VIDEO
The Devastating Effects of Hypoglycemia

Hypos
Since my wife has been started on insulin she has had funny turns. What is the cause of this?
Your wife’s funny turns are likely to be due to a low blood glucose level. The medical term is hypoglycaemia that most people call ‘hypo’ for short.
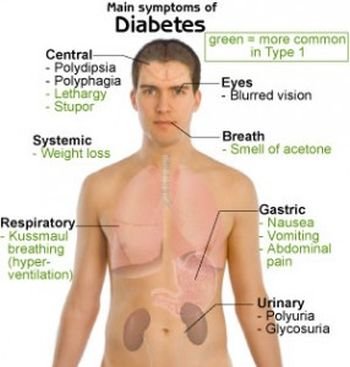
When the blood glucose level falls below a certain level (usually3 mmol/litre), the brain is affected. Highly dependent on glucose, the brain stops working properly and begins to produce symptoms such as weakness of the legs, double or blurred vision, confusion, and headache and, in severe cases, loss of consciousness and convulsions. Hypoglycaemia will also trigger the production of adrenaline, an hormone that will be responsible for causing sweating, rapid heartbeat and feelings of panic and anxiety.
Symptoms of hypo in groups
Cause – Symptom
Due to adrenaline response – Sweating
Pounding heart
Shaking/trembling
Hunger
Anxiousness
Tingling
Due to brain lack of glucose – Confusion/difficulty in thinking
Drowsiness/weakness
Odd (stroppy) behavior
Speech difficulty
Non-specific- Nausea
Headache
Tiredness
Children often describe a ‘dizzy feeling’ or just ‘tiredness’ when they are hypo. Most people find it hard to describe how they feel when hypo but the proof is that the blood glucose is low. If there is any doubt about the accuracy of your meter readings, it is always safer to take glucose or sugar if you’re feeling odd.
What is the best thing to take when I have a hypo?
This very much depends at which stage you recognize the hypo is developing. In the early stages the best treatment would be to have a meal or snack if one is due; or an extra snack such as a fruit, sandwich, or biscuits if there is some time before your next meal.
If your hypo is fairly well advanced then you need to take some very rapidly absorbed carbohydrates. This is best taken as sugar, sweets, or fruit juice or, for even greater speed, a sugary drink such as ordinary (not ‘diet’) Coke, lemonade, or Lucozade. Good things to carry in your pocket are also glucose tablets such as Dextro-Energy as they are absorbed very quickly. (Three tablets of Treatment with insulin listed above Symptoms of hypo in
Dextro-Energy contains 10 g of glucose). They are also less likely to be eaten when you are not hypo than ordinary sweets! Do not forget to eat some bread, biscuits, or a small sandwich after the sugar or sugary drink!
I am taking soluble and isophane insulin twice a day and I am getting hypos 2 to 3 hours after my evening meal. As I live alone this has been worrying me. What can I do?
Anyone who is having frequent hypos at a particular time of day can easily put this right by adjusting their insulin dose. In this case, you are having hypos at the time when your evening dose of soluble insulin is working. You should reduce the amount of soluble insulin you take in the evening until you have stopped having hypos at that time. On the other hand, hypos before your evening meal could be corrected by reducing your morning dose of intermediate-acting (isophane) insulin.
My teenage daughter has diabetes and sometimes turns very nasty and short-tempered. Is this due to the insulin?
Yes, probably – although it is not the only cause of bad moods in teenagers! The only way to find out is to try to persuade her to have a blood glucose measurement during her bad moods. If it is low (3 mmol/litre or less) she is then experiencing a hypo and some glucose should restore her good nature. Because the brain is affected by a low blood glucose level, irrational behaviour is common during a hypo. Your daughter may forcibly deny that she is hypo and resist taking the glucose her body needs. If you are firm and do not panic you will be able to talk her into taking the glucose (Lucozade, lemonade, or Coke can be useful here) and she will soon be back to normal. Children and adults can also become irritable if their blood glucose is very high.
My 8-year-old son often complains of feeling tired after recovering from a hypo. Is this usual and what is the best way to overcome it?
It is unusual to feel tired for more than 30 minutes after a hypo but, if your son does so, you should first check his blood glucose. If this is more than 4 mmol/litre you will just have to let him rest until he is back to normal. It is not uncommon for hypos to trigger headaches and migraine attacks, which may be the problem here.
My teenage son refuses to take extra carbohydrate when he is hypo and insists that we let him sleep it off. Is this all right?
Hypos should always be corrected as quickly as possible. Your son is right in thinking that the insulin will eventually wear off and that his blood glucose will return to normal. However, if his blood glucose falls to very low levels, it could cause problems, and he may even become unconscious. His refusal to take sugar is part of the confusion that occurs during a hypo and, if he can be persuaded to take glucose, he will get better more quickly.
I have been taking insulin for 38 years and my hypos have always been mild. Recently I suffered two blackouts lasting a minute, which I presume were hypos. Why has this started?
Blackouts tend to occur in children who have not yet learned to recognize the warning signs of a hypo but, on rare occasions, anyone on insulin can be caught unawares and have a sudden hypo, which makes them black out. Sometimes as people get older the ‘adrenaline’ warnings of a hypo fail to operate. This failure may be due to the natural ageing process or to damage (caused by diabetes) of the involuntary nerve supply which transmits the warning signs. Recent studies have suggested that keeping blood glucose levels above 4 mmol/litre can help to restore lost hypo warnings. ‘Make 4 the floor’ is the advice given. A number of people have also reported that after changing to human insulin they have less warning of hypos. So far there is no explanation for this.
I have recently lost my warning signs for hypos. Is it likely that they will return?
