VIDEO
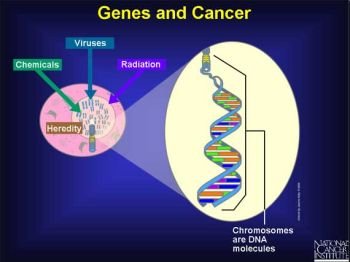
Why do family cancer genes lead to cancer?
Individuals with a family history of breast and/or ovarian cancer undergo testing of the genes BRCA1 and BRCA2 to determine if they contain mutations known to predispose to cancer.
Families with Li-Fraumeni syndrome may have breast cancer, sarcomas, brain tumors, leukemias, lymphomas, and adrenal cancers; members are tested for mutation in a gene called p53.
A family history of colon cancer as well as cancers of the endometrium (uterus), ovaries, duodenum, pancreas, and kidneys/ureters, may indicate the presence of Lynch syndrome or hereditary non-polyposis colon cancer (HNPCC); the genes MLH1, MSH2, and others will be
investigated for mutations.
Children who develop an eye tumor called retinoblastoma are tested for mutations in the gene Rb, the first inherited cancer gene identified.
Why do mutations in BRCA1 and 2, MLH1, p53, Rb, and other genes of this class increase the risk that cancer will develop? Because they are the caretakers and gatekeepers, DNA’s security system; their normal job is to repair DNA damage, keep it mistake-free, or stop a cell from surviving if its DNA is irreparably harmed. Their absence by mutation makes DNA unstable and prone to further damage, a situation termed genomic instability. Genomic instability creates a vicious cycle of mounting DNA damage that ultimately creates numerous genetic mutations inside a cell.
Although cancer is not a certainty, its risk is greatly increased. Defects in family cancer genes thus set the stage for cancer to develop. Their presence from conception accounts for the earlier age of onset of cancer in individuals who harbor them.
Who should be tested?
In general, genetic testing is recommended for those with a personal or family history indicating that a family cancer gene may be present.
Some of these indicators are:
1. Cancer diagnosed before the age of fifty;
2. Multiple family members affected by cancer;
3. Two or more cancers in any individual;
4. Breast cancer diagnosed in a man;
5. The same type of cancer in a close relative (for example, sisters with breast cancer or a father and daughter with pancreatic cancer); and
6. Clustering of cancers in one family that are known to be caused by the same genetic mutation, such as breast/ovarian/pancreatic or colon/uterine/ovarian cancers.
These and other features of a family medical history are tip-offs that a family may have a hereditary predisposition to cancer. One or more members may then be asked to consider giving a blood sample so that their DNA can be tested for mutations in the specific genes associated with the types of cancer occurring in the family.
Testing Saves Lives
The main reason to find a family cancer gene is to save lives. Individuals who possess the mutant gene can undergo earlier and more frequent cancer screening tests aimed at early detection, such as breast MRI and colonoscopy. Some may be advised, or elect themselves, to remove the organs at high risk in order to prevent cancer from developing.
Healthy persons at increased risk can consider taking medications to reduce their chances of developing specific cancers, such as: (1) tamoxifen and raloxifene to prevent breast cancer; and (2) finasteride to prevent prostate cancer, although it has not received FDA approval for this purpose (it is approved for the treatment of benign prostatic hypertrophy, or BPH). Women at increased risk for breast cancer and men at increased risk for prostate cancer (including all men aged fifty-five and older) should discuss the risks and benefits of taking these medications with their physicians.
If you know that you are a carrier of a family cancer gene, then you can be proactive in finding ways to prevent or better detect cancer.
High-risk individuals are also encouraged to participate in clinical trials aimed at finding better ways to prevent cancer. This is a dynamic field, with new studies and recommendations coming frequently. These issues should be discussed with appropriate health care professionals. On the other hand, if a family harbors a mutant cancer gene, then those members who test negative for the mutation (do not have it) can be relieved of the anxiety of believing themselves to be at high risk for cancer. They can follow routine cancer screening guidelines and would not be advised to undergo preventative surgery or other intensive measures to avoid cancer.
It is important to realize that not all families with a clear history of a family cancer will be found to have a gene mutation. This is not because the genes are not present but rather because not all the family cancer genes are known. Such families should be referred to an appropriate center that is working to identify new family cancer genes. Family members should continue high-level surveillance approaches to detect cancer as early as possible.
Getting yourself genetically tested for cancer is understandably a process fraught with emotion. There are many medical, psychological, and practical aspects to consider when performing these tests. For example, some individuals from a high-risk family avoid being tested because they fear they will be advised to have an organ removed to prevent cancer; others may feel guilty if it is discovered that they do not harbor a mutant gene but their siblings do. Some decline counseling because they fear health insurance or employment discrimination (a genetic nondiscrimination bill was signed into law in the United States in 2008). For these and many other reasons, intensive education and counseling is provided before genetic testing is performed.
Through a process called informed consent, all possible outcomes of genetic testing are discussed ahead of time, as are the psychological, medical, and financial ramifications of the test results.
Your genetic counselors, physicians, family, and support systems will help you decide on the best course of action to take following the results of genetic testing. Each individual’s personal preferences are always paramount.
Does family history matter in sporadic cancer development?
When multiple members of a family are affected by the same type of cancer, the probability of a family cancer gene is high and the importance of the family DNA is clear. But consider the majority of cancer patients who either lack a family clustering of similar cancers or who may have several members affected by different cancers. Is their family history of any importance? Does a family’s DNA influence cancer development in the commonly occurring sporadic cancers, or does cancer affect most of us randomly, without regard to our genetic constitution?
Answers to these questions have only recently come to light. Large studies of the populations of Utah, Sweden, and in particular Iceland, where nearly all cancer cases since the eighteenth century have been accurately catalogued, have shown that many cancers tend to cluster in particular families. They do not affect the population randomly.
Nearly all the common cancers, and even the less common cancers (such as thyroid and testicular), are found more frequently not only in the nuclear family but also in third-, fourth-, and fifth-degree relatives in some families. Even a cancer such as lung cancer affects some families more than others, separate from the effects of smoking. Moreover, a tendency to develop cancer in general (different types of cancer), rather than only one or two types, has been found in some families.
The increase in cancer risk to members of families with different types of sporadic cancers is much less than the risk associated with inherited cancer genes, such as a mutant BRCA1. Yet these findings show that one’s family history is important and that a person’s family DNA undoubtedly influences the development of even sporadic cancers. The specific genes that may cause family clustering of sporadic cancers are unknown at this time. An oncologist, therefore, could not recommend that genetic testing be done on individuals whose families have a variety of sporadic cancers because the tests have not yet been developed to detect the culprit genes. In contrast to the leading role played by a family cancer gene to cause a hereditary family cancer, it is believed that many different genes are each playing a “bit part” to collectively bring about a sporadic cancer. Some of these genes may be gatekeepers, others caretakers, and still others genes that help the body detoxify carcinogens in the environment. Discovering these genes is extremely important if we are to understand why most cancers develop. It is also an arduous task that will be accomplished only through painstaking and innovative research.
Summary
Whether a cancer is inherited or sporadic, the types of genetic mutations that give rise to it are similar. Both types of cancers have mutations in genes important to the growth, spread, and survival of cancer. Although some mutations are inherited and give those individuals a “head start” on cancer, most occur after birth and affect the general population later in life. This is the current expert view of cancer’s development and of its dependence on changes to DNA.