What Happens If You Eat Too Much or Too Little Protein?
While protein is essential to health and normal body function, eating too much or too little can be unhealthy. Let’s look at what happens to the human body when it gets too much or too little protein.
Eating Too Much Protein Can Mean Too Much Heart-Unhealthy Fat and Weaker Bones
As you read in the beginning of our texts, Melissa, the college student, had switched to a high-protein diet to help her slim down. Unfortunately, her steady diet of low-fiber, fat-rich cheeses, hamburgers, and fried foods was affecting her health. The lack of fiber-rich whole grains, fruits, and vegetables was causing her to become extremely constipated and giving her bellyaches. A diet high in saturated fat can raise the LDL (“bad”) cholesterol level in the blood. Before Melissa switched to a high-protein diet, her LDL cholesterol was in the healthy range. But her steady diet of fatty foods caused her LDL cholesterol to climb into the dangerously high range. Her doctor sent her to a registered dietitian (RD), who advised her to trim the fatty foods from her diet and add back the fiber-rich whole grains, fruits, and vegetables. Melissa’s cholesterol dropped to a healthy level within months, and the high-fiber foods helped to “keep things moving” in her intestinal tract and eliminate constipation. The RD also recommended that Melissa walks on campus between classes daily to help her better manage her weight.
Although consuming protein is a key to good health, eating more is clearly not necessarily eating better. In fact, a diet that is too high in protein is associated with the following risks:
Heart disease. A high-protein diet may increase your risk for heart disease and die prematurely from heart disease. Many foods rich in protein are also rich in heart-unhealthy saturated fats. Although lean meats and skinless poultry contain less saturated fat than some other cuts of meat, they are not completely free of saturated fat. Hence, a high protein intake can make a low saturated fat intake a challenge. Lowering the saturated fat in your diet is important in lowering your risk for heart disease.
Kidney stones. A high-protein diet may also increase your risk for kidney stones, which commonly contain calcium. More than 10 percent of Americans will likely suffer from a kidney stone at least once in their lives.
Osteoporosis. A high-protein diet may also increase your risk of osteoporosis (poor bone density). Although still a controversial issue, numerous research studies have shown that bones lose calcium when a person’s diet is too high in protein. The loss seems to occur because calcium is taken from bone to act as a buffer, offsetting the acid generated when specific amino acids are broken down. Other research has attempted to determine if calcium loss leads to osteoporosis when there is an adequate amount of calcium in a high-protein diet. If a higher dietary protein intake is coming from foods such as low-fat milk, yogurt, and cheese, it can add calcium to the diet. Unfortunately, many American adults are falling short of their recommended calcium intake. If their diets are also high in protein, this isn’t a healthy combination for their bones.
Cancer. A high-protein diet may increase your risk for cancer; however, this relationship is also less than clear. While large amounts of meat, especially red and processed meats, may increase the risk for colon cancer, research doesn’t necessarily support a connection between high amounts of total protein and increased colon cancer risk.
One final health concern surrounding a high-protein diet is the displacement of other foods. If your diet is overloaded with protein-rich foods, such as meat, fish, and poultry, they will likely crowd out another nutrient- and fiber-rich foods. As you know, a diet that contains high fiber and a wide variety of nutrient-dense foods can help you reduce your risk for several chronic diseases, such as cancer, heart disease, diabetes, and stroke. If you fill up on meat and milk at meals, you might be shortchanging yourself on foods, such as whole grains, fruits, and vegetables that contain disease-fighting compounds.
While many individuals have the luxury of worrying about consuming too much protein, others are desperately trying to meet their daily needs. Let’s look at the serious health implications of chronically eating too little dietary protein.
Eating Too Little Protein Can Lead to Poor Bone Health and Malnutrition
Eating too little protein can lead to many health problems, including compromised bone health. In fact, eating too little protein has been shown to lead to loss of bone mass. A study of more than 500 women over age 55 showed that higher dietary protein consumption was associated with more dense bone. Another study of more than 2,000 males and females ranging in age from 50 to 89 showed that those under the age of 70 who had a diet higher in protein had 65 percent fewer hip fractures compared with those with the lowest protein intake. When it comes to our bones, too much protein or too little can both be unhealthy.
Protein-Energy Malnutrition
Every day, almost 17,000 children around the world approximately 6 million annually-die because they don’t have access to enough food. These children’s diets are inadequate in either protein or calories or both, a condition is known as protein-energy malnutrition (PEM).When calories and protein are inadequate, dietary protein is used for energy rather than reserved for its numerous other roles in the body.
Moreover, other important nutrients, such as vitamins and minerals, also tend to be in short supply, which further compounds PEM. Many factors can lead to PEM, including poverty, poor food quality, insufficient food intake, unsanitary living conditions, ignorance regarding the proper feeding of children, and stopping lactation (nursing) too early. Because they are growing, infants and children have higher nutritional needs for their size than adults. They are also dependent on others to provide them with food. For these reasons, PEM is more frequently seen in infants and children than in adults.
