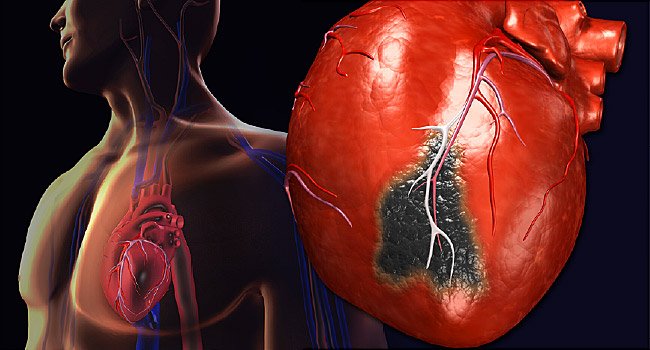
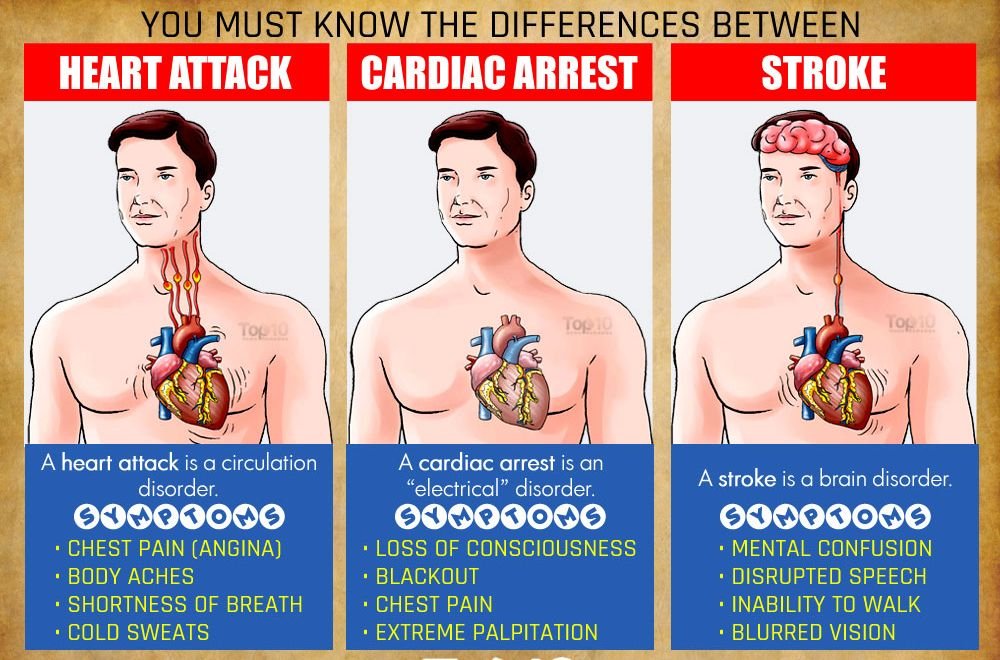
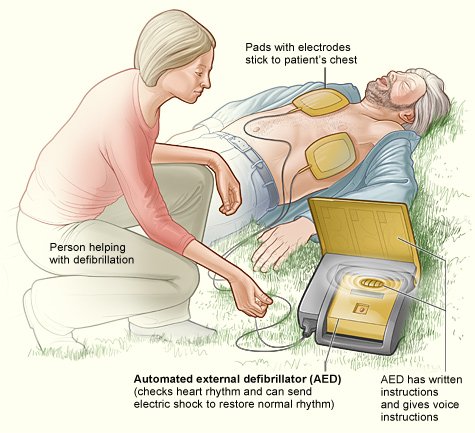
Heart Attacks and Heart Disease
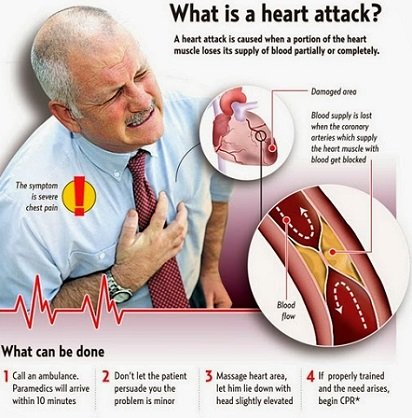
What is a coronary artery bypass graft, and when is it used?
