten years might expect to develop endometrial cancer.
Using combined HRT is essential, as the numbers then drop dramatically. Fewer than 2 in 1,000 women using combined HRT for ten years might expect to develop endometrial cancer.
I had a hysterectomy several years ago because of fibroids and am thinking about starting HRT to try to help my menopausal symptoms and my migraines. What should I use?
The advantage of having had a hysterectomy is that all you need to think about is oestrogen. Ideally, you should use a patch or gel. If you start at a low dose and gradually increase it, you will minimize the chance of an increase of migraines rather than a hoped-for fall in the number of attacks.
I am using HRT and am trying to decide how long I should take it. It has really helped my migraines but I’ve been reading about HRT and breast cancer. How long can I safely take it?
Answering that question is about trying to understand the figures from research, which looks at population risk, and translating that into your personal risk. If you are over 50, the longer you take HRT, the greater your potential personal risk.
Different organisations present the figures in different ways, and trying to make sense of it all is not easy. If you consider women aged 50 who do not use combined HRT, 32 in every 1,000 would be diagnosed by the age of 65 years.
If you start combined HRT at the age of 50 and take it for five years, there are 6 extra cases of breast cancer, and if you take it for ten years there are 19 extra cases. This translates to 38 in every 1,000 who take combined HRT for five years and 51 in every 1,000 who take combined HRT for ten years.
Only you can decide how long you can safely take HRT. It depends on how you weigh up the risks and benefits of taking HRT. This is a very personal choice and a very individual decision.
I have been on HRT for five years and my migraines have been fantastic. My doctor says I have to stop after five years but can I carry on using it?
If you have been on combined HRT for five years, you need to consider the facts and decide what level of risk you are prepared to accept to achieve the benefit you are experiencing. If you feel that the risk of developing breast cancer and the potential increase in risk of stroke are worth it, you can make an informed decision to continue.
If you are taking oestrogen alone and do not need any progesterone for protection of the womb lining, the increase in risk of breast cancer is minimal. There is only one extra case of breast cancer per 1,000 women after five years’ use, and a further five cases after ten years.
I have been talking to my doctor about HRT after my specialist said I should try it. Tablets, patches or gels: how do I decide?
Patches and gels are going to offer a better option than tablets. It is the peaks and troughs that tend to trigger migraine attacks, and patches and gels will provide a steady blood level. The advantage of patches, when using a ‘matrix’ patch, is that you can cut it into quarters and halves and thereby slowly increase the dose of oestrogen. The slower the increase, the easier it is to get control of the migraine without causing a rebound increase in migraine attacks due to too much oestrogen.
I am still getting periods but they are irregular and some of them can be quite heavy. How can I ease my periods and help my migraine?
One option is the low-dose combined Pill, provided you don’t smoke and don’t get aura. If you get menstrual migraine, you could ‘tri-cycle’ the Pill, which would reduce the number of periods and the number of migraines. This works because if you take the Pill in the normal way, you get thirteen periods a year. If you tri-cycle the Pill, take three packs one after the other; then you will get only five periods a year and therefore, potentially, only five migraines.
Another option would be the LNG-IUS (Mirena) coil, which would potentially stop your periods. If this, in itself, is not enough to help the migraines, you might consider top-up oestrogen to stabilise fluctuating hormone levels.
I last had a period two years ago and I am thinking about starting HRT to try to reduce the number of migraines I am getting. I don’t want to start periods again, though, so what are my options?
If it has been that long since you had a period, you could try a continuous combined HRT (CCHRT). This has reasonable chance of giving you bleed-free HRT. You might get some irregular spotting or bleeding but, if CCHRT suits you, you should get few or no periods.
If you do not settle with an off-the-shelf option of CCHRT (one of the standard prescribable options), it is possible to get a little more creative. There are two progestogen products that can be taken on a daily basis and then you can use top-up oestrogen, but start at a low dose and slowly increase it until you get the balance right.
Every time I start HRT, my migraines get worse. Why is this?
It is probably because you started with too much oestrogen too quickly. The only way to combat this is to start again at a low dose of oestrogen and then slowly increase it. You also need to take progesterone. If you are just starting with menopausal symptoms (being
peri-menopausal), it needs to be given cyclically; that is to say, you will need to take the progesterone for a short part of each cycle – giving you a period on a regular basis. If you are two years beyond the menopause and you are using oral progesterone, it should be taken daily. An alternative would be to use the LNG-IUS coil as the progesterone source.
Oestrogen, in this circumstance, is best delivered by a ‘matrix’ oestrogen patch, which you can cut into quarters and halves. The size of the dose can be manipulated by quartering the patch and increasing the dose by the smallest increment – doing this weekly, fortnightly or monthly. Increasing the dose in this way will allow you to find the amount of oestrogen that will control your migraines and, hopefully, improve any menopausal symptoms you have.
If my migraine gets worse with the tablet HRT, why will patches be better?
The theory is that tablet HRT causes peaks and troughs in oestrogen levels, which might increase the risk of migraines being triggered. Patches will produce a steady level of oestrogen and are therefore less likely to trigger migraines.
My doctor has said that too much oestrogen is as much of a problem as too little, so how can I find the right dose and get the balance right?
Finding the right dose and getting the right balance need time and patience if an off-the-shelf formulation does not suit you. Different types of progesterone suit different people, and the dose of oestrogen needs to be just right. This means that you and your doctor need to ring the changes and permutations until you get it right.