Because protein is needed for so many functions in the body, it isn’t surprising that a chronic protein deficiency can lead to many health problems. For example, without adequate dietary protein, the cells in the lining of the gastrointestinal tract aren’t adequately replaced when they are routinely sloughed off. The inability to regenerate these cells inhibits their function. Absorption of the little amount of food that may be available is reduced, and bacteria that normally stay in the intestines can get into the blood and poison it, causing septicemia. Malnourished individuals frequently have a compromised immune system, which can make fighting even a minor infection, such as a respiratory infection or diarrhea, impossible. Malnourished children have died after exposure to measles as well as after bouts of diarrhea.
While deficiencies of both calories and protein often occur simultaneously, sometimes one condition may be more prevalent than the other. A severe deficiency of protein is called kwashiorkor, whereas a severe deficiency of calories is called marasmus. A condition that is caused by a chronic deficiency of both calories and protein is called marasmic kwashiorkor.
Kwashiorkor
Kwashiorkor was first observed in the 1930s in tribes in West Africa: often the firstborn child became sick when a new sibling became part of the family. Typically, the newborn displaced the first child, usually around 18 months of age, from his or her lactating mother and her nutritionally balanced breast milk. The first child was then relegated to an inadequate and unbalanced diet high in carbohydrate-rich grains but severely deficient in protein. This sets the stage for serious medical complications.
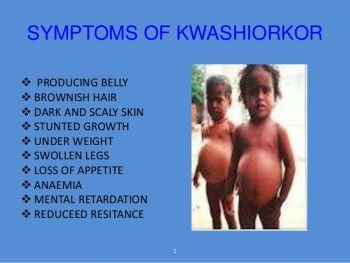
A classic symptom of severe kwashiorkor is edema in the legs, feet, and stomach. As we discussed earlier, protein plays an important role in maintaining fluid balance in the blood and around the cells. With protein deficiency, fluid accumulates in the spaces surrounding the cells, causing swelling. The body wastes away as the muscle proteins are broken down to generate the amino acids needed to synthesize other proteins. Consequently, muscle tone and strength diminish. Those with kwashiorkor often have skin that is dry and peeling. Rashes or lesions can also develop. Their hair is often brittle and can be easily pulled out. These children often appear pale, have facial expressions that display sadness and apathy, and cry easily. They are prone to infections, rapid heartbeats, excess fluid in the lungs, pneumonia, septicemia, and water and electrolyte imbalances-all of which can be deadly.
Marasmus and Marasmic Kwashiorkor
The bloating seen in kwashiorkor is the opposite of the frail, emaciated appearance of marasmus. Because they are not consuming enough calories, marasmic individuals are starving. They are often not even at 60 percent of their desirable body weight.Marasmic children’s bodies use all available calories to stay alive; thus, growth is interrupted. These children are weakened and appear apathetic. Many can’t stand without support. They look old beyond their years, as the loss of fat in the face one of the last places that the body loses fat during starvation causes the disappearance of a robust childlike appearance. Their hair is thin and dry and lacks the sheen seen in the hair of healthy children. Their body temperature and blood pressure are both low, and they are prone to dehydration, infections, and unnecessary blood clotting.
Individuals with marasmic kwashiorkor have the worst of both conditions. They often have edema in their legs and arms, yet have a “skin and bones” appearance in other parts of the body. When these individuals are provided with medical and nutritional treatment, such as receiving adequate protein, the edema subsides and their clinical symptoms more closely resemble that of a person with marasmus.
Appropriate medical care and treatment can dramatically reduce the 20 to 30 percent mortality rate seen among children with severe PEM worldwide. The treatment for PEM should be carefully and slowly implemented using a three-step approach. The first step addresses the life-threatening factors, such as severe dehydration and fluid and nutrient imbalances. The second step is to restore the individual’s depleted tissues by gradually providing nutritionally dense calories and high-quality protein. The third step involves transitioning the person to foods and introducing the physical activity. The only successful way to cure PEM is to eradicate it.
Message
A high-protein diet may play a role in increasing the risk of heart disease, kidney problems, and calcium loss from bone. Consuming too much protein from animal sources can increase the amount of heart-unhealthy saturated fat in your diet. Too many protein-rich foods in the diet can displace whole grains, fruits, and vegetables, which have been shown to help reduce many chronic diseases. A low-protein diet has also been shown to lead to loss of bone mass. PEM is caused by an inadequate amount of protein and/or calories in the diet. A severe deficiency of protein is called kwashiorkor; a deficiency of calories is called marasmus.
These conditions can be improved with proper food and treatment.
Figs are a sweet way to get some calcium. Five large figs provide more than 10 percent of many adults’ daily calcium needs.
Where’s the Protein and Saturated Fat in Your Foods?
While many foods, in particular, dairy foods and meats, can provide a hefty amount of protein, they can also provide a large amount of saturated fat. Choose nonfat and low-fat dairy foods and lean sources of meats and skinless poultry to enjoy your protein without consuming too much-saturated fat.
Terms:
Protein-energy malnutrition (PEM) – A lack of sufficient dietary protein and/or calories.
Kwashiorkor – A state of PEM where there is a severe deficiency of dietary protein.
Marasmus – A state of PEM where there is a severe deficiency of calories that perpetuates wasting; also called starvation.



