Sun Safety – Spotting skin cancer
What is skin cancer?
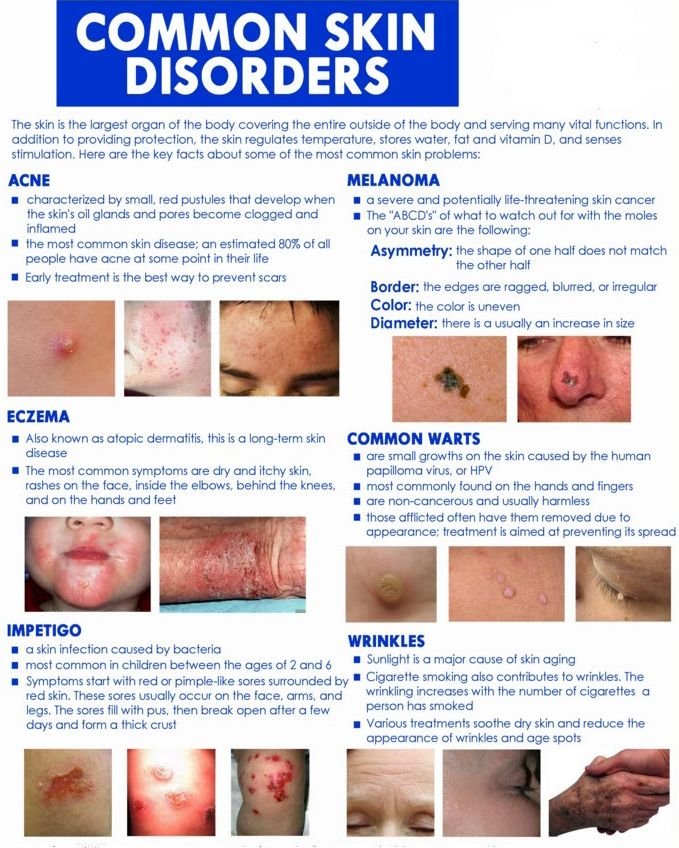
Three basic types of skin cancer exist. The most common but least likely to spread is basal cell cancer. One third of all basal cells occur around the nose. Other common areas are on and around the ears, upper back, neck, and cheeks. Squamous cell cancers (Plate 10) are more likely to spread, and like basal cells, they are generally a result of chronic sun exposure.
Melanomas (Plate 11) are the deadliest cancer. When it has grown to the size of a dime, it already has a 50% chance of having spread. The rate of melanoma in the 1930s was 1 in 1,500, and the rate is now as high as 1 in 75 persons. The four classic warning signs are moles with asymmetrical shape, irregular border, color variation, and a diameter greater than that of a pencil eraser (Plate 12).
Term:
Melanomas – A type of malignant tumor that arises from the uncontrolled growth of melanocytes found in the epidermis.
What about melanoma?
Melanoma is a form of skin cancer that begins in melanocytes (the cells that make the pigment melanin). Although most people have between 10 and 40 benign moles, the melanoma is a different entity.
I remember a patient named Ted, a stock trader, who had a biopsy on his back. When he returned for removal of the sutures, I told him, “You have a melanoma.” “I figured it was something bad because a few people told me to have it seen. Just didn’t have time for it,” he told me. “You know, I’m on the phone from early morning on, and in the evening, I have to get out and socialize to get more clients.
It’s endless.”
“How long has it been on your back?” I asked.
“As far as I know, about 2 years,” Ted said. “Lately it’s been itching a lot. Am I gonna die?” he asked, a trace of worry in his voice. “This is serious,” I told him. “You have a chance of survival if you get this taken care of right away.”
Even before I sent the sample to the laboratory for diagnosis, I was fairly certain that he had melanoma. In melanoma, there are four basic warning signs, which can be recalled as ABCD: asymmetry (if a line was drawn through the middle, the two sides would not match), border (irregular in shape, with scalloped or notched edges), color (typically brown or black, and sometimes mixes of red, white, and blue), and diameter (larger than a quarter of an inch, the size of a pencil eraser). Ted’s tumor was asymmetrical with many areas of pigmentation, ranging from slightly pink to dark blue.
Melanoma arises because of accumulated DNA damage in a skin cell. The damage so deranges the cell’s ability to control its growth that it multiplies repeatedly. The early stages are classified by the tumor’s thickness and by how many layers of skin the tumor has invaded. The deeper the melanoma has advanced through the layers of skin, a measure known as Clark’s level of invasion, the more likely it is to be fatal. Ted had a Clark’s level stage III melanoma. That meant the melanoma had grown into the middle layer of the dermis but had not yet reached the deep dermis or subcutaneous fat.
In the past few years, great advances have been made so that the surgery for a safe and thorough melanoma removal requires removing much less tissue. With thin melanomas, outpatient procedures under local anesthesia are sufficient. Healing generally occurs in 1 to 2 weeks, and scars are minimal; however, when the melanoma has progressed beyond stage II, as in Ted’s case, the key question becomes this: Has the tumor shed cells and spread beyond the original site? If it has spread, the lymph nodes closest to the tumor are the most likely site of metastases. I hadn’t detected swelling of nodes in Ted’s armpits or neck, but that didn’t mean the tumor hadn’t spread. A new method, called lymphoscintigraphy, can precisely map the lymph system using a small amount of a radioactive substance injected at the site of the melanoma. With the help of a scanner, the path of lymphatic fluid draining from the melanoma to the nodes can be traced. The surgeon can examine the results and biopsy only the lymph nodes that are in line to receive lymph fluid from the melanoma. If the cancer is suspected to have spread widely, however, the physician may order more extensive scans, such as computed tomography scans or magnetic resonance imaging scans.