A coronary artery bypass graft (CABG) is the major cardiac surgery performed most commonly in America and in all other civilized countries worldwide. CABG may be performed as an emergency operation, but it is performed more commonly as an elective surgery. Surgeons perform it when coronary angioplasty or thrombolytic therapy is not successful or is not appropriate. When CABG is scheduled (rather than as an emergency surgery), they usually do this a few days later to allow recovery of the heart muscle. A recent study showed that 1-year risk of death is reduced by more than 40% when coronary angioplasty or CABG is performed within 14 days after the onset of acute heart attack. The PTCA is initially successful in more than 90% of cases.
A CABG makes a bypass (detour) to reestablish blood circulation around the blocked segment of the coronary artery. Most commonly, a saphenous vein obtained from the leg is installed as a bypass vessel so that blood flow around the blockage from the aorta (the largest arterial trunk) to the coronary artery will be established. Less commonly, one or both internal mammary arteries (arteries in the chest wall, normally arising from branches of the aorta) are used for a CABG.
Doctors commonly perform a CABG to relieve a blocked left main coronary artery; a diffusely narrowed or blocked coronary artery; a disease involving multiple coronary arteries; and poor function of the left ventricle. In addition, a CABG also helps to overcome significant technical difficulty during PTCA, when PTCA is unsuccessful, and when there are serious complications during PTCA. Such complications might include rupture of the coronary artery, worsening of the blockage, and the occurrence of a new heart attack.
After a CABG, you would stay in the hospital for 1 week. You would need about 3 weeks for full recovery.
Is there an age limit or gender difference for CABG?
A coronary artery bypass graft is usually recommended for adults up to the age of 75 years. However, some older adults (80-85 years old) underwent CABG recently with successful outcomes. The outcome of CABG among women seems to be less favorable than that among heir male counterparts. That’s due to various reasons, such as some technical difficulty during CABG and the delayed diagnosis of coronary artery disease among women.
Are other kinds of heart surgery performed for heart attacks?
When any major complications of heart attack occur, a variety of heart surgeries might be necessary. In the event of mitral regurgitation (leaking back of blood flow from the left ventricle to the left atrium because of mitral valve dysfunction, physicians would replace the mitral valve with an artificial heart valve. When an acute heart attack produces a ventricular septal defect (formation of a hole in the ventricular septum between two ventricles, a surgeon would repair the hole immediately.
When a major complication, such as congestive heart failure (markedly diminished pumping action of the heart), persists or deteriorates in spite of all available therapy, you would need transplantation of a new heart or an artificial heart.
What is an artificial pacemaker, and when is it used?
When medications and varied medical or surgical treatments are not effective or appropriate, the resolution of certain medical conditions requires electrical treatment. One of two major electrical devices or methods is an artificial pacemaker. The other is the use of electrical shocks. An artificial pacemaker is a small, battery-operated device that regulates your heartbeat by imitating your natural heart rhythm arising from the sinus node (your natural pacemaker).
Some artificial pacemakers are permanent units (internal) implanted in the chest; others are temporary (external) units. Most artificial pacemakers have a sensing device that turns off when your natural heart rhythm is faster than the preset desired heart rate, and it turns back on when your heart rate becomes slower than that preset rate.
This type of artificial pacemaker is called a demand pacemaker. At present, almost all pacemakers are manufactured as demand pacemakers. The artificial pacemaker consists of two parts: the pulse generator and wires (insulated leads). The pulse generator is a small metal “can” that contains a battery and electrical circuitry (a computer). They regulate the rate of electrical impulses sent to your heart. The pulse generator is implanted in your chest, just below your collarbone in most cases. However, for cosmetic reasons, physicians can implant the pulse generator elsewhere (e.g., in the area between the upper chest wall and arm, or the armpit).
