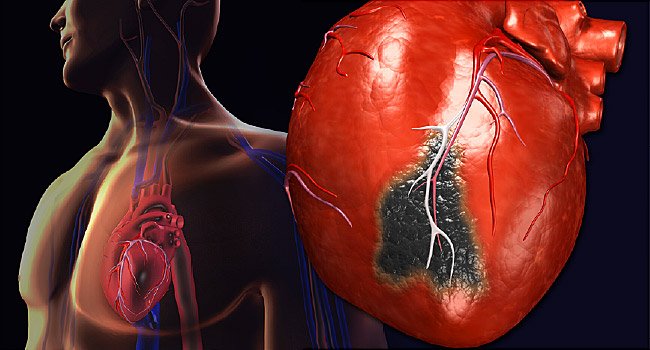
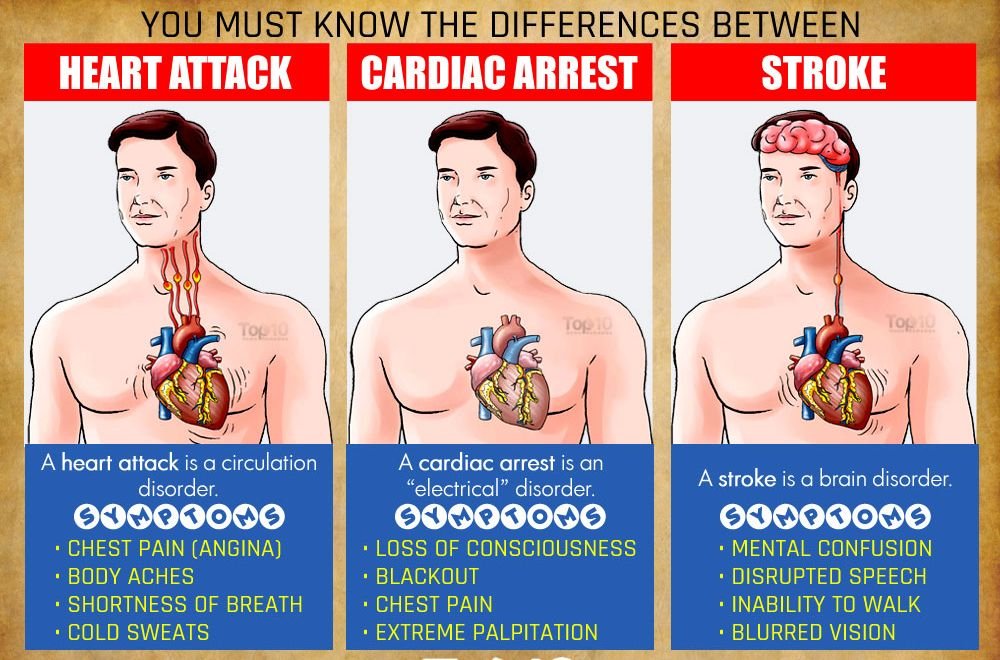
What Is a Pacemaker and How Does It Work? (Video)
Definition of Artificial pacemaker
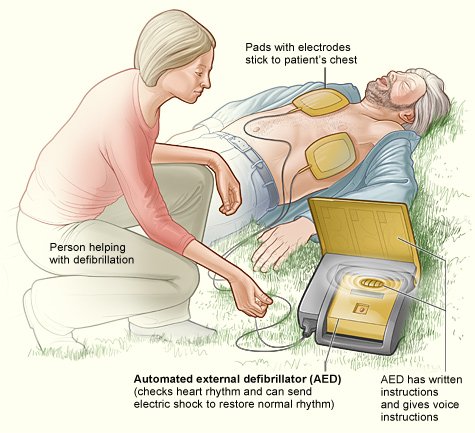
What are the limits and risks of artificial pacemaker functions?
If you receive an artificial pacemaker implantation, you should carry a wallet ID card showing information about your pacemaker. That’s because some equipment used by doctors and dentists can affect your artificial pacemaker functions and may cause it to malfunction. You will also need to show this card when traveling through airports, as the security equipment used to screen passengers should not be used on people with pacemakers.
Many surroundings and devices do not interfere with the function of your artificial pacemaker. They include CB radios, electric drills, electric shavers, electric blankets, heating pads, metal detectors, microwave ovens, TV transmitters, remote control TV changers, and cellular phones (less than 3 watts). Dental equipment does not appear to interfere with the pacemaker functions, but you might may feel an increase in pacing rates during dental drilling.
Electrical shock treatment (electroconvulsive therapy) for certain mental disorders does not appear to interfere with pacemaker functions. Likewise, diagnostic radiation (e.g., chest x ray) appears to show no interference in pacing functions. However, therapeutic radiation (e.g., treatment for certain cancers) may interfere with pacemaker circuits.
Magnetic resonance imaging (MRI) may interfere with your pacemaker functions. Therefore, you should discuss possible risks and benefits with your doctor before undergoing an MRI procedure. Research has shown, however, that radiofrequency (RF) ablation is safe for pacemaker function. RF is a special electrical treatment to manage a variety of arrhythmias (abnormal heart rhythms).