In Ted’s case, a preoperative evaluation included a complete blood count, a chest x-ray, and liver function studies to help rule out extensive metastases. A preoperative lymphoscintigraphy showed the presence of a tumor in the nodes in his armpits. Surgery was done to remove the melanoma and the affected nodes.
In stages III and IV disease, additional therapy may follow surgery. Several cancer drugs are used to treat melanoma. In addition, experimental melanoma vaccines are being studied. These vaccines are designed to boost the body’s defenses against an existing melanoma, and many are in clinical trials for patients with stages III and IV disease. Another experimental strategy is to treat patients with naturally occurring immune-system factors that discourage the tumor’s growth and spread.
I saw Ted 3 months later, and he expressed his appreciation and stated, “I didn’t realize what a mess I was in.” “You’re getting another chance,” I said. “Do I have a higher chance of another melanoma?” “Yes, the chances of having another melanoma are greater with a history of melanoma. You need regular checkups every 3 months for 3 years and then yearly for life,” I said. “With careful watching, most second melanomas are caught at an early stage and are treated by surgical excision.” “Is there a special melanoma diet?” “No, but you’ll do better keeping a well-balanced diet with folic acid, vitamins B6, B12, C, and A, and iron and zinc.” “Is it safe to donate blood?” “In most cases, blood centers will not accept blood from someone who has had cancer,” I said. “Should I avoid the sun?”
I explained that the Skin Cancer Foundation recommends that all people avoid the sun as much as possible, especially during the hours of 10 a.m. to 4 p.m. I told him to use a sunscreen with a sun protection factor of 15 or greater and to always wear a hat and sunglasses outdoors. People with a fair complexion, blue eyes, and blond hair are the most susceptible to melanomas, as are people with a history of blistering sunburns during childhood.
“I have a sister who ha before the age of 18 years. The younger a child is when the burns occur, the greater the risk.
Stay out of the sun. Use sunscreens with a sun protection factor of 15 or greater every day, and use mild antibacterial soaps and cleansers. You should wear sunglasses with ultraviolet protective coating and hats with brims wide enough to protect the head, ears, and neck. Special clothing that protects the skin from ultraviolet damage can be purchased. Remember that the ultraviolet light from tanning beds is equally dangerous. There is no such thing as a safe and glowing tan. Self-tanning creams provide an alternative if one feels a need for a tan. Remember that many medicines taken internally, such as tetracycline and estrogens, can increase your sensitivity to ultraviolet light and the chance of you burning your skin.
Many techniques are available for treatment of cancerous and precancerous lesions. Cryosurgery, the use of liquid nitrogen for treatment of abnormal skin lesions, has been used since the early 1900s. Whitehouse had an article published in the Journal of the American Medical Association in 1907 entitled “Liquid Air in Dermatology: Its Indications and Limitations.” A doctor named Torre came along in the 1960s and developed a practical apparatus to use liquid air in a spray form. It rapidly developed into the preferred method of cryosurgery for treating benign and malignant lesions. When I ask my nurse whether my guns are loaded, she knows that I refer to the canisters that I use to administer my liquid nitrogen therapy.
Like many dermatologists, I shoot them all day long. Liquid nitrogen is truly remarkable-using liquid at subzero temperatures to destroy tissue in a relatively easy manner. Destruction of malignant cells requires a temperature at least as cold as –50° centigrade. Not only does it seem magical to me that the liquid stays liquid at these temperatures, but the results can be amazing. How does it work? Cryosurgery targets the dermal–epidermal junction, providing separations some dark moles on her skin. Who should she see?”
“A dermatologist.” The studies show that general physicians don’t typically have enough experience to diagnose melanoma skin lesions with the same accuracy as dermatologists. Family members of a melanoma victim have a greater chance of getting melanoma and therefore should be checked also on a regular basis.
I have seen Ted now for more than 10 years since his melanoma surgery, and he continues to be melanoma free.
Term:
Lymphoscintigraphy – A diagnostic method used to identify lymphedema, the spread of cutaneous melanoma, and other diseases.
Studies have shown that the risk of developing skin cancer increases if children have three blistering sunburns before the age of 18 years
How do you prevent these cancers from growing and killing?
Children must be protected from harmful exposure to ultraviolet rays. Studies have shown that the risk of developing skin cancer increases if children have three blistering sunburns and removal of epidermal lesions. In simple terms, the nasty, unwanted growths usually blister and fall off. Some of the benefits compared with other surgery include very little, if any, bleeding, no additional anesthesia, low rate of wound infection, no sutures, a biopsy that can be done while the lesion is frozen, rapid healing, easiness, and quickness. Not bad. The skin is an amazing, versatile organ. We have good treatments for your skin ills. My advice, however, is to protect your skin and prevent skin cancers and other problems.
How often should I have an exam?
Every year on your birthday you should get your birthday suit checked. In addition to yearly skin exams by a dermatologist, the American Academy of Dermatology recommends self-exams every month as the best way to catch potentially cancerous skin conditions in the early stages.