Very tight diabetic control is known to reduce hypoglycaemic awareness. In a study carried out with the help of people who had lost their warning symptoms, the results showed that when they ran their blood glucose control so as to prevent low glucose levels altogether for 3 months, partial or complete restoration of warning symptoms was experienced by everyone who had managed to avoid dropping to blood glucose levels of 4 mmol/litre or less. Do you think that you may fall into this category? If so, it may be worth discussing this with your diabetes team and reducing your dose of insulin.
My father has had diabetes for 20 years. Recently he had what his doctor calls epileptic fits. Would you tell me how to help him and if there is a cure?
A bad hypo may bring on a fit and it is important to check your father’s blood glucose during an attack. If the glucose level is low then reducing his insulin should stop the fits. If the fits are not due to a low blood glucose level, it should be possible to control them by making sure he takes his tablets regularly – ask his doctor for more details about these.
Can insulin reactions eventually cause permanent brain damage?
This question is often asked and is a great source of anxiety to many people. The brain quickly recovers from a hypo and there is unlikely to be permanent damage, even after a severe attack with convulsions. Very prolonged unconscious for days on end then the brain will not recover completely. This is not likely to occur in people with diabetes, in whom the insulin wears off after a few hours.
I have heard that there is an opposite to insulin called glucagon. Is this something like glucose and can it be used to bring someone round from a hypo?
Glucagon is a hormone which, like insulin, is produced by the pancreas. It causes glucose to be released into the bloodstream from stores of starch in the liver. Glucagon can also be injected to bring someone round from a hypo if they are too restless to swallow glucose, or unconscious. Glucagon cannot be stored in solution like insulin. It comes in a kit containing a vial with glucagon powder plus a syringe and sterile fluid for dissolving the powder. The process of dissolving the glucagon and drawing it into the syringe may be difficult especially if you are feeling panicky. It is worth asking the diabetes specialist nurse to show you and your likely helper how to draw up glucagon.
It is usually stated that glucagon only has a short-lasting effect and it is therefore important to follow it up with some sugar by mouth to prevent a relapse of coma. However, in children the blood glucose level may rise very high after an injection of glucagon and, as they often feel sick, it seems silly to force more sugar down them. It is best to do a blood test to help decide whether more glucose is really needed immediately. More sustaining carbohydrates (such as bread or biscuits) should be given as soon as they feel well enough to eat, as the blood glucose level can fall again later.
When I gave my wife a glucagon injection recently, she vomited. Is this normal?
Some people do vomit when regaining consciousness after a glucagon injection, particularly children. If only half the content of the vial is given (0.5 mg), it will usually be enough to correct the hypo, but less likely to cause sickness.
My diabetes was controlled by tablets for 20 years but 2 years ago my doctor recommended that I begin insulin treatment. I am well controlled but my sleep is often disturbed by dreams, or I wake up feeling hungry. Can you advise me what to do if this happens?
You may be going hypo in the middle of the night. It has been shown that many people have low blood glucose in the early hours of the night and, provided that they feel all right and sleep well, this probably does not matter. However, if you are regularly waking up with hypo symptoms (such as hunger) or having nightmares, you should first check whether you are hypo by measuring your blood glucose level at around 3.00am when your blood glucose is usually the lowest. If the reading is below 4 mmol/litre you need to reduce your evening dose of intermediate-acting insulin. If your blood glucose is then high before breakfast the next day, an injection of intermediate-acting insulin taken before going to bed instead of before your evening meal may solve your problem.
What can I do if my son has a bad hypo and is too drowsy to take any glucose by mouth?
You should try giving him Hypostop. This is a jelly loaded with glucose, which comes in a container with a nozzle. It can be squirted onto the gums of someone who is severely hypo and often leads to recovery within a few minutes. Hypostop is available on prescription from your doctor. If Hypostop fails, you should try injecting your son with glucagon – there are some questions about glucagon above.
Am I correct in thinking that only people on insulin can have hypos?
No. Some of the tablets used for treating Type 2 diabetes can also cause hypos. The commonly used ones are glibenclamide (Euglucon, Daonil) and gliclazide (Diamicron). These hypos will improve with glucose in the normal way but, because the tablets have a longer action than insulin, the hypo may return again after several hours. Anyone having hypos on tablets probably needs to reduce the dose. Metformin and the glitazones, however, do not cause hypos.
My diabetes is treated by diet alone and I have headaches and a light-headed feeling around midday if I have been busy in the morning. I am all right after eating something.
Why is this?
It seems surprising but some people on diet alone can go hypo if they go without food. This is because they produce their own insulin, but too late and sometimes too much. Ideally you should try to arrange a blood glucose measurement at a time that you feel odd in order to prove that you are actually hypo. If so, you could avoid the problem by eating little and often, especially on days when you are busy.
My daughter aged 21 takes insulin for her diabetes and is moving down to
By the age of 21 your daughter will be ready to be independent and live in a flat by herself. All parents worry when their children leave home, and diabetes adds to their anxiety, but sooner or later young people have to lead separate lives. We know that night hypos are common and that people either wake up or sort themselves out or else their blood glucose returns to normal as the insulin wears off and they wake up next morning unaware of any problem. However, there has been a handful of cases when people on insulin are found unexpectedly dead in bed, and possibly some of these cases are due to hypoglycaemia. This must be a cause of concern but considering the hundreds of thousands of people on insulin, the risk of this tragedy is equivalent to being struck by lightning and young people on insulin have a right to independence.
Your daughter should be aware of the risk of hypo when driving or swimming and be encouraged to tell her close friends and companions about diabetes. They should be told that, if she ever behaves oddly, she must be given some form of sugar, even if she protests. People often fail to take this simple precaution; it can avoid a lot of worry to their friends who may find them hypo and yet have no idea how to help.