Performance of lithotripsy, a noninvasive treatment to destroy kidney stones, is safe for most pacemaker wearers. However, this treatment may interfere with certain kinds of pacemakers implanted in the abdomen. Also, transcutaneous electrical nerve stimulation to manage acute or chronic pain may interfere with pacemaker function in certain models.
By and large, you should discuss the safety of and possible interference with your pacemaker’s functions with physicians or dentists before the use of any medical device or equipment. Pacemaker implantation is a simple procedure involving little risk, and complications are rare.
Nevertheless, possible risks and complications do exist. For example, displacement of the pulse generator or the pacemaker wires (insulated leads) can cause problems. Such events as tearing or perforation of the vein or arterial wall or of your heart itself; puncture of the lungs, which would cause your lung to collapse; and blood clotting or air bubbles in your veins could lead to major medical problems. Other events that would affect your pacemaker include infection or nerve damage at the incision site, bleeding or severe bruising, or even malfunction of your artificial pacemaker itself.
What kind of care is necessary after a pacemaker implantation?
After having an artificial pacemaker implanted, every patient requires certain follow-up care. By and large, you can carry out all daily activities without limitation, but you should be familiar with your pacemaker. You need to understand certain precautions and possible risks after receiving a pacemaker.
You should carry a pacemaker ID card at all times; it should contain important information regarding your pacemaker. You would show your ID card to any doctor or dentist or other medical professional during each visit. It’s also a good idea to show the ID card to security personnel (e.g., in airports) as needed. Medical personnel can monitor your pacemaker’s functions and transmit them via the telephone using a special telephone transmitter. They connect the transmitter to wristbands on each of your arms, then place the telephone receiver on the transmitter and hold a special magnet over the pacemaker. A specially trained technician on the other end of the phone line checks your heart rate, heart rhythm, pacemaker battery level, and pacemaker functions. The pacemaker check-up via telephone transmitter can be carried out at the doctor’s office or at a pacemaker clinic.
Several times a year, you should have a medical checkup at your doctor’s office or at a pacemaker clinic. Almost all university or teaching hospitals have a special pacemaker clinic that specializes only in patients with permanent pacemakers. During each visit, technicians check the battery level and functions of your pacemaker and can adjust your pacemaker’s settings as needed. The pacemaker pulse generator should be replaced every 6 to 10 years, and the leads may have to be replaced occasionally. The pacemaker clinic also can perform the pacemaker check-up via a telephone transmitter.
You should take certain precautions after receiving your pacemaker. You must inform your physician immediately if any troubling symptoms or signs occur. For instance, you might notice the reappearance of symptoms that surfaced before your pacemaker was implanted. Or you might feel dizziness, near-syncope or syncope, shortness of breath, marked weakness, or any other symptoms related to heart disease. Additionally, you might develop fever or chills (or both), a very rapid or very slow heart rhythm (with or without palpitations), pain, infection, swelling, or bleeding in the area around your pacemaker, or a swelling of the arm near the incision site. It is vitally important to report any such irregularity at once.
What is electrical shock treatment, and who needs it?
There are several ways to manage a variety of cardiac arrhythmias (usually very rapid heart rhythms) with electrical energy. One such process is emergency electrical shock treatment (use of a defibrillator) for cardiac arrest due to ventricular fibrillation (very rapid, chaotic, and ineffective heart rhythm arising from the ventricles). Another is electrical shock treatment of rapid heart rhythms that don’t respond to drugs, such as atrial fibrillation (rapid and irregular heart rhythm arising from the upper chambers). Other devices are automatic external defibrillators (AEDs) and implantable cardioverter-defibrillators (ICDs).
Certain drug-resistant rapid heart rhythms require the use of catheter ablation (a nonsurgical technique that destroys parts of the abnormal conduction pathway causing the arrhythmia).
Emergency defibrillation is only a life-saving measure to treat ventricular fibrillation, and the electrical shock should be delivered within 4 minutes from the onset of arrest (ventricular fibrillation). If administered after that, it usually will not prevent a fatal outcome. Delay of shock treatment for more than 4 to 5 minutes often produces permanent brain damage, even if the heart rhythm returns to normal later. Termination of ventricular tachycardia (very rapid and regular rhythm arising from the lower chambers) also often requires emergency electrical shock treatment. This is especially true if medications are not effective and the arrhythmia is life-threatening. Treatment of cardiac arrest in heart attack victims usually calls for cardiopulmonary resuscitation (CPR) coupled with electrical shock treatment.
Terms:
Radiofrequency (RF) – ablation special electrical treatment to manage a variety of rapid heart rhythms.
Lithotripsy – noninvasive treatment to destroy kidney stones.
You should discuss the safety of and possible interference with your pacemaker’s functions with physicians or dentists.
You should visit your doctor or a pacemaker clinic several times a year.
Inform your physician immediately if any troubling symptoms or signs occur.