Newer models are much smaller and lighter than older models. The smaller models weigh less than an ounce and are about the size of three silver dollars sandwiched together. Their battery life is generally 6 to 7 years, but batteries may operate for up to 10 to 12 years. The pulse generator must be replaced periodically before the pacemaker batteries wear out.
A surgeon threads the pacemaker wires (insulated leads) through a large vein and into the heart, and these flexible wires are connected to the pulse generator. Thus, these wires deliver the electrical impulses from the pulse generator to the heart. Managing various slow heart rhythms primarily requires an artificial pacemaker, particularly for significant symptoms, such as dizziness and near-syncope or syncope, associated with these abnormal rhythms. Occasionally, treatment of advanced congestive heart failure (markedly diminished pumping action of the heart) also requires an artificial pacemaker.
Certain medical conditions require the use of an artificial pacemaker. For example, in the sick sinus syndrome, your natural pacemaker (the sinus node) is unable to produce sufficient heart impulses; that creates a very slow and unstable heart rhythm. In this disorder, slow heart rhythm often coexists with components of very rapid rhythms, such as atrial fibrillation or ventricular tachycardia. That leads to a combination of slow and rapid heart rhythms (called bradytachycardia.
In another condition, heart block (AV block), the interruption in conducting your heart impulse to your ventricles (lower chambers) causes a very slow heart rhythm. This interruption is the result of a block in the conduction system, commonly in the AV node.
Physicians may use biventricular pacemakers in some cases of advanced congestive heart failure. That’s the case when all available medications are not effective enough to relieve congestive heart failure. Biventricular pacemakers stimulate both the right and the left ventricles in a coordinated fashion so that the pumping action can be improved.
Are different pacing methods used?
In the past, all older artificial pacemakers were designed to set the pacing rate (and only one rate) to stimulate the heart, regardless of the patient’s needs and the heart’s functions. At present, however, almost all newer pacemakers are manufactured as demand pacemakers (it functions only when needed). In addition, most pacemakers are “rate-adaptive.” That means that they can be programmed to adjust the pacing rate to your activity level, mimicking your natural heart rhythm. The newer models can meet different pacing needs, depending on where the pacing leads are directed and the method of programming the pulse generator (computer).
In atrioventricular (AV) sequential pacing, the atria (upper chambers) and the ventricles (lower chambers) of your heart are paced sequentially, as the name of the pacing method indicates. In AV sequential pacing, the location of the pacemaker leads allows them to sense your heart’s activity and pace as needed: first in the atria and then in the ventricles, sequentially.
Dual-site atrial pacing is still in research. In this type of pacing, the pacemaker programs the leads to stimulate both the right and left atria (both upper chambers).
This type of artificial pacing may reduce episodes of atrial fibrillation (an irregular and usually rapid heart rhythm arising from upper chambers.
Biventricular artificial pacing stimulates both the right and left ventricles of your heart. Medical researchers consider this pacing method to be beneficial in improving the pumping action of the heart in patients with advanced congestive heart failure. Currently, all implantable defibrillators (used to shock a heart back into normal rhythm after sudden cardiac arrest or ventricular fibrillation) include artificial pacemaker functions.
Surgery for artificial pacemaker implantation usually requires no more than an overnight hospital stay. In most cases, local anesthesia is used. Before you’re discharged from the hospital, doctors program your artificial pacemaker to fit your heart’s needs. You would return after several months to allow your doctor to make more detailed adjustments to the pacemaker settings.
Term:
Ventricular septal defect – hole (abnormal communication) in the muscle wall between the ventricles, a common form of congenital heart disease and possibly caused by a heart attack; a life threatening complication.
Artificial pacemakers can be programmed to adjust the pacing rate to your activity level, mimicking your natural heart rhythm.